Professional Documents
Culture Documents
Cirrhosis of The Liver: Glossary
Uploaded by
Noph0 ratings0% found this document useful (0 votes)
77 views21 pagesIn 2005, cirrhosis and other liver disorders were listed as the 12th leading cause of death in the United States. Liver transplantation is currently the only life-saving procedure for end-stage disease.
Original Description:
Original Title
Cirrhosis
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentIn 2005, cirrhosis and other liver disorders were listed as the 12th leading cause of death in the United States. Liver transplantation is currently the only life-saving procedure for end-stage disease.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
77 views21 pagesCirrhosis of The Liver: Glossary
Uploaded by
NophIn 2005, cirrhosis and other liver disorders were listed as the 12th leading cause of death in the United States. Liver transplantation is currently the only life-saving procedure for end-stage disease.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 21
CIRRHOSIS OF THE LIVER
I. Pathophysiology (Murphy, 2006)
a. Alteration in structure and degenerative changes resulting from buildup of diffuse bands of fibrotic
connective tissue causing widespread destruction of hepatic cells, impairing liver function, and impeding
blood flow through the liver
b. Compensated cirrhosis: Liver function may continue for some time, even with significant scarring, but
metabolic abnormalities can occur, such as coagulation defects and malnutrition.
c. Decompensated cirrhosis: progression of failure with significant complications, such as portal hypertension
with bleeding varices, ascites, peritonitis, hepatorenal syndrome, and encephalopathy
II. Etiology
a. Rate of progression of fibrosis to cirrhosis varies for unknown reasons.
b. Multiple causation (Wolf, 2007)
i. Hepatitis C (26%), B, and D (15%)
ii. Alcoholic liver disease (21%)
iii. Cholestatic diseases: biliary atresia, primary biliary cirrhosis, cystic fibrosis, primary sclerosing
cholangitis
iv. Miscellaneous liver disorders, including autoimmune, Wilsons disease, alpha
1
-antitrypsin deficiency,
hemochromatosis
v. Injury from trauma, drugs, or other environmental toxins
III. Treatment
a. Goals are to slow the progression of the disease and alleviate the symptoms.
b. Liver transplantation is currently the only life-saving procedure for end-stage disease.
IV. Statistics
a. Morbidity: In 2005, 112,000 hospitalizations for chronic liver disease or cirrhosis; approximately 17,000
individuals awaiting liver transplant (Scientific Registry of Transplant Recipients [SRTR], 2007).
b. Mortality: Approximately 35,000 deaths annually due to chronic liver disease and cirrhosis (Wolf, 2007);
in 2005, cirrhosis and other liver disorders were listed as the 12th leading cause of death in the United
States (Hsiang-Ching, 2008).
GLOSSARY
Ascites: Buildup of fluid in the abdomen, due to a number of conditions including severe liver disease.
Asterixis: Involuntary jerking movements of hands and feet associated with hepatic encephalopathy.
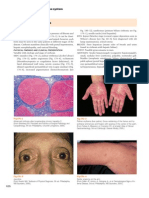
Ecchymosis: Skin discoloration consisting of a large, irregularly formed hemorrhagic area with colors
changing from blue-black to greenish-brown or yellow; commonly referred to as a bruise.
Fetor hepaticus: Particularly foul-smelling breath, which frequently precedes hepatic coma.
Hematemesis: Bloody vomitus.
Hepatic encephalopathy: Brain dysfunction directly due to liver dysfunction seen in advanced cirrhosis,
resulting in disturbances of consciousness and progressing to coma.
Hepatomegaly: Enlarged liver.
Hepatorenal syndrome: Represents a continuum of kidney dysfunction observed in individuals with
cirrhosis caused by the vasoconstriction of large and small renal arteries.
Jaundice: Yellow staining of the skin and sclerae (and sometimes other tissues and body fluids) because of
abnormally high blood levels of bilirubin.
Melena: Bloody stools.
Oliguria: Urinary output less than 400 mL/day.
Palmar erythema: Redness of the palms of the hands caused by dilation and congestion of capillaries.
Peritoneovenous shunt: Surgically implanted device for continuous draining of ascitic fluid into the venous
system. Fluid is removed via a pressure-sensitive one-way valve. It is connected to a tube under the
subcutaneous tissue of the chest wall to the neck, where it enters the internal jugular vein and terminates
in the superior vena cava.
Petechiae: Tiny red dots on the skin caused by minute hemor-rhage, indicating low platelet count or other
blood disorder.
Spider angiomas: Abnormal collection of blood vessels near the surface of the skin; can occur anywhere,
but are most common on the face and trunk.
Splenomegaly: Enlarged spleen.
Telangiectasis: Visibly dilated blood vessel on the skin or mucosal surface.
Care Setting
Client may be hospitalized on a medical unit during initial or recurrent acute episodes with
potentially life-threatening complications. Otherwise, this condition is managed at the community,
outpatient level.
Related Concerns
Alcohol: acute withdrawal
Substance dependence/abuse rehabilitation
Fluid and electrolyte imbalances
Psychosocial aspects of care
Renal dialysis
Renal failure: acute
Total nutritional support: parenteral/enteral feeding
Upper gastrointestinal/esophageal bleeding
Client Assessment Database
Data depend on underlying cause of the condition.
DIAGNOSTIC DIVISION
MAY REPORT MAY EXHIBIT
ACTIVITY/REST
Weakness
Fatigue, exhaustion
Lethargy
Decreased muscle mass and tone
CIRCULATION
History of or recent onset of heart failure (HF),
pericarditis, rheumatic heart disease, or cancer,
causing liver impairment leading to failure
Easy bruising, nosebleeds, bleeding gums
Hypertension or hypotension (fluid shifts)
Dysrhythmias, extra heart soundsS
3
, S
4
Jugular vein distention (JVD), distended abdominal
veins, spider angiomas, collateral circulation
Ecchymosis, petechiae
Anemia, leukopenia, thromboctyopenia, coagulation
disorders, splenomegaly
ELIMINATION
Flatulence
Diarrhea or constipation
Gradual abdominal enlargement
Abdominal distention (hepatomegaly, splenomegaly,
ascites)
Decreased or absent bowel sounds
Clay-colored stools, melena
Hemorrhoidal varices
Dark, concentrated urine; oliguria (hepatorenal
syndrome, failure)
FOOD/FLUID
Anorexia
Food intolerance, ingestion
Nausea, vomiting
Hematemesis
Weight loss or gain (fluid)
Tissue wasting, delayed wound healing
Edema generalized in tissues
Dry skin, poor turgor
Halitosis or fetor hepaticus, bleeding gums
Hypoalbuminemia
NEUROSENSORY
Significant other (SO)/family may report
personality changes, depressed mentation
Changes in mentation, confusion, hallucinations,
coma
Slowed, slurred speech
Asterixis
PAIN/DISCOMFORT
Abdominal tenderness and right upper quandrant
(RUQ) pain
Severe itching
Pins-and-needles sensation, burning pain in
extremities (peripheral neuropathy)
Guarding or distraction behaviors
Self-focus
RESPIRATION
Dyspnea Tachypnea, shallow respiration, adventitious breath
sounds
Limited thoracic expansion because of ascites
Hypoxia
SAFETY
Itching, dryness of the skin (pruritus) Fevermore common in alcoholic cirrhosis
Jaundiced skin and sclera
Spider angiomas, telangiectasis
Palmar erythema
Confusion progressing to delirium and coma (hepatic
encephalopathy)
Unsteady or shaky, jerking movements
SEXUALITY
Menstrual disorders (women)
Impotence (men)
Testicular atrophy, gynecomastia, loss of hair
chest, underarm, pubic
TEACHING/LEARNING
History of long-term alcohol or injection drug use
or abuse, alcoholic liver disease, use of drugs
affecting liver function
History of biliary system disease, hepatitis,
exposure to toxins, liver trauma
DISCHARGE PLAN CONSIDERATIONS
May need assistance with self-care and other
activities of daily living (ADLs), homemaking and
maintenance tasks
Refer to section at end of plan for postdischarge
considerations.
Diagnostic Studies
TEST
WHY IT IS DONE WHAT IT TELLS ME
BLOOD TESTS
Serum bilirubin (total and indirect unconjugated):
Bilirubin results from the breakdown of hemoglobin.
Elevated because of cellular disruption, or biliary
obstruction, causing jaudice.
Liver enzymes:
Aspartate aminotransferase/alanine
aminotransferase (AST/ALT), lactate
dehydrogenase (LDH), and isoenzymes (LDH
5
):
Detects liver damage.
Increased because of cellular damage and release of
enzymes. Most specific indicator of hepatitis as
cause (Murphy, 2006).
Alkaline phosphatase (ALP) and isoenzyme (APL
1
):
Enzyme found in high concentration in the liver cells
Elevated in biliary obstruction.
forming the bile ducts as well as in other tissues.
APL
1
is more specific to the liver and helpful in
determining type and extent of cirrhosis.
Gamma glutamyl transpeptidase (GGTP): Screens
for liver disease and alcohol abuse.
Level is elevated.
Serum albumin: Protein of the highest concentration
in plasma. Transports substances, such as bilirubin,
calcium, progesterone, and drugs, and regulates
osmotic pressure of blood, keeping fluid from
leaking out into the tissues.
Because albumin is made by the liver, decreased
serum albumin may result from liver disease.
Decreased albumin may also be explained by
malnutrition or a low-protein diet.
Immunoglobulin (Ig) A, G, and M: Proteins found
in blood or other bodily fluids used by the immune
system to identify and neutralize foreign objects,
such as bacteria and viruses.
Levels are increased.
Complete blood count (CBC): Battery of screening
tests, which typically includes hemoglobin (Hgb);
hematocrit (Hct); red blood cell (RBC) count,
morphology, indices, and distribution width index;
platelet count and size; white blood cell (WBC)
count and differential.
Hb, Hct, and RBCs may be decreased because of
bleeding and RBC destruction. Anemia is seen with
hypersplenism and iron deficiency. Leukopenia may
be present as a result of hypersplenism.
Bleeding/clotting:
Prothrombin time (PT): Measures length of time
required for blood sample to clot.
Prolonged because of decreased production of clotting
proteins and fat-soluble vitamin K deficiency,
leading to easy bleeding.
Fibrinogen and other clotting factors: Used to
monitor the progression of liver disease over time.
Decreased; chronically low levels seen in end-stage
liver disease.
Blood urea nitrogen (BUN): Urea is the end product
of protein metabolism formed in the liver from
amino acids and from ammonia compounds.
Elevation indicates breakdown of blood proteins and
possible kidney dysfunction because of diuretic use
in treatment of ascites.
Serum ammonia: Product of breakdown of protein,
which is normally converted to urea and excreted.
Elevated because of inability to convert ammonia to
urea.
Serum glucose: One of the simple sugars in the
blood, which serves as primary energy source for
cells.
Low blood glucose (hypoglycemia) suggests impaired
synthesis of glycogen from glucose (glycogenesis).
Electrolytes: Substances that dissociate into ions in
solution and acquire the capacity to conduct
electricity. Common electrolytes include sodium,
potassium, chloride, calcium, and phosphate.
Low potassium (hypokalemia) may reflect increased
aldosterone, although various imbalances may occur.
Low calcium (hypocalcemia) may occur because of
impaired absorption of vitamin D.
Nutrient studies: Evaluate nutritional status. Deficiency of vitamins A, B
12
, C, and K; folic acid;
and iron may be noted.
Viral tests: Determine if cirrhosis is caused by viral Hepatitis B, C, or D may be present.
hepatitis.
OTHER DIAGNOSTIC STUDIES
Abdominal ultrasonography with Doppler:
Diagnostic technique that uses sound waves to
produce an image of internal body structures.
May be first assessment performed in individual with
suspected liver disease to detect ascites and enlarged
liver and spleen. It can also identify biliary duct
obstruction or bile stones. Nodularity, irregularity,
and atrophy are ultrasonographic hallmarks of
cirrhosis. In advanced disease, the gross liver
appears small and multinodular, ascites may be
detected, and Doppler flow can be significantly
decreased in the portal circulation.
Liver biopsy: Biopsy can be performed via
percutaneous, transjugular, laparoscopic, open
operative, or computed tomography (CT)-guided
fine-needle approaches. Samples are obtained for
microscopic evaluation.
Detects fatty infiltrates, fibrosis, destruction of hepatic
tissues, tumors (primary or metastatic), and
associated ascites.
Percutaneous transhepatic cholangiography
(PTHC): X-ray procedure where dye is injected
directly into the drainage system of the liver. If
necessary, a catheter may be inserted to allow the
bile to drain into a collection bag outside the body or
into the small intestine.
Shows whether there is a blockage in the liver or the
bile ducts that drain it. May be done to differentiate
causes of jaundice or to perform biliary drainage.
Hepatobiliary iminodiacetic acid (HIDA) scan: The
client is given a radioactive tracer intravenously (IV)
that is excreted by the liver into bile ducts.
Identifies blockages in the biliary system.
Urine and stool urobilinogen: Serves as guide for
differentiating liver disease, hemolytic disease, and
biliary obstruction.
May or may not be present.
Nursing Priorities
1. Maintain adequate nutrition.
2. Prevent complications.
3. Enhance self-concept and acceptance of situation.
4. Provide information about disease process, prognosis, potential complications, and treatment
needs.
Discharge Goals
1. Nutritional intake adequate for individual needs.
2. Complications prevented or minimized.
3. Deals effectively with current reality.
4. Disease process, prognosis, potential complications, and therapeutic regimen understood.
5. Plan in place to meet needs after discharge.
NURSING DIAGNOSIS: imbalanced Nutrition: Less than Body Requirements
May be related to
Inadequate diet; inability to process, digest nutrients
Anorexia, nausea, vomiting, indigestion, early satiety (ascites)
Abnormal bowel function
Possibly evidenced by
Weight loss
Changes in bowel sounds and function
Poor muscle tone, muscle wasting; fatigue
Imbalances in nutritional studies
Desired Outcomes/Evaluation CriteriaClient Will
Nutritional Status NOC
Demonstrate progressive weight gain toward goal with client-appropriate normalization of laboratory values.
Experience no further signs of malnutrition.
ACTIONS/INTERVENTIONS RATIONALE
Nutrition Therapy NIC
Independent
Evaluate clients risk for malnutrition. Eighty-five percent to 90% of the blood that leaves
the stomach and intestines carries nutrients to
the liver where they are converted into
substances the body can use. The client with
liver dysfunction often has malnutrition because
of inadequate dietary intake due to poor food
choices or preference for alcohol rather than food
and may currently have malabsorption syndrome
due to inability to process or digest nutrients,
anorexia, nausea or vomiting, indigestion, or early
satiety associated with ascites. Because of the
decreased secretion of bile into the gut, client
may have difficulty absorbing fat and fat-soluble
vitamins A, D, E, and K. These deficiencies can
lead to such complications as decreased vision in
the dark, due to vitamin A deficiency; bone
disease, due to vitamin D deficiency; neurological
impairment, due to vitamin E deficiency; and
decreased production of clotting proteins in the
liver, due to vitamin K deficiency (Brettler, 2003).
Determine interest in eating and ability to chew,
swallow, and taste. Discuss eating habits,
including food preferences, intolerances, or
aversions. Note availability and use of support
systems.
Factors that affect ingestion and digestion of
nutrients.
Determine dietary intake and perform calorie count if
client is eating.
Provides information about intake, needs, and
deficiencies. Client with cirrhosis requires a
balanced protein diet providing 2,000 to 3,000
calories per day to permit liver cell regeneration.
Weigh, as indicated. Compare changes in fluid status
and recent weight history.
It may be difficult to use weight as a direct indicator
of nutritional status in view of edema and ascites.
Note: Undigested fat that passes into the large
intestine can cause diarrhea and lead to weight
loss (Brettler, 2003).
Assist or encourage client to eat; explain reasons for
the types of diet. Feed client if tiring easily, or
have SO assist client. Consider preferences in
food choices.
Improved nutrition is vital to recovery. Client may eat
better if family is involved and preferred foods are
included as much as possible. Client and family
must understand protein intake limitations and
how best to meet needs and desires within
limitations.
Encourage client to eat all meals and supplementary
feedings.
Client may demonstrate loss of interest in food
because of nausea, generalized weakness, and
fatiguewhich is often first reported symptom
and seen in approximately 70% of clients with
cirrhosis (Taylor, 2008).
Recommend or provide small, frequent meals. Poor tolerance to larger meals may be due to
increased intra-abdominal pressure or ascites.
Limit such high-salt foods as canned soups and
vegetables, processed meats, and condiments.
Provide salt substitutes if allowed, avoiding those
containing ammonia.
Salt limitations can help manage fluid complications
in cirrhosis, including ascites or tissue edema.
Salt substitutes enhance the flavor of food and
aid in increasing appetite; ammonia potentiates
risk of encephalopathy.
Restrict intake of caffeine and gas-producing or spicy
and excessively hot or cold foods.
Aids in reducing gastric irritation, diarrhea, and
abdominal discomfort that may impair oral intake
and digestion.
Encourage or provide frequent mouth care, especially
before meals.
Client is prone to sore and bleeding gums and bad
taste in mouth, which contributes to anorexia.
Provide assistance with activities as needed.
Promote undisturbed rest periods, especially
before meals.
Conserving energy reduces metabolic demands on
the liver and promotes cellular regeneration.
Recommend cessation of smoking. Reduces excessive gastric stimulation and risk of
irritation and bleeding.
Collaborative
Monitor nutritional laboratory studies: serum glucose,
prealbumin or albumin, total protein, and
ammonia.
Glucose may be decreased because of impaired
glycogenesis, depleted glycogen stores, or
inadequate intake. Protein may be low because of
impaired metabolism, decreased hepatic
synthesis, or loss into peritoneal cavity (ascites).
Protein-calorie malnutrition contributes to further
development of fatty liver and deterioration of
function. Elevation of ammonia level may require
restriction of protein intake to prevent serious
complications.
Maintain nothing by mouth (NPO) status, when
indicated.
Gastrointestinal (GI) rest may be required in acutely
ill clients to reduce demands on the liver and
production of ammonia and urea in the GI tract.
When this is the case, nutrition must be supplied
by another methodenteral or parenteral
feedings.
Determine nutritional and caloric needs using
appropriate methods, such as total energy
expenditure (TEE), body mass index (BMI), Harris-
Benedict equation, or indirect calorimetry test, as
indicated.
Identifies energy requirements and deficits. Skinfold
measurements and indirect calorimetry are useful
in assessing changes in muscle mass, energy
expenditure, and subcutaneous fat reserves.
Consult with dietitian or nutritionist to provide diet
that is high in calories and simple carbohydrates,
low in fat, and low to moderate in protein. Limit
sodium, as necessary. Provide liquid supplements,
as indicated.
Because clients intake is usually limited, high-calorie
foods are desired. Carbohydrates supply readily
available energy. Fats are poorly absorbed
because of liver dysfunction and may contribute
to abdominal discomfort. Proteins are needed to
improve serum protein levels, reducing edema and
promoting liver cell regeneration. However,
protein can also elevate ammonia levels and must
be restricted if ammonia level is elevated or if
client has clinical signs of hepatic
encephalopathy. In addition, these individuals
may tolerate vegetable protein better than meat
protein.
Provide enteral tube feedings or total parenteral
nutrition (TPN), if indicated.
May be required to supplement diet or to provide
nutrients when client is too nauseated or anorexic
to eat or when esophageal varices interfere with
oral intake. (Refer to CP: Total Nutritional
Support: Parenteral/Enteral Feedings.)
Administer medications, as indicated, for example:
Vitamin supplements (especially fat-soluble vitamins Replacement required because of the inability of the
A, D, E, K) and B vitamins (thiamine, iron, folic
acid)
liver to process or store vitamins.
Zinc sulfate Improves sense of taste and may enhance appetite.
Digestive enzymes, such as pancrelipase (Niokase)
and lactulose
May be tried to promote digestion of fats and reduce
incidence of steatorrhea and diarrhea.
Antiemetics, such as trimethobenzamide (Tigan) Used with caution to reduce nausea and vomiting
and enhance oral intake.
NURSING DIAGNOSIS: excess Fluid Volume
May be related to
Compromised regulatory mechanismsyndrome of inappropriate antidiuretic hormone (SIADH), decreased
plasma proteins, malnutrition
Excess sodium and fluid intake
Possibly evidenced by
Edema, anasarca, weight gain
Intake greater than output, oliguria, changes in urine specific gravity
Dyspnea, adventitious breath sounds, pleural effusion
Blood pressure (BP) changes, altered central venous pressure (CVP)
JVD, positive hepatojugular reflex
Altered electrolyte levels
Change in mental status
Desired Outcomes/Evaluation CriteriaClient Will
Fluid Balance NOC
Demonstrate stabilized fluid volume, with balanced intake and output (I&O), stable weight, vital signs
within clients normal range, and absence of edema.
ACTIONS/INTERVENTIONS RATIONALE
Fluid/Electrolyte Management NIC
Independent
Measure I&O, noting positive balanceintake in
excess of output. Weigh daily, and note gain
more than 0.5 kg/day.
Reflects circulating volume status, developing or
resolving fluid shifts, and response to therapy.
Positive fluid balance and weight gain often
reflects continuing fluid retention. Note:
Decreased circulating volume and fluid shifts can
directly affect renal function and urine output,
resulting in hepatorenal syndrome.
Monitor BP and CVP, if available. Note JVD and
abdominal vein distention.
BP elevations are usually associated with fluid
volume excess but may not occur because of
fluid shifts out of the vascular space. JVD and
presence of distended abdominal veins are
associated with vascular congestion.
Assess respiratory status, noting increased
respiratory rate and dyspnea.
Indicative of pulmonary congestion or edema.
Auscultate lungs, noting diminished or absent breath
sounds and developing adventitious sounds
crackles.
Increasing pulmonary congestion may result in
consolidation, impaired gas exchange, and
complications, such as pulmonary edema.
Monitor for cardiac dysrhythmias. Auscultate heart
sounds, noting development of S3/S4 gallop
rhythm.
May be caused by HF, decreased coronary arterial
perfusion, or electrolyte imbalance.
Assess degree of peripheral and dependent edema. Fluids shift into tissues as a result of sodium and
water retention, decreased albumin, and
increased antidiuretic hormone (ADH).
Measure abdominal girth. Reflects accumulation of fluid or ascites resulting
from loss of plasma proteins and fluid into
peritoneal space. Note: Excessive fluid
accumulation can reduce circulating volume,
resulting in hypotension and dehydration.
Encourage bedrest when ascites is present. May promote recumbency-induced diuresis.
Provide frequent mouth care and occasional ice
chips, particularly if NPO; schedule fluid intake
around the clock.
Decreases sensation of thirst, especially when fluid
intake is restricted.
Collaborative
Monitor serum albumin and electrolytes, particularly
potassium and sodium.
Decreased serum albumin affects plasma colloid
osmotic pressure, resulting in edema formation.
Reduced renal blood flow, accompanied by
elevated ADH and aldosterone levels and the use
of diuretics to reduce total body water, may
cause various electrolyte shifts and imbalances.
Monitor serial chest x-rays. Vascular congestion, pulmonary edema, and pleural
effusions frequently occur.
Restrict sodium and fluids, as indicated. Sodium may be restricted to minimize fluid retention
in extravascular spaces. Fluid restriction may be
necessary to correct dilutional hyponatremia.
Administer salt-free albumin and plasma expanders,
as indicated.
Albumin may be given to increase the colloid osmotic
pressure in the vascular compartment, thereby
increasing effective circulating volume and
decreasing formation of ascites.
Administer medications, as indicated, for example:
Diuretics, such as spironolactone (Aldactone) and
furosemide (Lasix)
Used with caution to control edema and ascites,
block effect of aldosterone, and increase water
excretion while sparing potassium when
conservative therapy with bedrest and sodium
restriction do not alleviate problem. Diuretic given
in coordination with albumin administration may
enhance fluid removal.
Potassium Serum and cellular potassium are usually depleted
because of liver disease and urinary losses.
Positive inotropic drugs and arterial vasodilators Given to increase cardiac output and improve renal
blood flow and function, thereby reducing excess
fluid.
NURSING DIAGNOSIS: risk for impaired Skin Integrity
Risk factors may include
Altered circulation and metabolic state
Accumulation of bile salts in skin
Poor skin turgor, skeletal prominence, presence of edema, ascites
Possibly evidenced by
(Not applicable; presence of signs and symptoms establishes an actual diagnosis)
Desired Outcomes/Evaluation CriteriaClient Will
Risk Control NOC
Maintain skin integrity.
Identify individual risk factors and demonstrate behaviors or techniques to prevent skin breakdown.
ACTIONS/INTERVENTIONS RATIONALE
Skin Surveillance NIC
Independent
Discuss itching with client, addressing areas involved
and time of day when client is most
uncomfortable.
Pruritus affects about two-thirds of clients with
primary biliary cirrhosis; the cause is unknown.
The itching often worsens during the evening and
improves during the day. It typically begins in the
palms and soles, and then spreads to the rest of
the body. Prolonged, repeated scratching can
result in excoriations and thickening and
darkening of the skin (Heathcote, 2000).
Inspect skin surfaces and pressure points routinely.
Gently massage bony prominences or areas of
continued stress. Use emollient lotions and limit
use of soap for bathing.
Edematous tissues are more prone to breakdown and
to the formation of decubitus ulcers. Ascites may
stretch the skin to the point of tearing in severe
cirrhosis.
Encourage and assist with repositioning on a regular
schedule, while in bed or chair, and active or
passive range-of-motion (ROM) exercises, as
Repositioning reduces pressure on edematous tissues
to improve circulation. Exercises enhance
circulation and improve or maintain joint mobility.
appropriate.
Recommend elevating lower extremities. Enhances venous return and reduces edema
formation in extremities.
Keep linens dry and free of wrinkles. Moisture aggravates pruritus and increases risk of
skin breakdown.
Suggest clipping fingernails short and provide
mittens or gloves, if indicated.
Prevents client from inadvertently injuring the skin,
especially while sleeping.
Encourage, or provide, perineal care following
urination and bowel movement.
Prevents skin excoriation breakdown from bile salts.
Collaborative
Use alternating pressure mattress, egg-crate or foam
mattress, waterbed, or sheepskins, as indicated.
Reduces dermal pressure, increases circulation, and
diminishes risk of tissue ischemia and breakdown.
Apply calamine lotion and provide baking soda baths. May be soothing and provide relief of itching.
Administer medications, such as cholestyramine
(Questran), colestipol (Colestid), hydroxyzine
(Atarax), and dronabinol (Marinol), if indicated.
Although the cause of pruritus is unknown, it may be
associated with jaundice or bile salts in skin and
may respond to these treatments.
NURSING DIAGNOSIS: risk for ineffective Breathing Pattern
Risk factors may include
Intra-abdominal fluid collection (ascites)
Decreased lung expansion, accumulated secretions
Decreased energy, fatigue
Possibly evidenced by
(Not applicable; presence of signs and symptoms establishes an actual diagnosis)
Desired Outcomes/Evaluation CriteriaClient Will
Respiratory Status: Ventilation NOC
Maintain effective respiratory pattern and be free of dyspnea and cyanosis, with arterial blood gases (ABGs)
and vital capacity within acceptable range.
ACTIONS/INTERVENTIONS RATIONALE
Ventilation Assistance NIC
Independent
Monitor respiratory rate, depth, and effort. Rapid, shallow respirations or dyspnea may be
present because of hypoxia or fluid accumulation
in abdomen.
Auscultate breath sounds, noting crackles, wheezes,
and rhonchi.
Indicates developing complicationspresence of
adventitious sounds reflects accumulation of fluid
while diminished sounds suggest atelectasis
increasing risk of pulmonary infection.
Investigate changes in level of consciousness (LOC). Changes in mentation may reflect hypoxemia and
respiratory failure, which often accompany
hepatic coma.
Keep head of bed elevated. Position client on side. Facilitates breathing by reducing pressure on the
diaphragm and minimizes risk of aspiration of
secretions.
Encourage frequent repositioning, deep-breathing
exercises, and coughing, as appropriate.
Aids in lung expansion and mobilizing secretions.
Monitor temperature. Note presence of chills,
increased coughing, and changes in color or
character of sputum.
Indicative of onset of infection, such as pneumonia.
Collaborative
Monitor serial ABGs, pulse oximetry, vital capacity
measurements, and chest x-rays.
Reveals changes in respiratory status and developing
pulmonary complications.
Provide supplemental oxygen (O2) as indicated. May be necessary to treat or prevent hypoxia. If
respirations or oxygenation are inadequate,
mechanical ventilation may be required.
Demonstrate and assist with respiratory adjuncts,
such as incentive spirometer.
Reduces incidence of atelectasis and enhances
mobilization of secretions.
Prepare for and assist with acute care procedures,
such as:
Paracentesis Occasionally done to remove ascites fluid to relieve
abdominal pressure when respiratory
embarrassment is not corrected by other
measures.
Peritoneovenous shunt Surgical implant of a catheter to return accumulated
fluid in the abdominal cavity to systemic
circulation via the vena cava; provides long-term
relief of ascites and improvement in respiratory
function.
NURSING DIAGNOSIS: risk for Bleeding
Risk factors may include
Abnormal blood profile; altered clotting factorsdecreased production of prothrombin, fibrinogen, and factors
VIII, IX, and X; impaired vitamin K absorption; and release of thromboplastin
Portal hypertension, development of esophageal varices
Possibly evidenced by
(Not applicable; presence of signs and symptoms establishes an actual diagnosis)
Desired Outcomes/Evaluation CriteriaClient Will
Coagulation Status NOC
Maintain homeostasis with absence of bleeding.
Risk Control NOC
Demonstrate behaviors to reduce risk of bleeding.
ACTIONS/INTERVENTIONS RATIONALE
Bleeding Precautions NIC
Independent
Assess for signs and symptoms of GI bleeding; for
instance, check all secretions for frank or occult
blood. Observe color and consistency of stools,
nasogastric (NG) drainage, or vomitus.
The GI tractesophagus and rectumis the most
usual source of bleeding because of its mucosal
fragility and alterations in homeostasis associated
with cirrhosis.
Observe for presence of petechiae, ecchymosis, and
bleeding from one or more sites.
Subacute disseminated intravascular coagulation
(DIC) may develop secondary to altered clotting
factors.
Monitor pulse, BP, and CVP, if available. An increased pulse with decreased BP and CVP may
indicate loss of circulating blood volume, requiring
further evaluation.
Note changes in mentation and LOC. Changes may indicate decreased cerebral perfusion
secondary to hypovolemia or hypoxemia.
Avoid rectal temperature; be gentle with GI tube
insertions.
Rectal and esophageal vessels are most vulnerable to
rupture.
Encourage use of soft toothbrush and electric razor,
avoiding straining for stool, forceful nose
blowing, and so forth.
In the presence of clotting factor disturbances,
minimal trauma can cause mucosal bleeding.
Use small needles for injections. Apply pressure to
small bleeding or venipuncture sites for longer
than usual.
Minimizes damage to tissues, reducing risk of
bleeding and hematoma.
Recommend avoidance of aspirin-containing
products.
Prolongs coagulation, potentiating risk of
hemorrhage.
Collaborative
Monitor Hgb and Hct, platelets, and clotting factors. Indicators of anemia, active bleeding, or impending
complications, such as DIC.
Administer medications, as indicated, for example:
Supplemental vitamins, such as vitamins K, D, and C Promotes prothrombin synthesis and coagulation, if
liver is functional. Vitamin C deficiencies increase
susceptibility of GI system to irritation and
bleeding.
Stool softeners Prevents straining for stool with resultant increase in
intra-abdominal pressure and risk of bleeding
hemorrhoidal varices, especially when client has
portal hypertension.
Provide gastric lavage with cool saline solution or
water, as indicated.
In presence of acute bleeding, evacuation of blood
from GI tract may reduce ammonia production
and risk of hepatic encephalopathy. (Refer to CP:
Upper Gastrointestinal/Esophageal Bleeding.)
Assist with insertion and maintenance of intestinal or
esophageal tube, such as Sengstaken-Blakemore
tube.
Temporarily controls bleeding of esophageal varices
by balloon tamponade when control by other
means, such as lavage, and hemodynamic
stability cannot be achieved.
Prepare for procedures, such as direct ligation or
banding of varices, esophagogastric resection,
transjugular intrahepatic portosystemic shunt
(TIPS), and splenorenal-portacaval anastomosis.
May be needed to control active hemorrhage or to
decrease portal and collateral blood vessel
pressure to minimize risk of recurrence of
bleeding. TIPS is a nonsurgical procedure to
relieve portal hypertension and decompress
varices by creating a shunt between the systemic
and portal venous systems to redirect portal
blood flow.
NURSING DIAGNOSIS: risk for acute Confusion
Risk factors may include
Alcohol abuse
Inability of liver to detoxify certain enzymes and drugs
Possibly evidenced by
(Not applicable; presence of signs and symptoms establishes an actual diagnosis)
Desired Outcomes/Evaluation CriteriaClient Will
Cognition NOC
Maintain usual level of mentation and reality orientation.
Initiate behaviors or lifestyle changes to prevent or minimize recurrence of problem.
ACTIONS/INTERVENTIONS RATIONALE
Reality Orientation NIC
Independent
Observe for changes in behavior and mentation:
lethargy, confusion, drowsiness, slowing or
slurring of speech, and irritability. Arouse client at
intervals, as indicated.
Ongoing assessment of behavior and mental status is
important because of fluctuating nature of
hepatic encephalopathy or impending hepatic
coma.
Review current medication regimen. Adverse drug reactions or interactions may
potentiate or exacerbate confusion.
Evaluate sleep and rest schedule. Difficulty falling asleep or staying asleep leads to
sleep deprivation, exacerbating cognition
problems and fatigue.
Note development or presence of asterixis, fetor
hepaticus, and seizure activity.
Suggests elevating serum ammonia levels and
increased risk of progression to encephalopathy.
Consult with SO about clients usual behavior and Provides baseline for comparison of current status.
mentation.
Have client write name periodically and keep this
record for comparison. Report deterioration of
ability. Have client do simple arithmetic
computations.
Easy test of neurological status and muscle
coordination.
Reorient to time, place, person, and situation, as
needed.
Assists in maintaining reality orientation, reducing
confusion and anxiety.
Maintain a pleasant, quiet environment and approach
in a slow, calm manner. Encourage uninterrupted
rest periods.
Reduces excessive stimulation and sensory overload,
promotes relaxation, and may enhance coping.
Provide continuity of care. If possible, assign same
nurse over a period of time.
Familiarity provides reassurance, aids in reducing
anxiety, and provides a more accurate
documentation of subtle changes.
Reduce provocative stimuli and confrontation.
Refrain from forcing activities. Assess potential
for violent behavior.
Avoids triggering agitated, violent responses;
promotes client safety.
Discuss current situation and future expectations. Client and SO may be reassured that intellectual as
well as emotional function may improve as liver
involvement resolves.
Maintain bedrest and assist with self-care activities. Reduces metabolic demands on liver, prevents
fatigue, and promotes healing, lowering risk of
ammonia buildup.
Identify and provide for safety needs, such as
supervision during smoking, bed in low position,
side rails up, and pad, if necessary. Provide close
supervision.
Reduces risk of injury when confusion, seizures, or
violent behavior occurs.
Investigate temperature elevations. Monitor for signs
of infection.
Infection may precipitate hepatic encephalopathy
caused by tissue catabolism and release of
nitrogen.
Recommend avoidance of narcotics or sedatives,
anti-anxiety agents, and limiting or restricting use
of medications metabolized by the liver.
Certain drugs are toxic to the liver, whereas other
drugs may not be metabolized because of
cirrhosis, causing cumulative effects that affect
mentation, mask signs of developing
encephalopathy, or precipitate coma.
Collaborative
Monitor laboratory studies, such as ammonia,
electrolytes, pH, blood urea nitrogen (BUN),
glucose, and CBC with differential.
Elevated ammonia levels, hypokalemia, metabolic
alkalosis, hypoglycemia, anemia, and infection can
precipitate or potentiate development of hepatic
coma.
Eliminate or restrict protein in diet. Provide glucose
supplements and adequate hydration.
Ammonia is responsible for mental changes in
hepatic encephalopathy. Dietary changes may result
in constipation, which also increases bacterial action
and formation of ammonia. Glucose provides a
source of energy, reducing need for protein
catabolism.
Administer medications, as indicated, for example:
Ursodeoxycholic acid (urosodiol, UDCA, Actigall) Major medication used to slow the progression of the
disease; may delay need for transplantation.
Immunosuppressive agents, such as corticosteroids
(Prednisolone, DeltaCortef), methotrexate
(Rheumatrex/Folex), and cyclosporine
(Sandimmune/Neoral); anti-inflammatory agents,
such as colchicines
These agents may inhibit immune reactions that
mediate inflammatory processes and progression
of the disease.
Electrolytes Corrects imbalances and may improve cerebral
function and metabolism of ammonia.
Stool softeners, colonic purges such as magnesium
sulfate, enemas, and lactulose
Removes protein and blood from intestines.
Acidifying the intestine produces diarrhea and
decreases production of nitrogenous substances,
reducing risk or severity of encephalopathy. Note:
Long-term use of lactulose may be required for
clients with hepatic encephalopathy to reduce
ammonia on a daily or regular basis.
Bactericidal agents, such as neomycin (Mycifradin)
and kanamycin (Kantrex)
Destroys intestinal bacteria, reducing production of
ammonia, to prevent encephalopathy.
Administer supplemental O2. Mentation is affected by O2 concentration and
utilization in the brain.
Assist with procedures as indicated, such as dialysis,
plasmapheresis, or extracorporeal liver perfusion.
May be used to reduce serum ammonia levels if
encephalopathy develops or other measures are
not successful.
NURSING DIAGNOSIS: Self-Esteem [specify]/disturbed Body Image
May be related to
Biophysical changes, altered physical appearance
Uncertainty of prognosis, changes in role function
Personal vulnerability
Self-destructive behavioralcohol-induced disease
Possibly evidenced by
Verbalization of change or restriction in lifestyle
Fear of rejection or reaction by others
Negative feelings about body and abilities
Feelings of helplessness, hopelessness, or powerlessness
Desired Outcomes/Evaluation CriteriaClient Will
Self-Esteem NOC
Verbalize understanding of changes and acceptance of self in the present situation.
Identify feelings and methods for coping with negative perception of self.
ACTIONS/INTERVENTIONS RATIONALE
Self-Esteem Enhancement NIC
Independent
Discuss situation and encourage verbalization of
fears and concerns. Explain relationship between
nature of disease and symptoms.
Client is very sensitive to body changes and may
also experience feelings of guilt when cause is
related to alcohol or other drug use.
Support and encourage client; provide care with a
positive, friendly attitude.
Caregivers sometimes allow judgmental feelings to
affect the care of client and need to make every
effort to help client feel valued as a person.
Encourage family/SO to verbalize feelings, visit
freely, and participate in care.
Family/SO may feel guilty about clients condition
and may be fearful of impending death. They
need nonjudgmental emotional support and free
access to client. Participation in care helps them
feel useful and promotes trust between staff,
client, and family/SO.
Assist client/SO to cope with change in appearance;
suggest clothing that does not emphasize altered
appearance, such as use of red, blue, or black
clothing.
Client may present unattractive appearance as a
result of jaundice, ascites, and ecchymotic areas.
Providing support can enhance self-esteem and
promote clients sense of control.
Collaborative
Refer to support services, such as counselors,
psychiatric resources, social service, clergy, and
alcohol treatment program.
Increased vulnerability and concerns associated with
this illness may require services of additional
professional resources.
NURSING DIAGNOSIS: deficient Knowledge [Learning Need] regarding
condition, prognosis, treatment, self-care, and discharge needs
May be related to
Lack of exposure or recall; information misinterpretation
Unfamiliarity with information resources
Possibly evidenced by
Questions, request for information, statement of misconception
Inaccurate follow-through of instructions, development of preventable complications
Desired Outcomes/Evaluation CriteriaClient Will
Knowledge: Illness Care NOC
Verbalize understanding of disease process, prognosis, and potential complications.
Correlate symptoms with causative factors.
Knowledge: Health Behaviors NOC
Identify and initiate necessary lifestyle changes.
Actively participate in care.
ACTIONS/INTERVENTIONS RATIONALE
Teaching: Disease Process NIC
Independent
Review disease process and future expectations. Provides knowledge base from which client can
make informed choices.
Emphasize importance of avoiding alcohol. Give
information about medical and community
services available to aid in alcohol rehabilitation, if
indicated.
Alcohol is one of the leading causes for the
development of cirrhosis.
Inform client of altered effects of medications with
cirrhosis and the importance of using only drugs
prescribed or cleared by a healthcare provider
who is familiar with clients history.
Some drugs are hepatotoxic, especially opioids,
sedatives, and hypnotics. In addition, the
damaged liver has a reduced ability to metabolize
all drugs, potentiating cumulative effect and
aggravation of bleeding tendencies.
Review procedure for maintaining function of
peritoneovenous shunt when present.
Several types of shunts are available, so it is
important that client and SO understand care
needed for clients shunt. For example, Denver
shunt requires client to periodically pump the
chamber to maintain patency of the device, and
client with a LeVeen shunt may wear an
abdominal binder or engage in a Valsalvas
maneuver to maintain shunt function.
Assist client with identifying support person(s). Because of length of recovery, potential for relapses,
and slow convalescence, support systems are
extremely important in maintaining behavior
modifications.
Emphasize the importance of good nutrition.
Recommend avoidance of high-protein and salty
foods, onions, and strong cheeses. Provide
written dietary instructions.
Proper dietary maintenance and avoidance of foods
high in sodium and protein aid in remission of
symptoms and help prevent ammonia buildup and
further liver damage. Written instructions are
helpful for client to refer to at home.
Stress necessity of follow-up care and adherence to
therapeutic regimen.
Chronic nature of disease has potential for life-
threatening complications. Provides opportunity
for evaluation of effectiveness of regimen,
including patency of shunt if used.
Discuss sodium and salt substitute restrictions and
necessity of reading labels on food, OTC drugs,
Minimizes ascites and edema formation. Overuse of
substitutes may result in other electrolyte
and herbal agents. imbalances. Food, OTC medications, and personal
care products, including antacids and some
mouthwashes, may contain sodium or alcohol and
may be toxic to the liver or be primarily
metabolized by the liver.
Encourage scheduling activities with adequate rest
periods.
Adequate rest decreases metabolic demands on the
body and increases energy available for tissue
regeneration.
Promote diversional activities that are enjoyable to
client.
Prevents boredom, facilitates rest, and minimizes
anxiety and depression.
Recommend avoidance of persons with infections,
especially upper respiratory infections.
Decreased resistance, altered nutritional status, and
impaired immune responses potentiate risk of
infection.
Instruct client and SO of signs and symptoms that
warrant notification of healthcare provider, such
as increased abdominal girth, rapid weight loss or
gain, increased peripheral edema, increased
dyspnea, fever, blood in stool or urine, excess
bleeding of any kind, and jaundice.
Prompt reporting of symptoms provides opportunity
to treat complications before they become life-
threatening. Note: Client may be evaluated for
additional medical or surgical interventions,
including liver transplantation.
Instruct SO to notify healthcare providers of any
confusion, untidiness, night wandering, tremors,
or personality change.
Changes reflecting deterioration in mental status may
be apparent to SO, although insidious changes
may be noted by others with less frequent
contact with client.
POTENTIAL CONSIDERATIONS following acute hospitalization (dependent on clients age,
physical condition and presence of complications, personal resources, and life responsibilities)
Fatiguedecreased metabolic energy production, states of discomfort, altered body chemistry,
such as changes in liver function, effect on target organs, alcohol withdrawal
imbalanced Nutrition: Less than Body Requirementsinadequate diet, inability to process and
digest nutrients, anorexia, nausea and vomiting, indigestion, early satiety (ascites), abnormal
bowel function
risk for ineffective self Health Managementperceived benefit, social support deficit, economic
difficulties.
dysfunctional Family Processesabuse of alcohol, resistance to treatment, inadequate coping
and lack of problem-solving skills, addictive personality and codependency
risk for Caregiver Role Strainaddiction or codependency; family dysfunction before caregiving
situation; presence of situational stressors, such as economic vulnerability, hospitalization,
changes in employment
You might also like
- Presentation on Cirrhosis of LiverDocument34 pagesPresentation on Cirrhosis of LiverAnshu kumariNo ratings yet
- Notes Liver CirrhosisDocument10 pagesNotes Liver CirrhosisSanthu SuNo ratings yet
- Chapter 8Document89 pagesChapter 8Harith AtrisNo ratings yet
- Liver Cirrhosis, A Simple Guide To The Condition, Treatment And Related DiseasesFrom EverandLiver Cirrhosis, A Simple Guide To The Condition, Treatment And Related DiseasesNo ratings yet
- 3 Liver CirrhosisDocument50 pages3 Liver CirrhosisKamal AhmedNo ratings yet
- Chronic Liver FailureDocument4 pagesChronic Liver FailureJasmine Faith SilvaNo ratings yet
- NCM 30 Study Guide On The ChildDocument6 pagesNCM 30 Study Guide On The ChildJai - HoNo ratings yet
- CirrhoisDocument6 pagesCirrhoisAslimah RakimNo ratings yet
- Chronic Liver FailureDocument25 pagesChronic Liver FailureMohamed Na3eemNo ratings yet
- Disorders of The Hepatobiliary System: Dr. Mehzabin AhmedDocument27 pagesDisorders of The Hepatobiliary System: Dr. Mehzabin Ahmedbpt2100% (1)
- Sirrhosis HatiDocument6 pagesSirrhosis HatikimokberusungNo ratings yet
- Liver CirrhosisDocument2 pagesLiver CirrhosisAzette Agpi100% (3)
- Prezentare Ciroza Eng Semne Si SimptDocument64 pagesPrezentare Ciroza Eng Semne Si SimptDăscălașu CatalinaNo ratings yet
- Activity 8-Liver Cirrhosis-DonghitDocument8 pagesActivity 8-Liver Cirrhosis-DonghitAllona Jane Beatrice DonghitNo ratings yet
- Hepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijDocument69 pagesHepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Module 15 Diets For Diseases of The Liver 2Document13 pagesModule 15 Diets For Diseases of The Liver 2WendellNo ratings yet
- Liver Functions & Diseases ExplainedDocument19 pagesLiver Functions & Diseases ExplainedRacha MougharbelNo ratings yet
- Acute Liver FailureDocument3 pagesAcute Liver FailureElisabeth F. OjhaNo ratings yet
- Examen IM-gastroenterologieDocument15 pagesExamen IM-gastroenterologieNicola BereholschiNo ratings yet
- Liver Cirrhosis CaseDocument8 pagesLiver Cirrhosis Casemarlx5No ratings yet
- Liver, Biliary Tract and Pancreas ProblemsDocument95 pagesLiver, Biliary Tract and Pancreas ProblemsBav VAansoqnuaetzNo ratings yet
- FLDDocument16 pagesFLDTselmeg TselmegNo ratings yet
- Primary Biliary CholangitisDocument23 pagesPrimary Biliary CholangitisAbdul hadiNo ratings yet
- Cirrhosis of LiverDocument35 pagesCirrhosis of LiverShazia Parveen100% (1)
- Cirrhosis: Liver Damage and FibrosisDocument20 pagesCirrhosis: Liver Damage and FibrosisMike GNo ratings yet
- Understanding Jaundice: Causes, Types, Symptoms & TreatmentDocument30 pagesUnderstanding Jaundice: Causes, Types, Symptoms & TreatmentAtharva DeshmukhNo ratings yet
- Liver CirhosisDocument15 pagesLiver CirhosisMoslem abd alzahra aziz AlsialwyNo ratings yet
- Take Home Exam - Ali, Habiba L.Document5 pagesTake Home Exam - Ali, Habiba L.hally_lipNo ratings yet
- Cirrhosis of Liver: Shemil Clinical Instructor DmwimsDocument25 pagesCirrhosis of Liver: Shemil Clinical Instructor DmwimsSrihari DivyaNo ratings yet
- Liver CirrohosisDocument157 pagesLiver CirrohosisSeema SachdevaNo ratings yet
- Lec 9 Part2 Liver CirrhosisDocument16 pagesLec 9 Part2 Liver CirrhosisRussia Al ShboulNo ratings yet
- Hepatic CirrhosisDocument20 pagesHepatic CirrhosisAnifowose samsonNo ratings yet
- Med Surg Test 4 Study GuideDocument29 pagesMed Surg Test 4 Study GuideJessNo ratings yet
- Topic List Q&ADocument63 pagesTopic List Q&APop D. MadalinaNo ratings yet
- Understanding Cirrhosis of the LiverDocument16 pagesUnderstanding Cirrhosis of the LiverAmanda ScarletNo ratings yet
- Acute Renal Failure & Chronic Renal FailureDocument38 pagesAcute Renal Failure & Chronic Renal FailureArti GondNo ratings yet
- CirrhosisDocument56 pagesCirrhosisJerson IngnoNo ratings yet
- CirrhosisDocument40 pagesCirrhosisyohannesNo ratings yet
- NephritisDocument16 pagesNephritisyikesNo ratings yet
- Chronic Liver DiseasesDocument43 pagesChronic Liver DiseasesDickson Luvi100% (1)
- Causes: o o o oDocument5 pagesCauses: o o o oyarem01No ratings yet
- Fulminant Hepatic FailureDocument50 pagesFulminant Hepatic FailureSangeeta BSRNo ratings yet
- Liver Cirrhosis GuideDocument8 pagesLiver Cirrhosis GuidegoyaNo ratings yet
- Liver Transplant Workup: IntroductionDocument9 pagesLiver Transplant Workup: IntroductionKay BristolNo ratings yet
- Sily MarinDocument6 pagesSily MarinBanc OanaNo ratings yet
- Cirrhosis of Liver, Liver Cancer, HepatitisDocument72 pagesCirrhosis of Liver, Liver Cancer, HepatitisBabita DhruwNo ratings yet
- Hemolytic Uremic Syndrome: By: Ankita Gupta 19580027Document15 pagesHemolytic Uremic Syndrome: By: Ankita Gupta 19580027Ankita guptaNo ratings yet
- Hepatosis - fatty liverDocument17 pagesHepatosis - fatty liverPriyamNo ratings yet
- Exam 3 Path o PhysiologyDocument8 pagesExam 3 Path o PhysiologyJennifer JaworskyNo ratings yet
- Liver Cell FailureDocument12 pagesLiver Cell Failureasmyr6975No ratings yet
- My Case Study of Liver CirrhosisDocument13 pagesMy Case Study of Liver Cirrhosisdysphile100% (1)
- Cirrhosis Diagnosis and TreatmentDocument4 pagesCirrhosis Diagnosis and TreatmentMANGNo ratings yet
- Drugs in Liver Disease - MedicineDocument26 pagesDrugs in Liver Disease - MedicineDahbi YassineNo ratings yet
- Diseases of Hepato-Biliary SystemDocument30 pagesDiseases of Hepato-Biliary SystemRupak PandeyNo ratings yet
- Cirrhosis Jol 2009Document54 pagesCirrhosis Jol 2009SaaraAlleyahAlAnazi100% (1)
- Cirrhosis Complications: Causes, Symptoms, and TreatmentDocument50 pagesCirrhosis Complications: Causes, Symptoms, and Treatmentnathan asfahaNo ratings yet
- Nutrition and Liver DiseaseDocument27 pagesNutrition and Liver Diseaseahmed razNo ratings yet
- 97Document79 pages97HATLERNo ratings yet
- Liver Cirrhosis: Irish Nicole Dela Cruz Gessel Ann BoguenDocument79 pagesLiver Cirrhosis: Irish Nicole Dela Cruz Gessel Ann BoguenIrish Nicole DCNo ratings yet
- Cirrhosisoftheliver 2016Document4 pagesCirrhosisoftheliver 2016Nazimr RazaNo ratings yet
- Solved To Evaluate Whether Pre Surgery Patient Attitudes Affect Recovery and UltimateDocument1 pageSolved To Evaluate Whether Pre Surgery Patient Attitudes Affect Recovery and UltimateAnbu jaromiaNo ratings yet
- EuroQoL Quality of Life Scale (EQ-5D) PDFDocument2 pagesEuroQoL Quality of Life Scale (EQ-5D) PDFCicci HoffNo ratings yet
- Karyotype ProjectDocument4 pagesKaryotype ProjectShreya DharmaNo ratings yet
- Protooncogene Tyrosineprotein Kinase Srcrelated Mouth Pyogenic Granuloma An Investigation Involving 2 InstanceskermbDocument2 pagesProtooncogene Tyrosineprotein Kinase Srcrelated Mouth Pyogenic Granuloma An Investigation Involving 2 Instanceskermbsaucebelief33No ratings yet
- Nur 205 1 Exam 1 Study GuideDocument10 pagesNur 205 1 Exam 1 Study Guidesylphlike5No ratings yet
- Dental Rest Seats GuideDocument42 pagesDental Rest Seats GuideAhmad Khalid HumidatNo ratings yet
- Elekta Infinity™ BrochureDocument12 pagesElekta Infinity™ BrochureDC ShekharNo ratings yet
- Arjun Pts Orem - Sumitra DeviDocument13 pagesArjun Pts Orem - Sumitra DeviChandan PradhanNo ratings yet
- Schizoaffective DisorderDocument6 pagesSchizoaffective DisorderJenish FitnessCoachNo ratings yet
- Dental Implant Awareness Among Patients in Our Institution in Chennai-Cross-Sectional SurveyDocument4 pagesDental Implant Awareness Among Patients in Our Institution in Chennai-Cross-Sectional SurveyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 50 Item Medical-Surgical Nursing Test DrillDocument17 pages50 Item Medical-Surgical Nursing Test DrillFilipino Nurses CentralNo ratings yet
- Psychology Disorders PresentationDocument15 pagesPsychology Disorders PresentationDhriti ChughNo ratings yet
- Nursing ResumeDocument3 pagesNursing Resumeapi-313972870No ratings yet
- Scholarship ExamDocument16 pagesScholarship ExamRicky Vanguardia IIINo ratings yet
- Drug Study Nov. 12Document6 pagesDrug Study Nov. 12Jenny Ajoc100% (4)
- Bruxism (Tooth Grinding) in Adults: SymptomsDocument3 pagesBruxism (Tooth Grinding) in Adults: SymptomsalgaipNo ratings yet
- AP Psych Midterm Study Guide 09-10 ObjDocument4 pagesAP Psych Midterm Study Guide 09-10 Objmrsaborges0% (1)
- Artificial Intelligence in HealthcareDocument3 pagesArtificial Intelligence in HealthcareBaekhyunee PubbyNo ratings yet
- Elizabeth Wettlaufer - Agreed Statement of FactsDocument57 pagesElizabeth Wettlaufer - Agreed Statement of FactsNick Westoll100% (3)
- Renal Failure and Kidney DiseaseDocument41 pagesRenal Failure and Kidney Disease12046No ratings yet
- NUH Values and Behaviours BookletDocument28 pagesNUH Values and Behaviours BookletEverjoyNo ratings yet
- PT IDS Medical Systems Indonesia Price List E-CatalogueDocument28 pagesPT IDS Medical Systems Indonesia Price List E-Cataloguekoes marNo ratings yet
- Chapter 9: Communication and The Therapeutic RelationshipDocument3 pagesChapter 9: Communication and The Therapeutic RelationshipKINDATNo ratings yet
- PESTLE Analysis of Square PharmaDocument3 pagesPESTLE Analysis of Square PharmaMuddasir NishadNo ratings yet
- Pharmacokinetics Compartment ModelingDocument94 pagesPharmacokinetics Compartment ModelingPinkishBlue100% (1)
- Leaked Sha Covid-19 PlanDocument20 pagesLeaked Sha Covid-19 PlanKatelyn Guignard100% (1)
- Myofascial Pain Syndrome in The Pelvic FloorDocument31 pagesMyofascial Pain Syndrome in The Pelvic FlooralgomohsinNo ratings yet
- CA Keats Chagolla Safe Triage Pregnant Patients Emergency Room-1Document39 pagesCA Keats Chagolla Safe Triage Pregnant Patients Emergency Room-1samsiahNo ratings yet
- Asthma PhenotypesDocument55 pagesAsthma PhenotypesAnonymous so6ZnlKywNo ratings yet
- Mefenamic AcidDocument2 pagesMefenamic AcidXtinego100% (1)