Professional Documents
Culture Documents
Referat Besar
Uploaded by
Nur_FaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Referat Besar
Uploaded by
Nur_FaCopyright:
Available Formats
BMJ 2013;346:f2634 doi: 10.1136/bmj.
f2634 (Published 8 May 2013)
Page 1 of 7
Clinical Review
CLINICAL REVIEW
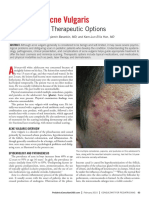
Acne vulgaris
1
Annelise L Dawson medical resident , Robert P Dellavalle chief
234
Department of Internal Medicine, Brigham and Womens Hospital, Boston, MA, USA; 2Department of Dermatology, University of Colorado Denver,
Aurora, Colorado, USA; 3Dermatology Service, Department of Veterans Affairs Medical Center, Denver, CO 80220, USA ; 4Department of
Epidemiology, Colorado School of Public Health, University of Colorado Denver, Aurora, CO, USA
1
Acne vulgaris is a common inflammatory skin condition.
Although often perceived as a self limited disease of
adolescence, its prevalence remains high into adulthood. Nearly
90% of teenagers have acne, and half of them continue to
experience symptoms as adults.1-3 By age 40 years, 1% of men
and 5% of women still have lesions.4 Recent analyses show an
increasing prevalence of acne in children, perhaps because of
pubertal onset.5
Given that acne may persist for decades and require long term
therapy, there has been a recent effort to reclassify acne as a
chronic disease.2 6 Acne has clear detrimental psychosocial
effects and may lead to permanent scarring.7 It is therefore not
surprising that patients are motivated to seek medical care. In
the United Kingdom, acne accounts for more than 3.5 million
annual visits to general practitioners,3 8 who must therefore be
equipped to treat acne. Several prominent groupsincluding
the Global Alliance to Improve Outcomes in Acne, the European
Dermatology Forum, and the American Academy of
Dermatologyhave published comprehensive treatment
recommendations detailing comparable therapeutic strategies.9-11
Here we provide a streamlined outline of treatment intended for
the non-specialist.
What are the clinical characteristics of
acne?
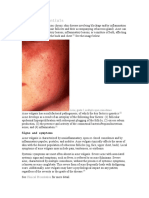
A spectrum of lesions may be present, including
non-inflammatory open and closed comedones (blackheads and
whiteheads, respectively) and inflammatory papules, pustules,
nodules, and cysts. Lesions may be present on the face, neck,
chest, or backareas with the greatest density of pilosebaceous
units.12 Comedone formation is intrinsic to the diagnosis of acne
vulgariswhen not clinically apparent, consider alternative
diagnoses. Diseases that mimic acne include rosacea, folliculitis,
angiofibromas, perioral dermatitis, and keratosis pilaris.5 13 14
The patients age may also help to distinguish these disorders
from acne. Keratosis pilaris and perioral dermatitis, for example,
tend to present in childhood, whereas rosacea tends to affect
older adults. In cases of diagnostic uncertainty, referral to
specialist care is warranted.
Several groups have proposed standardized measures for
classifying acne, although none has been universally
accepted.10 13 15 Classification is important because it helps to
inform treatment strategies.3 11 Acne is categorized broadly into
mild, moderate, and severe forms. Mild acne is typically limited
to the face and is characterized by the presence of
non-inflammatory closed and open comedones with few
inflammatory lesions. Moderate acne is characterized by an
increased number of inflammatory papules and pustules on the
face and often mild truncal disease. Finally, acne is considered
to be severe when nodules and cysts are present. In these cases,
facial lesions are often accompanied by widespread truncal
disease.
What causes acne?
Acne is an inflammatory disease of the pilosebaceous duct that
results from four primary pathophysiologic processes:
Abnormal keratinocyte proliferation and desquamation that
leads to ductal obstruction
Androgen driven increase in sebum production
Proliferation of Propionibacterium acnes
Inflammation.2 9 13 16 17
Increased androgen production causes abnormal epithelial
desquamation and follicular obstruction, which lead to the
primary precursor lesion in acnethe microcomedone.
Microcomedones are pathological structures not visible to the
naked eye that evolve into visible lesions.18 An increase in
circulating androgens also promotes sebum production, causing
these obstructed follicles to fill with lipid rich material and form
visible open and closed comedones.12 19 Sebum serves as a
substrate for bacterial growth, leading to proliferation of P acnes.
Finally, P acnes releases chemical mediators that promote
inflammation, which is propagated by traumatic rupture of
comedones into the surrounding dermis.2 17 This inflammation
manifests through the development of inflammatory papules,
pustules, nodules, and cysts.
Correspondence to: R P Dellavalle, Dermatology Service, Department of Veteran Affairs Medical Center, Denver, CO, USA
robert.dellavalle@ucdenver.edu
For personal use only: See rights and reprints http://www.bmj.com/permissions
Subscribe: http://www.bmj.com/subscribe
BMJ 2013;346:f2634 doi: 10.1136/bmj.f2634 (Published 8 May 2013)
Page 2 of 7
CLINICAL REVIEW
Summary points
Do not underestimate the impact of acne on patient quality of life and mental health
Topical retinoids are now a mainstay of treatment
Avoid prolonged antibiotic courses and antibiotic monotherapy because of the risk of bacterial resistance
For women with refractory acne or lesions confined to the lower half of the face, consider the addition of combined oral contraceptives
Oral isotretinoin is the most effective treatment for severe acne
Assess treatment adherence, which may be limited by irritation or regimen complexity
Sources and selection criteria
We performed a Medline database search using the term acne together with antibiotic resistance, antibiotics, azelaic acid, benzoyl
peroxide, classification, depression, diet, epidemiology, isotretinoin, oral contraceptives, pathogenesis, retinoids, scarring,
smoking, treatment, treatment guidelines, and vulgaris. We also searched the Cochrane Database of Systematic Reviews using the
term acne.
The successful management of acne requires an understanding
of these four facets of the pathophysiology of acne. Clinicians
should select mechanistically driven treatment regimens that
target each patients predominant lesion types.
Can acne be prevented?
Myths about the causes of acne abound. The central
discoloration in blackheads is not dirt, but oxidized melanin.20
A comprehensive systematic review found little evidence for
an association between acne and poor facial hygiene and
provided minimal support for frequent face washing.21
Aggressive cleansing may cause irritation, thereby exacerbating
active lesions or limiting the patients tolerance of therapy.21 22
Basic care with twice daily washing and use of a moisturizer
that does not contribute to comedone formation
(noncomedogenic) is an accepted standard.9 Although
misconceptions about dietary triggers have been largely
dispelled, recent reportsincluding a systematic review of
dietary influences on acne and a randomized investigator masked
controlled trial of glycemic load and acne severitysuggest
that acne is associated with high dairy diets and those with a
high glycemic load.23-27 Finally, a cross sectional analysis found
a significant dose dependent association between smoking and
acne severity.20 28
How is acne treated?
Careful assessment of the morphology and severity of acne is
an important first step in management, because lesion
morphology largely dictates the optimal treatment approach.
Treatment should be designed to target precursor lesions
(microcomedones) and active inflammatory lesions. Milder
cases are best managed with topical regimens, whereas systemic
drugs are indicated in more severe cases. The box summarises
the mechanisms of action of the most commonly used agents.
The table provides a treatment framework based on disease
severity.
Topical agents
Retinoids
Retinoids are vitamin A derivatives that normalize keratinocyte
desquamation and adhesion, leading to comedolysis and
preventing formation of new microcomedones. Some retinoids
also display anti-inflammatory properties.11 15 29-32 Perhaps the
most notable recent development in the treatment of acne is the
increased use of topical retinoids.29 Many randomized trials
show the efficacy of these drugs relative to vehicle, and they
For personal use only: See rights and reprints http://www.bmj.com/permissions
are recommended for all cases of acne, except when oral
retinoids are used.9 11 Studies show improvements within weeks,
with maximal benefit after three to four months.13 15 18 Mild
non-inflammatory comedonal acne may be treated with retinoid
monotherapy. When inflammatory lesions are present, retinoids
should be combined with antimicrobial therapy or benzoyl
peroxide.9 16 Because retinoids prevent the development of
microcomedones, they can also be used for maintenance
therapy.9
Several topical retinoid products exist, including tretinoin,
isotretinoin (not available in the United States), adapalene, and
tazarotene (not licensed for treatment of acne in the United
Kingdom).18 These products are available in cream, gel, liquid,
and microsphere formulations, each at multiple concentrations.
Formulations vary by country.9 18 Use of retinoids is limited by
transient skin irritation, which may be prevented by selecting
lower concentration or cream based formulations.18 29 31 A
meta-analysis of five randomized controlled trials suggests that
adapalene is the best tolerated retinoid, whereas several
moderately sized randomized studies found tazarotene to be
most efficacious at the expense of irritation.13 18 29 31-38 In addition,
anecdotal evidence suggests that some patients experience an
initial flare in acne lesions, which subsides with continued
use.2 18 31 Lastly, pregnant and breastfeeding women should
avoid topical retinoids.18 Women of child bearing age should
be counselled about the need for contraception.17
Topical antibiotics
The primary topical antibiotics used for acne are clindamycin
and erythromycin.30 These agents have bacteriostatic and
anti-inflammatory properties.11 30 32 Topical antibiotics are used
for mild to moderate acne when inflammatory lesions are
present.16
Antibiotic resistance is a growing concern and has prompted
efforts to limit the duration of antibiotic courses and to
emphasize combined regimens.2 Patterns of P acnes resistance
correspond to trends in antibiotic use.2 39 Treatment outcomes
worsen when resistance is presentsystematic reviews show
decreasing antibiotic efficacy over time, particularly for
erythromycin and clindamycin.2 32 40 41 P acnes resistance is not
the only concernStaphylococcus and Streptococcus resistance
may also develop.39 42 In practice, this means avoiding antibiotic
monotherapy and maintenance therapy.19 20 Instead, topical
antibiotics should always be used with retinoids, and possibly
benzoyl peroxide. Several double blind randomized controlled
trials have found that the addition of retinoid or benzoyl peroxide
therapy to topical antibiotics improves treatment
outcomes.9 10 17 39 43 44 Retinoids do not decrease resistance but
Subscribe: http://www.bmj.com/subscribe
BMJ 2013;346:f2634 doi: 10.1136/bmj.f2634 (Published 8 May 2013)
Page 3 of 7
CLINICAL REVIEW
Effects of the different agents used to treat acne
Topical retinoids: Comedolytic and sometimes anti-inflammatory
Antibiotics: Antimicrobial and anti-inflammatory
Benzoyl peroxide: Antimicrobial plus weakly anti-inflammatory and comedolytic
Hormonal agents: Sebosuppressive
Oral retinoids: Comedolytic, sebosuppressive, antimicrobial, and anti-inflammatory
promote antibiotic efficacy by improving penetration and
providing synergistic comedolytic and anti-inflammatory
effects.18 45 Benzoyl peroxide has bactericidal properties, thereby
minimizing bacterial resistance.39 45 Topical antibiotic courses
should be limited to 12 weeks duration when possible.9 16 46
Finally, combined topical and oral antibiotics should be
avoided.15 47
Administration, although it has been approved in many European
countries, so receives greater emphasis in the European
literature.10 55 A small double blind randomized trial
demonstrated efficacy of azelaic acid relative to placebo.56
Studies comparing azelaic acid with other topical agents are
limited. Azelaic acid is well tolerated but poses a risk of
hypopigmentation in darker skinned patients.17
Benzoyl peroxide
Salicylic acid
Benzoyl peroxide is a non-antibiotic antimicrobial agent that
has bactericidal effects by generating reactive oxygen species
within the follicle.15 32 48 49 It also has weak comedolytic and
anti-inflammatory properties.32 Owing to its bactericidal
properties, benzoyl peroxide produces rapid improvement in
inflammatory lesions and prevents the development of antibiotic
resistance.15 32 39 45 48-52 Although data on the comparative efficacy
and tolerability of benzoyl peroxide and topical retinoid
monotherapy are conflicting, most guidelines recommend a
mechanistically driven approach, with the addition of benzoyl
peroxide mainly when inflammatory lesions are present.9 10 17
Some studies, including a small double blind randomized trial,
show that inflammatory lesions improve more rapidly with
benzoyl peroxide than with topical retinoids.53
Benzoyl peroxide is available in numerous formulations, in
concentrations ranging from 2.5% to 10%,29 none of which show
clear superiority in systematic reviews, although irritation
increased with higher concentrations.27 32 48 52 Irritation typically
resolves with continued use. In addition, patients should be
warned that benzoyl peroxide may bleach clothing, bedding,
and hair.13 32 Finally, because all retinoids except adapalene are
unstable with benzoyl peroxide, these agents should be applied
separately.18 31 32
Combination products
The benefits of combined regimens include complementary
mechanisms of action, reduced risk of antibiotic resistance, and
improved treatment outcomes.2 9 10 13 15 17 18 30 47 48 An increasing
number of antibiotic-retinoid and antibiotic-benzoyl peroxide
combinations are now available. Retinoid-benzoyl peroxide
combinations are limited by retinoid instability in the presence
of benzoyl peroxide.
The biggest drawback to combined products is cost. Individual
generic components are typically less expensive and can be
applied simultaneously with equivalent effects.32 46 Nevertheless,
a small investigator blinded randomized controlled trial found
that combined products improve patient adherence by
simplifying daily regimens.54 For many clinicians and patients,
this improved ease of application and corresponding increase
in adherence justifies the cost of combined therapies.
Other topical treatments
Azelaic acid
Azelaic acid is an alternative to retinoids that has comedolytic,
antimicrobial, and anti-inflammatory properties.9 13 17 This agent
has not been approved for acne by the US Food and Drug
For personal use only: See rights and reprints http://www.bmj.com/permissions
Salicylic acid is an over-the-counter agent with desquamating
and comedolytic properties that is less potent than retinoids.48
Few studies of salicylic acid exist, although available studies
show that it is less effective but better tolerated than other
agents.17 29 48 Salicylic acid may be used when patients cannot
tolerate standard agents.
Systemic agents
Systemic agents should be considered for patients with moderate
to severe acne. These therapies are useful in patients with truncal
disease in whom application of topical agents would be difficult.
Hormonal therapies
Hormonal therapies are a useful adjunct to treatment in women
with moderate to severe acne, especially those who desire oral
contraception or in whom traditional therapy has failed.27
Anecdotal evidence suggests that women with lesions confined
to the lower face and jaw are most likely to benefit.15 57
Hormonal agents are available in two primary forms: combined
oral contraceptives, which suppress ovarian androgen
production, and androgen receptor blockers, such as cyproterone
acetate, spironolactone, and flutamide. In the UK, a combined
oral contraceptive containing cyproterone acetate and
ethinylestradiol is licensed for the treatment of acne.13 57 58 These
agents decrease androgen mediated effects on the sebaceous
follicle.57 Although hyperandrogenic states such as polycystic
ovarian syndrome are associated with acne, most women with
acne have normal androgen levels but still benefit from
antiandrogen therapy.57 Full benefit is seen after three to six
months of treatment.15
A recent Cochrane review confirmed the efficacy of combined
oral contraceptives in treating inflammatory and
non-inflammatory acne but found few differences in efficacy
between the different types, including cyproterone acetate, which
is often recommended.59 60 It is therefore not clear whether
formulations containing cyproterone acetate should be favored,
especially because this agent may increase the risk of venous
thromboembolism.27 57 59 Progesterin only contraceptives may
worsen acne.9
Oral antibiotics
Systemic antibiotics are indicated for moderate to severe
inflammatory acne.9 Like topical antibiotics, oral antibiotics
have antimicrobial and anti-inflammatory effects.13 39 50
Doxycycline, minocycline, lymecycline, tetracycline, and
Subscribe: http://www.bmj.com/subscribe
BMJ 2013;346:f2634 doi: 10.1136/bmj.f2634 (Published 8 May 2013)
Page 4 of 7
CLINICAL REVIEW
A patients story
I first developed acne in high school. My family encouraged me to wash my face often with several over-the-counter products, which mostly
exacerbated my symptoms. I was so embarrassed about my skin that I started to avoid spending time with friends. When my mother noticed
this change, she agreed to take me to a dermatologist, who suggested topical antibiotics and benzoyl peroxide. These treatments caused
substantial irritation, so I stopped using them promptly. I was sure that my acne was incurable, so I learned to live with it.
When I reached adulthood, I began taking oral contraceptive pills, not knowing that they could affect the acne. Within a month of starting
treatment, my acne improved dramatically. After six months, my lesions had nearly disappeared. I was thrilled to be disease free for the first
time in nearly a decade but felt sad that this therapy had not been offered to me years earlier. I suspect this would have substantially improved
my teenage confidence and self esteem.
erythromycin are most commonly used. Few comparative studies
exist, although a systematic review of systemic therapy with
tetracyclines found no antibiotic to be more effective than
another.17 41 46 Although minocycline was previously favored by
clinicians, a recent Cochrane review found no clear evidence
of superiority.61 62 Given the lack of comparative data, antibiotic
selection may be driven by side effect profiles and patterns of
P acnes resistance. Tetracyclines must be avoided in pregnant
women and children given the associated risk of tooth
discoloration. Women of childbearing age should be advised to
use contraception when taking these agents. Doxycyline causes
photosensitivity. In rare cases minocycline leads to skin
hyperpigmentation and drug induced systemic lupus
erythematosus. Limecycline has gained popularity in Europe
but is not available in the US.63 Increasing P acnes resistance
has decreased reliance on erythromycin and tetracycline.11 42 49 50
As with topical antibiotics, oral antibiotics should be combined
with other agents to minimize the development of bacterial
resistance and improve treatment efficacy. Always use oral
antibiotics in conjunction with a topical retinoid or benzoyl
peroxide16 50several small to moderate sized randomized
controlled trials have shown that this increases efficacy.64-66
Assess treatment response at six to eight weeks, at which point
a decision to continue or change antibiotics may be made.50
When possible, limit antibiotic courses to 12 weeks
duration.2 16 46
Isotretinoin
Isotretinoin is remarkably efficacious in the treatment of severe
acne, as well as treatment resistant moderate disease, and is now
the first line treatment in such cases.10 13 Isotretinoin is thought
to target all four components involved in the development of
acne by normalizing follicular desquamation, decreasing sebum
secretion, inhibiting the growth of P acnes, and exerting
anti-inflammatory effects.13 31 49 Given these broad effects and
the potential for adjunctive therapy to compound adverse effects,
isotretinoin is prescribed as monotherapy.
Patients typically complete a 16-24 week course of isotretinoin,
taking 0.5-1 mg per kg per day to target a cumulative dose of
120-150 mg per kg.11 16 49 The dose is slowly increased as
tolerated. Effects are not usually seen for the first one or two
months.67 Meta-analyses show that at least half of patients are
permanently cured after a single course, and only 20% of
patients require repeat treatment.15 17 31 49 68 69 Relapse is most
common in younger patients, in women with hormonally driven
acne, and when goal cumulative dosing is not achieved.31 57 70 71
Use of oral isotretinoin is tightly regulated because of its well
known teratogenic effects and is available through specialist
care only in many countries.42 Female patients must demonstrate
a negative pregnancy test and use contraception.49 Although
charged with having detrimental psychological effects, there is
no clear evidence that isotretinoin leads to depression or
suicidality.72-74 Other adverse reactions include chapped skin,
dry eyes, epistaxis, myalgias, and alterations in serum lipid and
For personal use only: See rights and reprints http://www.bmj.com/permissions
transaminase concentrations, most of which resolve after
treatment is stopped.11 13 31 49
What are the consequences of acne?
Although many people dismiss acne vulgaris as an
inconsequential disease of adolescence, it has clear long lasting
psychosocial and physical effects. Many studies have shown an
association between acne and depression and anxiety,
independent of disease severity.7 75 Psychological effects
improve with treatment.76 Furthermore, acne may cause
permanent scarring that is difficult to correct. Finally, because
of its frequency and chronicity, the economic burden of acne is
substantial, with associated expenditure in the US alone
exceeding $2.5bn (1.64bn; 1.93bn) annually.20 To reduce
these effects, patients with acne should receive early, aggressive,
mechanistically driven therapy.
Contributors: Both authors had full access to the content of this review
and are guarantors. ALD searched the literature, compiled the
references, and drafted the manuscript. RPD critically revised the
manuscript for intellectual content.
Competing interests: We have read and understood the BMJ Group
policy on declaration of interests and declare the following interests:
None.
Provenance and peer review: Commissioned; externally peer reviewed.
Patient consent obtained.
1
2
3
4
5
6
7
8
9
10
11
12
13
14
15
16
17
18
19
20
Yentzer BA, Hick J, Reese EL, Uhas A, Feldman SR, Balkrishnan R. Acne vulgaris in the
United States: a descriptive epidemiology. Cutis 2010;86:94-9.
Thiboutot D, Gollnick H, Bettoli V, Dreno B, Kang S, Leyden JJ, et al. New insights into
the management of acne: an update from the global alliance to improve outcomes in acne
group. J Am Acad Dermatol 2009;60(5 suppl):S1-50.
Purdy S, de Berker D. Acne. BMJ 2006;333:949-53.
Goulden V, Stables GI, Cunliffe WJ. Prevalence of facial acne in adults. J Am Acad
Dermatol 1999;41:577-80.
Friedlander SF, Baldwin HE, Mancini AJ, Yan AC, Eichenfield LF. The acne continuum:
an age-based approach to therapy. Semin Cutan Med Surg 2011;30(3 suppl):S6-11.
Gollnick HP, Finlay AY, Shear N. Can we define acne as a chronic disease? If so, how
and when? Am J Clin Dermatol 2008;9:279-84.
Barnes LE, Levender MM, Fleischer AB Jr, Feldman SR. Quality of life measures for acne
patients. Dermatol Clin 2012;30:293-300, ix.
Newton JN. How cost-effective is oral isotretinoin? Dermatology 1997;195(suppl 1):10-4;
discussion 38-40.
Gollnick H, Cunliffe W, Berson D, Dreno B, Finlay A, Leyden JJ, et al. Management of
acne: a report from a Global Alliance to Improve Outcomes in Acne. J Am Acad Dermatol
2003;49(1 suppl):S1-37.
Nast A, Dreno B, Bettoli V, Degitz K, Erdmann R, Finlay AY, et al. European
evidence-based (S3) guidelines for the treatment of acne. J Eur Acad Dermatol Venereol
2012;26(suppl 1):1-29.
Strauss JS, Krowchuk DP, Leyden JJ, Lucky AW, Shalita AR, Siegfried EC, et al.
Guidelines of care for acne vulgaris management. J Am Acad Dermatol 2007;56:651-63.
Brown SK, Shalita AR. Acne vulgaris. Lancet 1998;351:1871-6.
Haider A, Shaw JC. Treatment of acne vulgaris. JAMA 2004;292:726-35.
Archer CB, Cohen SN, Baron SE. Guidance on the diagnosis and clinical management
of acne. Clin Exp Dermatol 2012;37(suppl 1):1-6.
James WD. Clinical practice. Acne. N Engl J Med 2005;352:1463-72.
Abad-Casintahan F, Chow SK, Goh CL, Kubba R, Miyachi Y, Noppakun N, et al. Toward
evidence-based practice in acne: consensus of an Asian Working Group. J Dermatol
2011;38:1041-8.
Williams HC, Dellavalle RP, Garner S. Acne vulgaris. Lancet 2012;379:361-72.
Thielitz A, Gollnick H. Topical retinoids in acne vulgaris: update on efficacy and safety.
Am J Clin Dermatol 2008;9:369-81.
Chen W, Thiboutot D, Zouboulis CC. Cutaneous androgen metabolism: basic research
and clinical perspectives. J Invest Dermatol 2002;119:992-1007.
Knutsen-Larson S, Dawson AL, Dunnick CA, Dellavalle RP. Acne vulgaris: pathogenesis,
treatment, and needs assessment. Dermatol Clin 2012;30:99-106, viii-ix.
Subscribe: http://www.bmj.com/subscribe
BMJ 2013;346:f2634 doi: 10.1136/bmj.f2634 (Published 8 May 2013)
Page 5 of 7
CLINICAL REVIEW
Areas for future research
Large randomized controlled trials on the treatment of acne are needed
Comparative effectiveness research should be prioritized, as cited by the Institute of Medicine77
Study of the cutaneous microbiome, including disease associations with Propionibacterium acnes strains, may improve our understanding
of the pathogenesis of acne and open up new therapeutic approaches78
Additional educational resources
Resources for healthcare professionals
American Academy of Dermatology: Strauss JS, Krowchuk DP, Leyden JJ, Lucky AW, Shalita AR, Siegfried EC, et al. Guidelines of
care for acne vulgaris management. J Am Acad Dermatol 2007;56:651-63
European Dermatology Forum: Nast A, Dreno B, Bettoli V, Degitz K, Erdmann R, Finlay AY, et al. European evidence-based (S3)
guidelines for the treatment of acne. J Eur Acad Dermatol Venereol 2012;26(suppl 1):1-29
Global Alliance to Improve Oucomes in Acne: Gollnick H, Cunliffe W, Berson D, Dreno B, Finlay A, Leyden JJ, et al. Management of
acne: a report from a Global Alliance to Improve Outcomes in Acne. J Am Acad Dermatol 2003;49(1 suppl):S1-37
National Institute of Health and Care Excellence (www.cks.nhs.uk/acne_vulgaris)Clinical knowledge summary on acne vulgaris
Resources for patients
American Academy of Dermatology (www.aad.org/skin-conditions/dermatology-a-to-z/acne)Basic patient information regarding acne
treatment with particular emphasis on adult acne
British Association of Dermatologists (www.bad.org.uk/site/793/default.aspx)General overview of acne treatment
National Institute of Health and Care Excellence (www.cks.nhs.uk/acne_vulgaris)Clinical knowledge summary on acne vulgaris
UpToDate Patient Information (www.uptodate.com/contents/acne-beyond-the-basics)Patient oriented guide to the pathophysiology
and treatment of acne
21
22
23
24
25
26
27
28
29
30
31
32
33
34
35
36
37
38
39
40
41
42
43
Magin P, Pond D, Smith W, Watson A. A systematic review of the evidence for myths
and misconceptions in acne management: diet, face-washing and sunlight. Fam Pract
2005;22:62-70.
Goodman G. Cleansing and moisturizing in acne patients. Am J Clin Dermatol
2009;10(suppl 1):1-6.
Smith RN, Mann NJ, Braue A, Makelainen H, Varigos GA. The effect of a high-protein,
low glycemic-load diet versus a conventional, high glycemic-load diet on biochemical
parameters associated with acne vulgaris: a randomized, investigator-masked, controlled
trial. J Am Acad Dermatol 2007;57:247-56.
Spencer EH, Ferdowsian HR, Barnard ND. Diet and acne: a review of the evidence. Int
J Dermatol 2009;48:339-47.
Bowe WP, Joshi SS, Shalita AR. Diet and acne. J Am Acad Dermatol 2010;63:124-41.
Ingram JR, Grindlay DJ, Williams HC. Management of acne vulgaris: an evidence-based
update. Clin Exp Dermatol 2010;35:351-4.
Smith EV, Grindlay DJ, Williams HC. Whats new in acne? An analysis of systematic
reviews published in 2009-2010. Clin Exp Dermatol 2011;36:119-22; quiz 23.
Schafer T, Nienhaus A, Vieluf D, Berger J, Ring J. Epidemiology of acne in the general
population: the risk of smoking. Br J Dermatol 2001;145:100-4.
Ramanathan S, Hebert AA. Management of acne vulgaris. J Pediatr Health Care
2011;25:332-7.
Tan HH. Topical antibacterial treatments for acne vulgaris : comparative review and guide
to selection. Am J Clin Dermatol 2004;5:79-84.
Chivot M. Retinoid therapy for acne. A comparative review. Am J Clin Dermatol
2005;6:13-9.
Gamble R, Dunn J, Dawson A, Petersen B, McLaughlin L, Small A, et al. Topical
antimicrobial treatment of acne vulgaris: an evidence-based review. Am J Clin Dermatol
2012;13:141-52.
Cunliffe WJ, Poncet M, Loesche C, Verschoore M. A comparison of the efficacy and
tolerability of adapalene 0.1% gel versus tretinoin 0.025% gel in patients with acne vulgaris:
a meta-analysis of five randomized trials. Br J Dermatol 1998;139(suppl 52):48-56.
Cunliffe WJ, Danby FW, Dunlap F, Gold MH, Gratton D, Greenspan A. Randomised,
controlled trial of the efficacy and safety of adapalene gel 0.1% and tretinoin cream 0.05%
in patients with acne vulgaris. Eur J Dermatol 2002;12:350-4.
Galvin SA, Gilbert R, Baker M, Guibal F, Tuley MR. Comparative tolerance of adapalene
0.1% gel and six different tretinoin formulations. Br J Dermatol 1998;139(suppl 52):34-40.
Leyden JJ, Tanghetti EA, Miller B, Ung M, Berson D, Lee J. Once-daily tazarotene 0.1%
gel versus once-daily tretinoin 0.1% microsponge gel for the treatment of facial acne
vulgaris: a double-blind randomized trial. Cutis 2002;69(2 suppl):12-9.
Webster GF, Guenther L, Poulin YP, Solomon BA, Loven K, Lee J. A multicenter,
double-blind, randomized comparison study of the efficacy and tolerability of once-daily
tazarotene 0.1% gel and adapalene 0.1% gel for the treatment of facial acne vulgaris.
Cutis 2002;69(2 suppl):4-11.
Tanghetti E, Dhawan S, Green L, Del Rosso J, Draelos Z, Leyden J, et al. Randomized
comparison of the safety and efficacy of tazarotene 0.1% cream and adapalene 0.3% gel
in the treatment of patients with at least moderate facial acne vulgaris. J Drugs Dermatol
2010;9:549-58.
Leyden JJ, Del Rosso JQ, Webster GF. Clinical considerations in the treatment of acne
vulgaris and other inflammatory skin disorders: a status report. Dermatol Clin 2009;27:1-15.
Simonart T, Dramaix M. Treatment of acne with topical antibiotics: lessons from clinical
studies. Br J Dermatol 2005;153:395-403.
Simonart T, Dramaix M, De Maertelaer V. Efficacy of tetracyclines in the treatment of
acne vulgaris: a review. Br J Dermatol 2008;158:208-16.
Harper JC. An update on the pathogenesis and management of acne vulgaris. J Am Acad
Dermatol 2004;51(1 suppl):S36-8.
Lookingbill DP, Chalker DK, Lindholm JS, Katz HI, Kempers SE, Huerter CJ, et al.
Treatment of acne with a combination clindamycin/benzoyl peroxide gel compared with
For personal use only: See rights and reprints http://www.bmj.com/permissions
44
45
46
47
48
49
50
51
52
53
54
55
56
57
58
59
60
61
62
63
64
clindamycin gel, benzoyl peroxide gel and vehicle gel: combined results of two double-blind
investigations. J Am Acad Dermatol 1997;37:590-5.
Leyden JJ, Krochmal L, Yaroshinsky A. Two randomized, double-blind, controlled trials
of 2219 subjects to compare the combination clindamycin/tretinoin hydrogel with each
agent alone and vehicle for the treatment of acne vulgaris. J Am Acad Dermatol
2006;54:73-81.
Elston DM. Topical antibiotics in dermatology: emerging patterns of resistance. Dermatol
Clin 2009;27:25-31.
Ozolins M, Eady EA, Avery AJ, Cunliffe WJ, Po AL, ONeill C, et al. Comparison of five
antimicrobial regimens for treatment of mild to moderate inflammatory facial acne vulgaris
in the community: randomised controlled trial. Lancet 2004;364:2188-95.
Simpson RC, Grindlay DJ, Williams HC. Whats new in acne? An analysis of systematic
reviews and clinically significant trials published in 2010-11. Clin Exp Dermatol
2011;36:840-3; quiz 43-4.
Bowe WP, Shalita AR. Effective over-the-counter acne treatments. Semin Cutan Med
Surg 2008;27:170-6.
Newman MD, Bowe WP, Heughebaert C, Shalita AR. Therapeutic considerations for
severe nodular acne. Am J Clin Dermatol 2011;12:7-14.
Del Rosso JQ, Kim G. Optimizing use of oral antibiotics in acne vulgaris. Dermatol Clin
2009;27:33-42.
Cunliffe WJ, Holland KT, Bojar R, Levy SF. A randomized, double-blind comparison of a
clindamycin phosphate/benzoyl peroxide gel formulation and a matching clindamycin gel
with respect to microbiologic activity and clinical efficacy in the topical treatment of acne
vulgaris. Clin Thera 2002;24:1117-33.
Fakhouri T, Yentzer BA, Feldman SR. Advancement in benzoyl peroxide-based acne
treatment: methods to increase both efficacy and tolerability. J Drugs in Dermatol
2009;8:657-61.
Hughes BR, Norris JF, Cunliffe WJ. A double-blind evaluation of topical isotretinoin 0.05%,
benzoyl peroxide gel 5% and placebo in patients with acne. Clin Exp Dermatol
1992;17:165-8.
Yentzer BA, Ade RA, Fountain JM, Clark AR, Taylor SL, Fleischer AB Jr, et al. Simplifying
regimens promotes greater adherence and outcomes with topical acne medications: a
randomized controlled trial. Cutis 2010;86:103-8.
Thiboutot D. Versatility of azelaic acid 15% gel in treatment of inflammatory acne vulgaris.
J Drugs Dermatol 2008;7:13-6.
Iraji F, Sadeghinia A, Shahmoradi Z, Siadat AH, Jooya A. Efficacy of topical azelaic acid
gel in the treatment of mild-moderate acne vulgaris. Indian J Dermatol Venereol Leprol
2007;73:94-6.
George R, Clarke S, Thiboutot D. Hormonal therapy for acne. Semin Cutan Med Surg
2008;27:188-96.
Van Vloten WA, Sigurdsson V. Selecting an oral contraceptive agent for the treatment of
acne in women. Am J Clin Dermatol 2004;5:435-41.
Arowojolu AO, Gallo MF, Lopez LM, Grimes DA, Garner SE. Combined oral contraceptive
pills for treatment of acne. Cochrane Database System Rev 2007;1:CD004425.
Arowojolu AO, Gallo MF, Lopez LM, Grimes DA. Combined oral contraceptive pills for
treatment of acne. Cochrane Database System Rev 2012;7:CD004425.
Garner SE, Eady EA, Popescu C, Newton J, Li WA. Minocycline for acne vulgaris: efficacy
and safety. Cochrane Database System Rev 2003;1:CD002086.
Garner SE, Eady A, Bennett C, Newton JN, Thomas K, Popescu CM. Minocycline for
acne vulgaris: efficacy and safety. Cochrane Database System Rev 2012;8:CD002086.
Bossuyt L, Bosschaert J, Richert B, Cromphaut P, Mitchell T, Al Abadie M, et al.
Lymecycline in the treatment of acne: an efficacious, safe and cost-effective alternative
to minocycline. Eur J Dermatol 2003;13:130-5.
Thiboutot DM, Shalita AR, Yamauchi PS, Dawson C, Arsonnaud S, Kang S. Combination
therapy with adapalene gel 0.1% and doxycycline for severe acne vulgaris: a multicenter,
investigator-blind, randomized, controlled study. Skinmed 2005;4:138-46.
Subscribe: http://www.bmj.com/subscribe
BMJ 2013;346:f2634 doi: 10.1136/bmj.f2634 (Published 8 May 2013)
Page 6 of 7
CLINICAL REVIEW
65
66
67
68
69
70
71
72
Gold LS, Cruz A, Eichenfield L, Tan J, Jorizzo J, Kerrouche N, et al. Effective and safe
combination therapy for severe acne vulgaris: a randomized, vehicle-controlled,
double-blind study of adapalene 0.1%-benzoyl peroxide 2.5% fixed-dose combination gel
with doxycycline hyclate 100 mg. Cutis 2010;85:94-104.
Cunliffe WJ, Meynadier J, Alirezai M, George SA, Coutts I, Roseeuw DI, et al. Is combined
oral and topical therapy better than oral therapy alone in patients with moderate to
moderately severe acne vulgaris? A comparison of the efficacy and safety of lymecycline
plus adapalene gel 0.1%, versus lymecycline plus gel vehicle. J Am Acad Dermatol
2003;49(3 suppl):S218-26.
DiGiovanna JJ. Systemic retinoid therapy. Dermatol Clin 2001;19:161-7.
White GM. Acne therapy. Adv Dermatol 1999;14:29-58; discussion 59.
Wessels F, Anderson AN, Kropman K. The cost-effectiveness of isotretinoin in the
treatment of acne. Part 1. A meta-analysis of effectiveness literature. South Afr Med J
1999;89(7 Pt 2):780-4.
White GM, Chen W, Yao J, Wolde-Tsadik G. Recurrence rates after the first course of
isotretinoin. Arch Dermatol 1998;134:376-8.
Stainforth JM, Layton AM, Taylor JP, Cunliffe WJ. Isotretinoin for the treatment of acne
vulgaris: which factors may predict the need for more than one course? Br J Dermatol
1993;129:297-301.
Goldsmith LA, Bolognia JL, Callen JP, Chen SC, Feldman SR, Lim HW, et al. American
Academy of Dermatology Consensus Conference on the safe and optimal use of
isotretinoin: summary and recommendations. J Am Acad Dermatol 2004;50:900-6.
For personal use only: See rights and reprints http://www.bmj.com/permissions
73
74
75
76
77
78
Jacobs DG, Deutsch NL, Brewer M. Suicide, depression, and isotretinoin: is there a causal
link? J Am Acad Dermatol 2001;45:S168-75.
Marqueling AL, Zane LT. Depression and suicidal behavior in acne patients treated with
isotretinoin: a systematic review. Semin Cutan Med Surg 2007;26:210-20.
Dunn LK, ONeill JL, Feldman SR. Acne in adolescents: quality of life, self-esteem, mood,
and psychological disorders. Dermatol Online J 2011;17:1.
Hahm BJ, Min SU, Yoon MY, Shin YW, Kim JS, Jung JY, et al. Changes of psychiatric
parameters and their relationships by oral isotretinoin in acne patients. J Dermatol
2009;36:255-61.
Committee on Comparative Effectiveness Research Prioritization, Institute of Medicine.
Initial national priorities for comparative effectiveness research. National Academies
Press, 2009. www.nap.edu/catalog.php?record_id=12648.
Fitz-Gibbon S, Tomida S, Chiu BH, Nguyen L, Du C, Liu M, et al. Propionibacterium acnes
strain populations in the human skin microbiome associated with acne. J Invest Dermatol
2013; published online 21 Jan.
Cite this as: BMJ 2013;346:f2634
BMJ Publishing Group Ltd 2013
Subscribe: http://www.bmj.com/subscribe
BMJ 2013;346:f2634 doi: 10.1136/bmj.f2634 (Published 8 May 2013)
Page 7 of 7
CLINICAL REVIEW
Table
Table 1| General treatment algorithm according to acne severity
Topical retinoid
Benzoyl peroxide
Topical
antibiotic
Oral antibiotic
Hormonal agent*
Maintenance
Recommended
treatment
Possible treatment
No
No
Possible treatment
No
No
Mild
Recommended
treatment
Possible treatment
No
No
No
Alternative
treatment
No
Mild-moderate
Recommended
treatment
Possible treatment
Recommended
treatment
No
No
Alternative
treatment
No
Moderate
Recommended
treatment
Recommended
treatment
Possible treatment
Alternative
treatment
Monotherapy
Moderate-severe
Recommended
treatment
Recommended
treatment
No
Recommended Possible treatment
treatment
Alternative
treatment
Monotherapy
No
No
No
No
Monotherapy
Severity
Severe
Recommended treatment
No
No
Azelaic acid
Oral retinoid
*Female patients only.
Oral retinoids are prescribed as monotherapy.
Select oral or topical antibiotic only.
For personal use only: See rights and reprints http://www.bmj.com/permissions
Subscribe: http://www.bmj.com/subscribe
You might also like
- 0610 - Peds Acne FeaDocument9 pages0610 - Peds Acne FeaReginaNo ratings yet
- Acne Vulgaris Pathogenesis, Treatment, and Needs AssessmentDocument8 pagesAcne Vulgaris Pathogenesis, Treatment, and Needs AssessmentOsler Rodríguez BarbaNo ratings yet
- Jurnal Acne 3Document6 pagesJurnal Acne 3riena456No ratings yet
- Acne Vulgaris PDFDocument8 pagesAcne Vulgaris PDFsmackooooooNo ratings yet
- Acne in Childhood Wendy Kim, Do and Anthony J. Mancini, MDDocument10 pagesAcne in Childhood Wendy Kim, Do and Anthony J. Mancini, MDPrajnamita Manindhya El FarahNo ratings yet
- Jurnal Acne 1Document12 pagesJurnal Acne 1riena456No ratings yet
- Acne Vulgaris ThesisDocument4 pagesAcne Vulgaris ThesisLisa Riley100% (1)
- Dermatology How To Manage Acne VulgarisDocument18 pagesDermatology How To Manage Acne VulgarisJosehNo ratings yet
- Perioral Dermatitis - StatPearls - NCBI BookshelfDocument5 pagesPerioral Dermatitis - StatPearls - NCBI BookshelfHanna ABNo ratings yet
- Acne Grading Guideline (Group 17)Document3 pagesAcne Grading Guideline (Group 17)Jennifer MartindocNo ratings yet
- Adult Female Acne: A Guide To Clinical Practice: EviewDocument14 pagesAdult Female Acne: A Guide To Clinical Practice: Eviewputri.SpANo ratings yet
- Acne Vulgaris DissertationDocument6 pagesAcne Vulgaris DissertationBestPaperWritingServiceUK100% (1)
- Pengģunaan ABDocument8 pagesPengģunaan ABPrashetyaQusnaNo ratings yet
- AcneDocument24 pagesAcnefarmasi_hm100% (2)
- Acne Vulgaris and Cosmetic 2016 jdv.13579Document10 pagesAcne Vulgaris and Cosmetic 2016 jdv.13579Vita BūdvytėNo ratings yet
- Diagnosis and Treatment of Acne: A Guide for Primary CareDocument17 pagesDiagnosis and Treatment of Acne: A Guide for Primary CareluthfiNo ratings yet
- Acne in Adolescents: BackgroundDocument4 pagesAcne in Adolescents: BackgroundMuthu RaajendhiraNo ratings yet
- Auriculotherpy in Treating Acne Rev 9112014Document72 pagesAuriculotherpy in Treating Acne Rev 9112014bertyNo ratings yet
- Diagnosis and Treatment of AcneDocument7 pagesDiagnosis and Treatment of AcnenovialbarNo ratings yet
- Hormonas and AcneDocument3 pagesHormonas and AcneRistiana Suci d'KemponNo ratings yet
- Case Discussion 5Document6 pagesCase Discussion 5Siraj INo ratings yet
- Jurding 1Document13 pagesJurding 1Hasmi YunitaNo ratings yet
- Pathophysiology and Impact of Acne Vulgaris (38 charactersDocument6 pagesPathophysiology and Impact of Acne Vulgaris (38 charactersPrajnamita Manindhya El FarahNo ratings yet
- Acne Vulgaris Management: What's New and What's Still True?: Review ArticleDocument5 pagesAcne Vulgaris Management: What's New and What's Still True?: Review ArticleAlmuizzu NurjannahNo ratings yet
- Acne treatments and preserving skin's barrier functionDocument4 pagesAcne treatments and preserving skin's barrier functionKataDullNo ratings yet
- Coretan SenimanDocument6 pagesCoretan SenimanerinNo ratings yet
- Acne Relapses Impact On Quality of Life and Productivity2019Document7 pagesAcne Relapses Impact On Quality of Life and Productivity2019sara3elena3manolacheNo ratings yet
- Practice Essentials AcneDocument6 pagesPractice Essentials AcneaigoooNo ratings yet
- Jurnal Kulit AcneDocument7 pagesJurnal Kulit AcnePsyhlaNo ratings yet
- Adolescent Acne Treatment Options OverviewDocument3 pagesAdolescent Acne Treatment Options OverviewMutiaraDaraNo ratings yet
- Adolescent Acne Treatment Options OverviewDocument3 pagesAdolescent Acne Treatment Options OverviewDesi RatnaningtyasNo ratings yet
- Acne Vulgaris Acne Vulgaris Acne Vulgaris Acne Vulgaris Acne VulgarisDocument8 pagesAcne Vulgaris Acne Vulgaris Acne Vulgaris Acne Vulgaris Acne VulgarisEga JayaNo ratings yet
- Acne Among Medical Students in Baghdad Pattern and Associated Factors 2761Document7 pagesAcne Among Medical Students in Baghdad Pattern and Associated Factors 2761fawzi aljassarNo ratings yet
- Meth Elab Topic N2Document19 pagesMeth Elab Topic N2Group M1869No ratings yet
- Literature Review On Acne VulgarisDocument8 pagesLiterature Review On Acne Vulgarisafmziepjegcfee100% (1)
- Mandelic Acid Chemical Peel in Acne Vulgaris: A Boon or A Bane?Document4 pagesMandelic Acid Chemical Peel in Acne Vulgaris: A Boon or A Bane?IOSRjournalNo ratings yet
- Current Issues in The Treatment of Acne VulgarisDocument8 pagesCurrent Issues in The Treatment of Acne VulgarisajiNo ratings yet
- The Relationship of Proper Skin Cleansing To Pathophysiology, Clinical Benefits, and The Concomitant Use of Prescription Topical Therapies in Patients With Acne VulgarisDocument13 pagesThe Relationship of Proper Skin Cleansing To Pathophysiology, Clinical Benefits, and The Concomitant Use of Prescription Topical Therapies in Patients With Acne VulgarisKadir KUCUKNo ratings yet
- Azaleic AcidDocument8 pagesAzaleic AcidRaissaOslinNo ratings yet
- Neglected aspects in the management of acneDocument5 pagesNeglected aspects in the management of acneaduranmexNo ratings yet
- ACNEDocument37 pagesACNE2226205No ratings yet
- SGD Ein 2 Kelompok 5Document27 pagesSGD Ein 2 Kelompok 5Rahmadanti Nur FadillaNo ratings yet
- Acad Dermatol Venereol - 2012 - Nast - European Evidence Based S3 Guidelines For The Treatment of AcneDocument29 pagesAcad Dermatol Venereol - 2012 - Nast - European Evidence Based S3 Guidelines For The Treatment of Acnesonrisa39No ratings yet
- European Guidelines Acne TreatmentDocument29 pagesEuropean Guidelines Acne TreatmentLeonardus LeonardusNo ratings yet
- BJD 19477Document19 pagesBJD 19477sagar6778No ratings yet
- Acne Therapeutic (Mandelic Acid)Document11 pagesAcne Therapeutic (Mandelic Acid)Nur NurkurniaNo ratings yet
- Jur DingDocument6 pagesJur DingRund Van EarghNo ratings yet
- An Update On The Diagnosis and Treatment of LeprosyDocument10 pagesAn Update On The Diagnosis and Treatment of LeprosyChlarissa WahabNo ratings yet
- Acne and Niacinamide 2017 dth.12481Document7 pagesAcne and Niacinamide 2017 dth.12481Vita BūdvytėNo ratings yet
- Candidiasis (Candidosis)Document17 pagesCandidiasis (Candidosis)h8j5fnyh7dNo ratings yet
- Microbiome and Probiotics in Acne Vulgaris-A Narrative ReviewDocument11 pagesMicrobiome and Probiotics in Acne Vulgaris-A Narrative ReviewVanNo ratings yet
- Synopsis PDFDocument11 pagesSynopsis PDFshivam tiwari100% (2)
- Diagnosis and Treatment of Rosacea: Aaron F. Cohen, MD, and Jeffrey D. Tiemstra, MDDocument4 pagesDiagnosis and Treatment of Rosacea: Aaron F. Cohen, MD, and Jeffrey D. Tiemstra, MDbookaholic7No ratings yet
- Chemical Peels and Microdermabrasion PDFDocument9 pagesChemical Peels and Microdermabrasion PDFKhiem Tran DuyNo ratings yet
- HERBAL PLANTS AND PROPIONIBACTERIUM ACNES - AN OVERVIEWDocument13 pagesHERBAL PLANTS AND PROPIONIBACTERIUM ACNES - AN OVERVIEWmskchoudhuriNo ratings yet
- Acne, The Skin Microbiome, and Antibiotic Treatment2019Document10 pagesAcne, The Skin Microbiome, and Antibiotic Treatment2019sara3elena3manolacheNo ratings yet
- Dermatology MCQ With AnswersDocument27 pagesDermatology MCQ With Answershesham0% (1)
- Atopic Dermatitis: New Perspectives on Managing a Chronic Inflammatory DiseaseFrom EverandAtopic Dermatitis: New Perspectives on Managing a Chronic Inflammatory DiseaseRating: 5 out of 5 stars5/5 (1)
- VitiligoFrom EverandVitiligoMauro PicardoNo ratings yet
- Fast Facts: Dermatological Nursing: A practical guide on career pathwaysFrom EverandFast Facts: Dermatological Nursing: A practical guide on career pathwaysNo ratings yet
- Skin Biopsy A Pillar in The Identification of Cutaneous Mycobacterium Tuberculosis Infection PDFDocument6 pagesSkin Biopsy A Pillar in The Identification of Cutaneous Mycobacterium Tuberculosis Infection PDFMeryam SetiawanNo ratings yet
- Skin Biopsy A Pillar in The Identification of Cutaneous Mycobacterium Tuberculosis Infection PDFDocument6 pagesSkin Biopsy A Pillar in The Identification of Cutaneous Mycobacterium Tuberculosis Infection PDFMeryam SetiawanNo ratings yet
- Cutaneous Tuberculosis in Children PDFDocument10 pagesCutaneous Tuberculosis in Children PDFMeryam SetiawanNo ratings yet
- Ref 8-BVDocument7 pagesRef 8-BVMeryam SetiawanNo ratings yet