Professional Documents
Culture Documents
The Optic Nerve
Uploaded by
Edwin Darmawan0 ratings0% found this document useful (0 votes)
116 views7 pagesopt nerve
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentopt nerve
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
116 views7 pagesThe Optic Nerve
Uploaded by
Edwin Darmawanopt nerve
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 7
The Optic Nerve
Optic Nerve Head Edema Often Reflects Increased Intracranial Pressure
Optic nerve head (optic disc) edema refers to a swelling of the optic nerve head where it
enters the globe. Optic nerve head edema can result from various causes, the most important
of which is increased intracranial pressure. The term papilledema, which is still widely used
in that context, is imprecise because no optic papilla exists.
Other important causes of optic nerve head edema are (1) obstruction to the venous drainage
of the eye (as may occur with compressive lesions of the orbit), (2) infarction of the optic
nerve (ischemic optic neuropathy), (3) inflammation of the optic nerve close to the eyeball
(optic neuritis, papillitis), and (4) multiple sclerosis.
Edema of the optic nerve head is characterized clinically by a swollen optic disc that displays
blurred margins and dilated vessels (Fig. 29-15). Frequently, hemorrhages (Fig. 29-16),
exudates, and cotton-wool spots are seen, and concentric folds of the choroid and retina may
surround the nerve head.
Acutely, optic nerve head edema results in few if any visual symptoms. As the condition
becomes established, swelling of the optic nerve head enlarges the normal blind spot. After
many months, atrophic changes lead to a loss of visual acuity.
Rubbin pathology
FIGURE 29-15. Chronic papilledema. The optic nerve head is congested and protrudes
anteriorly toward the interior of the eye. It has blurred margins, and the vessels within it are
poorly seen. In contrast to acute papilledema, the veins are not so congested, and hemorrhage
is not a feature.
FIGURE 29-16. Hemorrhage in papilledema. The optic nerve head is markedly congested,
with dilated veins and a blurred margin. A small hemorrhage is evident within the optic nerve
head at its junction with the retina. Several small cotton-wool spots are present within
the adjacent retina.
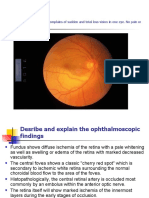
Figure 11-26 The left ocular fundus as seen with an ophthalmoscope.
An increase in CSF pressure slows venous return from the retina, causing edema of the retina (fluid
accumulation). The edema is viewed during ophthalmoscopy as swelling of the optic disc, a condition
called papilledema. Normally, the disc is flat and does not form a papilla. Papilledema results from
increased intracranial pressure and increased CSF pressure in the extension of the subarachnoid
space around the optic nerve (Fig. 7.50A).
Moore
Etiologi
The swollen disc (Figure 14.2 ) is an important and often worrying sign.
Papilloedema is the term given to disc swelling associated with raised
intracranial pressure (ICP), accelerated hypertension and optic disc ischaemia.
Papillitis , a condition with a similar fundoscopic appearance, is due to optic
neuritis (infl ammation) affecting the nerve head. Visual loss always occurs with
optic neuritis but is uncommon with the papilloedema of hypertension
and/or raised intracranial pressure; it is, however, a feature of ischaemic
papilloedema.
The differential diagnosis of disc swelling is shown in Table 14.1 . Some
normal optic nerve heads may appear to be swollen, due a crowding of nerve
fi bres entering the disc. This is termed pseudopapilloedema and occurs
particularly in small, hypermetropic eyes where the nerve entry site is reduced
in size. Note also that myelinated nerve fi bres occurring on the nerve head may
be mistaken for optic disc swelling. During development, myelination of the
optic nerve begins proximally and spreads centrifugally to be completed at the
lamina cribrosa at term. Occasionally, as a developmental variant, the process
extends into the peripapillary retinal nerve fi bre layer as a patch of light -
scattering, myelinated fi bres; the normally unmyelinated retinal nerve fi bre
layer is partly myelinated, giving it a feathery, white appearance which refl ects
the organization of the nerve fi bre layer.
In myopia it is common to see a pale
myopic crescent of peripapillary atrophy, at the temporal margin of the optic
disc. In high myopia the optic disc may be surrounded by such an atrophic area
( peripapillary atrophy ), which may be confused with disc swelling.
History
The crucial feature of disc swelling due to raised intracranial pressure is that
there is rarely an associated visual loss, although some patients, with advanced
papilloedema, may develop fl eeting visual loss lasting seconds when they alter
posture from lying to standing ( obscurations of vision).
Other important clues to the presence of raised intracranial pressure include:
headache, worse on waking and made worse by coughing;
nausea, retching;
diplopia (double vision), usually due to a sixth nerve palsy;
other neurological signs, if the raised pressure is due to a cranial space -
occupying lesion visual fi eld loss; cranial nerve palsy;
a history of head trauma suggesting a subdural haemorrhage;
a history of medications sometimes associated with raised intracranial pressure
(e.g. oral contraceptives, tetracyclines).
Signs
The optic disc is swollen, its edges are blurred and the superfi cial capillaries
are dilated and thus abnormally prominent. There is no spontaneous venous
pulsation of the central retinal vein. This has a physiological basis. The central
retinal vein is exposed to cerebrospinal fl uid (CSF) as it leaves the optic nerve
to join the veins of the orbit. Normally, venous pressure in the retinal veins
at the nerve head is just above ocular pressure. Venous pulsation occurs
because the vein collapses briefl y with each rise in ocular pressure with arte-
rial infl ow. When the CSF pressure is higher than the ocular pressure, as
occurs in papilloedema due to raised intracranial pressure, the pressure in
the veins at the disc rises above the ocular pressure and so spontaneous
venous pulsation is lost. Absence of spontaneous venous pulsation is seen in
5 20% of those with normal nerve heads, but in this case venous collapse at
the nerve head can be induced by light pressure on the globe.
A large blind spot will be found on visual fi eld testing, corresponding to the
swollen nerve head. In chronic papilloedema the fi eld may become constricted.
A fi eld defect may, however, be caused by the space - occupying
lesion causing the papilloedema.
Abnormal neurological signs may indicate the site of a space - occupying
lesion.
Investigation
CT and MRI scanning will identify any space - occupying lesion or enlargement
of the ventricles. Following neurological consultation (and normally after a
scan) a lumbar puncture will enable intracranial pressure to be measured.
Treatment is dependent on fi ndings.
Lecture note ophtalmo
The retina is the innermost layer, or "camera film," of the eye. The retina is attached firmly to
the underlying choroid at the optic nerve posteriorly and at the ora serrata anteriorly. Between
these two points, the retina is in contact with the choroid but it is not attached. The ora serrata
is the junction of the retina and ciliary body. The retina is only 0.4 mm in thickness and is
thinnest in the region of the macula. Histologically, the retina is made up of 10 distinct layers.
Basically, the retina senses light through the rods and cones in its outer layer (closest to the
RPE), performs initial signal processing in its middle layer, and encodes and transmits the
data in its inner layer, the nerve fiber layer. The nerve fiber layer is directly under the inner
limiting membrane of the retina, the layer closest to the vitreous. These nerve fibers course
along the inner portion of the retina and aggregate to form the optic nerve. On leaving the
eye, the nerve fibers become myelinated.
Within the retina are several important structures: the optic disc, the retinal vessels, and the
macula. Figure 10-8 illustrates the retina of the left eye.
The optic disc is located at the nasal aspect of the posterior pole of the retina. This is the head
of the optic nerve, from where the nerve fibers of the retina exit the eye. The optic disc is 1.5
mm in diameter and is ovoid. It is lighter than the surrounding retina and appears yellowish-
pink. The disc margins are sharp with some normal blurring of the nasal portion. African-
American patients may have pigmentation at the margins. The physiologic cup is the center
of the disc, where the retinal vessels penetrate. This small depression normally occupies
about 30% of the disc diameter.
The retinal vessels emerge from the disc and arborize on the retinal surface. The arteries are
brighter red and thinner than the veins. An artery-to-vein ratio of 2:3 is normal.
Textbook physic diagnosis
PAPILLOEDEMA PAPILLITIS
Visual Acuity Normal (usually) Reduced
Pupil Normal Poor response to
direct light
Visual Field Normal (increased Central scotoma
blind spot) or field defect
Colour Vision Normal Defective
Usually Usually
bilateral unilateral
The ophthalmoscopic appearance of disc oedema in papilloedema
and papillitis is the same. Papilloedema is differentiated from papillitis
by the presence of other clinical features.
Papilloedema is a passive swelling of the optic disc commonly
caused by raised intracranial pressure. The condition is usually
bilateral. Vision is normal unless the macula is affected by oedema
or exudates. Rarely is the vision diminished because of optic atrophy
in severe unrelieved papilloedema. The visual fields and colour vision
are also normal although the blind spot is sometimes enlarged. The
pupillary reflex to light is normal.
Papillitis is an inflammation of the optic nerve, frequently of
uncertain aetiology. Disseminated sclerosis is an important cause.
The condition is usually unilateral. Because the optic nerve is
inflamed, there is usually marked visual loss. A central scotoma is
present and the eye may have defective colour vision, especially to
red. The pupil is dilated, with sluggish or no reaction to direct light.
Ischaemic optic neuropathy
Ischaemia to the optic nerve head from arteriolar sclerosis and
temporal arteritis also causes sudden visual loss with a swollen optic
disc in the elderly population. It is important to exclude temporal
arteritis by blood erythrocyte sedimentation rate (ESR). Systemic
steroids will protect the unaffected eye. The prognosis for the affected
eye is usually poor and optic atrophy usually follows.
papilloedema
Pseudo-papilloedema is a variation in the appearance of the optic
disc which is sometimes mistaken for true disc oedema. It should be
clearly differentiated from the latter in order to avoid unnecessary
investigations and anxiety to the patient.
One common cause of pseudo-papilloedema is hypermetropia
where the disc margin is blurred. Other common causes include
drusen (yellowish-white deposits at the optic disc) and opaque
myelinated nerve fibres. Fundal fluorescein angiography can help to
distinguish pseudo-papilloedema from true disc oedema.
Color atlas ophthalmology
OCULAR MANIFESTATIONS
Papilledema is observed on fundus examination, by direct or indirect
ophthalmoscopy. Indirect ophthalmoscopy with a 20 D lens provides a
better stereoscopic view. A 90 D lens used in conjunction with biomicroscopy
provides excellent magnification and stereopsis. It is useful to
characterize the changes in the optic nerve head that occur in papilledema
as being mechanical or vascular in nature.
The five mechanical clinical signs of optic disc edema are:
Blurring of the optic disc margins.
Filling in of the optic disc cup.
Anterior extension of the nerve head (3 D = 1 mm of elevation).
Edema of the nerve fiber layer.
Retinal or choroidal folds, or both.
The five vascular clinical signs of optic disc edema are:
Venous congestion of arcuate and peripapillary vessels.
Papillary and retinal peripapillary hemorrhages.
Nerve fiber layer infarcts (cotton-wool spots).
Hyperemia of the optic nerve head.
Hard exudates of the optic disc.
In addition, elements of optic disc swelling can be used to help characterize
the papilledema as early, fully developed, chronic, or late.
In early papilledema, disc hyperemia, disc swelling, blurring of the disc margins, and blurring of the nerve fiber layer are
found (Fig. 9-6-1).
In fully developed papilledema, gross elevation of the optic nerve head and engorged and dusky veins appear, peripapillary
splinter hemorrhages and sometimes choroidal folds arise, and retina striae are seen (Fig.
9-6-2).
In chronic papilledema, fewer hemorrhages occur, the optic disc cup is obliterated completely, less disc hyperemia is seen,
and hard exudates occur within the nerve head (Fig. 9-6-3).
In late disc edema, secondary optic atrophy occurs, disc swelling subsides, retinal arterioles are narrowed or sheathed, and
the optic disc appears dirty gray and blurred, secondary to gliosis (Fig. 9-6-4).
1. Rubin R, Strayer DS, Rubin E. Rubin's Pathology: Clinicopathologic Foundations of Medicine:
Wolters Kluwer Health/Lippincott Williams & Wilkins; 2011.
You might also like
- Sudden Loss of Vision & Optic NeuropathyDocument30 pagesSudden Loss of Vision & Optic NeuropathyIshak IzharNo ratings yet
- MCQ OphthalmologyDocument206 pagesMCQ OphthalmologyMohammed Mousa Imran100% (4)
- Lesson Plan On CataractDocument8 pagesLesson Plan On Cataractsimonjosan88% (8)
- St. Victoria Hospital Nursing Service Ward DeptDocument50 pagesSt. Victoria Hospital Nursing Service Ward DeptPat MagpaliNo ratings yet
- Diseases of The Optic Nerve 09Document25 pagesDiseases of The Optic Nerve 09somebody_maNo ratings yet
- Optic Nerve: Applied AnatomyDocument10 pagesOptic Nerve: Applied AnatomyMariam QaisNo ratings yet
- Proiect Nerv OpticDocument7 pagesProiect Nerv Opticiuliabucur92No ratings yet
- DEJ5 Online 2Document15 pagesDEJ5 Online 2Cecilia Fany GunawanNo ratings yet
- Pe in Raised IcpDocument15 pagesPe in Raised Icplydia_chandraNo ratings yet
- Differential Diagnosis of Papilledema - UpToDateDocument28 pagesDifferential Diagnosis of Papilledema - UpToDateDaniel PadillaNo ratings yet
- Papiledema & Neuritis OpticDocument42 pagesPapiledema & Neuritis OpticNadine Wang0% (1)
- Glaucoma Optic NerveDocument8 pagesGlaucoma Optic NerveernawatiNo ratings yet
- Anatomy and Physiology of EyeDocument19 pagesAnatomy and Physiology of Eyeashwini priyaNo ratings yet
- Fundoscopic Exam GuideDocument27 pagesFundoscopic Exam GuideRobert MontgomeryNo ratings yet
- Observations During Fundus ExaminationDocument3 pagesObservations During Fundus ExaminationAn'umillah Arini ZidnaNo ratings yet
- Optic AtrophyDocument40 pagesOptic Atrophypriya0% (1)
- Neuritis OptikDocument15 pagesNeuritis OptikElan SatriaNo ratings yet
- Essential Ophthalmology NotesDocument31 pagesEssential Ophthalmology NotesHashim Ahmad50% (2)
- Pa Pill EdemaDocument13 pagesPa Pill Edemarutuparna383No ratings yet
- Ahmed 2010Document11 pagesAhmed 2010Karamjot SinghNo ratings yet
- HY OphthalDocument124 pagesHY OphthaltejNo ratings yet
- Eent - Eye - LCCWDocument3 pagesEent - Eye - LCCWBeda MalecdanNo ratings yet
- Visual Loss Prevention Strategies for High-Risk SurgeriesDocument8 pagesVisual Loss Prevention Strategies for High-Risk SurgeriesIda MaryaniNo ratings yet
- RvoDocument43 pagesRvoOrchlon LkNo ratings yet
- Disc Edema Ento KeyDocument2 pagesDisc Edema Ento KeyumakantsinghNo ratings yet
- Neuro-ophthalmic Disorders Evaluation and ManagementDocument97 pagesNeuro-ophthalmic Disorders Evaluation and ManagementMarshet GeteNo ratings yet
- PACES 19 - Eye - FundusDocument5 pagesPACES 19 - Eye - FundusDrShamshad KhanNo ratings yet
- Optic Atrophy :major Review March 2010, Kerala Journal of Ophthalmology, Devendra V. Venkatramani Et AlDocument6 pagesOptic Atrophy :major Review March 2010, Kerala Journal of Ophthalmology, Devendra V. Venkatramani Et AlNavojit ChowdhuryNo ratings yet
- Optic Disc: Symptoms of The Optic Nerve DiseasesDocument11 pagesOptic Disc: Symptoms of The Optic Nerve DiseasesDilawar JanNo ratings yet
- Optic Nerve DiseaseDocument17 pagesOptic Nerve DiseasemhmdNo ratings yet
- Fundus Exam: Interior Surface of the Eye Opposite the LensDocument22 pagesFundus Exam: Interior Surface of the Eye Opposite the LensDheerajJonnalagaddaNo ratings yet
- OphthoDocument2 pagesOphthoGayathriNo ratings yet
- Normal Eye With Sudden Decreased VisionDocument38 pagesNormal Eye With Sudden Decreased VisionAnjar NuryantoNo ratings yet
- Ophthalmology - Acute Visual Loss PBL Case 2Document13 pagesOphthalmology - Acute Visual Loss PBL Case 2halesNo ratings yet
- Optic Neuritis: Demyelinating Disorders: Multiple Sclerosis (MS)Document4 pagesOptic Neuritis: Demyelinating Disorders: Multiple Sclerosis (MS)Najibah YaNo ratings yet
- NCP Rheum 0268Document9 pagesNCP Rheum 0268drheriNo ratings yet
- ABNORMAL EYES SIGNS GUIDEDocument50 pagesABNORMAL EYES SIGNS GUIDEMarie Jennifer ParilNo ratings yet
- INFLAMMATORY OPTIC NEURITIS & NEURORETINITISDocument49 pagesINFLAMMATORY OPTIC NEURITIS & NEURORETINITISVishal KulkarniNo ratings yet
- Print FriendlyDocument14 pagesPrint FriendlyLaura PutriNo ratings yet
- Food and CyanideDocument2 pagesFood and CyanideeugeniarNo ratings yet
- Chatgpt ONDocument9 pagesChatgpt ONdinimaslomanNo ratings yet
- Retinal DetachmentDocument9 pagesRetinal DetachmentAnita Amanda PrayogiNo ratings yet
- Papilledema: Jump To Navigationjump To SearchDocument4 pagesPapilledema: Jump To Navigationjump To SearchEri DooNo ratings yet
- RetinaDocument76 pagesRetinaSarahNo ratings yet
- Centralretinalarteryocclusion 150821150708 Lva1 App6891 PDFDocument50 pagesCentralretinalarteryocclusion 150821150708 Lva1 App6891 PDFDhivya SekarNo ratings yet
- Brainstem II: Eye Movements and Pupillary ControlDocument34 pagesBrainstem II: Eye Movements and Pupillary ControlhemendreNo ratings yet
- Ref 02Document6 pagesRef 02Mohamad FachryNo ratings yet
- Approach To The Adult With Acute Persistent Visual LossDocument17 pagesApproach To The Adult With Acute Persistent Visual LossMauricio SvNo ratings yet
- Acute Visual LossDocument10 pagesAcute Visual LossJim Jose AntonyNo ratings yet
- Papilloedema 71Document23 pagesPapilloedema 71Shivani NairNo ratings yet
- Introduction To FundusDocument55 pagesIntroduction To FundusGingerNo ratings yet
- Case 1: 70-Yr Man Complains of Sudden and Total Loss Vision in One Eye. No Pain or Other SymptomsDocument17 pagesCase 1: 70-Yr Man Complains of Sudden and Total Loss Vision in One Eye. No Pain or Other SymptomsCherry TamNo ratings yet
- Chronic Visual LossDocument7 pagesChronic Visual LossJim Jose AntonyNo ratings yet
- Physical Exam FindingsDocument77 pagesPhysical Exam FindingsMohamed Kamel MehrziNo ratings yet
- Abdominal PXDocument60 pagesAbdominal PXabinadivegaNo ratings yet
- SGD LBM 3 Modul MataDocument12 pagesSGD LBM 3 Modul MataMillatiazmi Maulida ArdianiNo ratings yet
- Clinical: Section 3 of 7Document13 pagesClinical: Section 3 of 7emilio9fernandez9gatNo ratings yet
- Seeing Inside the EyeDocument10 pagesSeeing Inside the EyeKristin NataliaNo ratings yet
- Neuro Bar Topics 1-68-1Document122 pagesNeuro Bar Topics 1-68-1ahmedaznjadatNo ratings yet
- Direct Ophthalmoscopy: Dr. Joe M Das Senior Resident Dept. of NeurosurgeryDocument51 pagesDirect Ophthalmoscopy: Dr. Joe M Das Senior Resident Dept. of NeurosurgerytaniamaulaniNo ratings yet
- Low Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsFrom EverandLow Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsNo ratings yet
- DK 1 - HemaDocument63 pagesDK 1 - HemaEdwin DarmawanNo ratings yet
- Journal Reading - TLR9 Expression Correlates with Cytokine Levels in SLE PatientsDocument48 pagesJournal Reading - TLR9 Expression Correlates with Cytokine Levels in SLE PatientsEdwin DarmawanNo ratings yet
- Bed Side TeachingmiopiDocument6 pagesBed Side TeachingmiopiEdwin DarmawanNo ratings yet
- Case Report Session Burn Injury: Preseptor: Ira Rubianti, DR., SPBPDocument13 pagesCase Report Session Burn Injury: Preseptor: Ira Rubianti, DR., SPBPEdwin DarmawanNo ratings yet
- Trauma: Bagian Ortopedi Dan TraumatologiDocument7 pagesTrauma: Bagian Ortopedi Dan TraumatologiEdwin DarmawanNo ratings yet
- Bed Side TeachingbdahanakDocument3 pagesBed Side TeachingbdahanakFizree IsmailNo ratings yet
- Clinical Science SessionDocument9 pagesClinical Science SessionEdwin DarmawanNo ratings yet
- PterigiumDocument16 pagesPterigiumEdwin DarmawanNo ratings yet
- TEORI - Wound HealingDocument23 pagesTEORI - Wound HealingEdwin DarmawanNo ratings yet
- TEORI - Hemangioma1Document29 pagesTEORI - Hemangioma1Edwin DarmawanNo ratings yet
- Osteoarthritis: Arranged byDocument12 pagesOsteoarthritis: Arranged byEdwin DarmawanNo ratings yet
- Basal Cell Carcinoma: Case Report SessionDocument5 pagesBasal Cell Carcinoma: Case Report SessionEdwin DarmawanNo ratings yet
- Clinical Science Session Carpal Tunnel Syndrome: Preceptor: Dr. H. Djajang Suhana, SP.S (K)Document20 pagesClinical Science Session Carpal Tunnel Syndrome: Preceptor: Dr. H. Djajang Suhana, SP.S (K)Edwin DarmawanNo ratings yet
- CRS PNDDocument4 pagesCRS PNDEdwin DarmawanNo ratings yet
- RUL Pneumonia with air bronchogram and minor fissure silhouetteDocument33 pagesRUL Pneumonia with air bronchogram and minor fissure silhouetteEdwin DarmawanNo ratings yet
- DyspepsiaDocument25 pagesDyspepsiaCynthia StefanusNo ratings yet
- Somatoform Disorders: Andre Samosir Vicci PuspaDocument11 pagesSomatoform Disorders: Andre Samosir Vicci PuspaEdwin DarmawanNo ratings yet
- Upper Limb: Edward Jaya HadiDocument33 pagesUpper Limb: Edward Jaya HadiEdwin DarmawanNo ratings yet
- Ultrasonograph yDocument24 pagesUltrasonograph yEdwin DarmawanNo ratings yet
- Ultrasonograph yDocument24 pagesUltrasonograph yEdwin DarmawanNo ratings yet
- Interstitial Vs AlveolarDocument17 pagesInterstitial Vs AlveolarEdwin DarmawanNo ratings yet
- DysenteryDocument3 pagesDysenteryEdwin DarmawanNo ratings yet
- Ethical and Legal Issues in Reproductive HealthDocument4 pagesEthical and Legal Issues in Reproductive HealthBianca_P0pNo ratings yet
- Officinalis) : Lavender (LavandulaDocument3 pagesOfficinalis) : Lavender (LavandulaMacsim RoxanaNo ratings yet
- State Medical Register of Madhya PradeshDocument1,214 pagesState Medical Register of Madhya PradeshAnonymous B35kDvZNo ratings yet
- Doctors DetailsDocument11 pagesDoctors Detailscyberlove160027009No ratings yet
- Nurse's Pocket GuideDocument11 pagesNurse's Pocket GuideRaf_Harold_427No ratings yet
- 2 Salivary GlandsDocument20 pages2 Salivary GlandsKaty SanchezNo ratings yet
- Lower Extremity Venous Duplex USDocument6 pagesLower Extremity Venous Duplex USjmg_mdNo ratings yet
- Chcics301b v2 Provide Support To Meet Personal Care NeedsDocument80 pagesChcics301b v2 Provide Support To Meet Personal Care Needsapi-87967494No ratings yet
- DC-6 Operation Manual Basic CE V1.1Document149 pagesDC-6 Operation Manual Basic CE V1.1giulian2009100% (1)
- Ceramic Restorations: Bonded Porcelain Veneers - Part 1: PerspectiveDocument5 pagesCeramic Restorations: Bonded Porcelain Veneers - Part 1: PerspectiveVinisha Vipin SharmaNo ratings yet
- T.N.T. health hazards of munitions workDocument3 pagesT.N.T. health hazards of munitions workLetícia LamasNo ratings yet
- Anatomi Wajah Untuk Filler 220815Document71 pagesAnatomi Wajah Untuk Filler 220815feilicia75% (4)
- Clinical Use of Reproductive HormonesDocument9 pagesClinical Use of Reproductive HormonesYaserAbbasiNo ratings yet
- Vol 4 DBR EPC AIIMS GKPR - 21.01.2018Document234 pagesVol 4 DBR EPC AIIMS GKPR - 21.01.2018Shyam SinghNo ratings yet
- Population Welfare Program and ServicesDocument57 pagesPopulation Welfare Program and Servicesadeel_khan_48No ratings yet
- Neonatal Disease Severity Scoring SystemsDocument6 pagesNeonatal Disease Severity Scoring Systemsida ayu agung WijayantiNo ratings yet
- Differentiate Between With AnswersDocument14 pagesDifferentiate Between With AnswersStephy SojanNo ratings yet
- Phyllodes TumorsDocument4 pagesPhyllodes TumorsNexi anessaNo ratings yet
- INTRODUCTION Teenage Pregnancy - Docx MilynDocument2 pagesINTRODUCTION Teenage Pregnancy - Docx Milynprince4hircs4christi100% (7)
- Invaginasi Jurnal2 PDFDocument4 pagesInvaginasi Jurnal2 PDFZieky YoansyahNo ratings yet
- OB Definition of TermsDocument9 pagesOB Definition of TermsWarrenSandovalNo ratings yet
- Reconstruction of MaxillaDocument58 pagesReconstruction of MaxillaAnjum IqbalNo ratings yet
- The Fifth Vital Sign Implementation PDFDocument8 pagesThe Fifth Vital Sign Implementation PDFTeten RustendiNo ratings yet
- Epilepsy in PregnancyDocument33 pagesEpilepsy in PregnancyxxdrivexxNo ratings yet
- ACS BookletDocument14 pagesACS Bookletmyat25No ratings yet
- RCH program goals for reproductive health and child survivalDocument2 pagesRCH program goals for reproductive health and child survivalAnnapurna DangetiNo ratings yet
- Assessment of The Use of A Dental Mouth MirrorDocument7 pagesAssessment of The Use of A Dental Mouth MirrorIOSRjournalNo ratings yet
- Stenosis Trakea Post TrakeotomiDocument7 pagesStenosis Trakea Post TrakeotomiVania Dwi AndhaniNo ratings yet