Professional Documents
Culture Documents
Anatomy, Physiology & Pathogenesis of Appendicitis
Uploaded by
Hari SlzOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Anatomy, Physiology & Pathogenesis of Appendicitis
Uploaded by
Hari SlzCopyright:
Available Formats
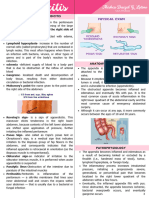
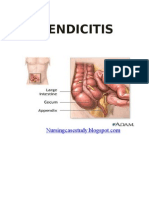
Anatomy of intestines, appendix, greater omentum, peritoneum and
abdominal wall.
Physiology of vomiting
Vomiting is the forceful ejection of stomach and intestinal content from the
mouth.
Can be caused by cerebral cause, visceral cause or altering in body chemistry.
1. Irritation of mucosal of upper GIT
2. Afferent nuclei from vestibular nuclei mediate nausea and vomiting of motion
sickness
3. Psychological sensory stimuli produce emetic response in vomiting centre
4. Chemoreceptor trigger zone in medulla detect changes in body pH.
5. Serotonin from enterochromaffin cells in small intestine trigger vomiting.
Before vomiting, nausea is felt. Stomach musculature is relaxed. Deep inspiration
takes place with closing of glottis and rising of soft palate. Sudden increase in
abdominal pressure brought by contraction of abdominal muscle. Violent
contraction of diaphragm and abdominal muscle compressing the stomach. This
forces gastric contents through relaxed stomach and oesophagus into mouth.
Physiology of peristalsis of intestine
Intestinal motility is controlled by peristalsis contraction, segmentation
contraction and tonic contraction. Peristalsis propels the chyme towards large
intestine. Segmentation contraction move the chyme to and fro, also increase its
exposure to the mucosal surface to facilitate digestion and absorption.
Ileum is linked to caecum by ileocaecal valve that restricts the reflux of colonic
content. Each time peristaltic wave reaches it, it open briefly, permitting some
chyme to squeeze into the caecum. When food leaves the stomach, the caecum
relaxes and passage of chyme across the ileocaecal valve increases, which is
known as gastroileal reflex.
Pathogenesis of appendicitis
Stages of appendicitis
1. Early stage- Obstruction of appendiceal lumen can be caused by lymphoid
hyperplasia, faecalith, foreign bodies, parasitic worm infection or inflammatory
stricture. Obstruction of appendix will cause fluid and mucus accumulation,
causing increased intraluminal pressure. This leads to bacterial growth within the
trapped mucous (as it is a good cultural environment) and appendiceal
distention. Acute inflammatory response occurs as the bacteria can produce
toxin and stimulate the aggregation of inflammatory cytokines. Inflammatory
response will cause oedema. Visceral nerve fibres are stimulated which patient
perceives as periumbilical pain, as the nerve that innervates the appendix and
umbilical dermatome is the same (T10).
2. Suppurative appendicitis- Increasing intraluminal pressure and oedema will
exceed the capillary perfusion pressure. The inflammatory response causing
swelling of lymph nodes which will further obstruct the lumen of appendix. This
results in more inflammatory fluid invasion and bacterial growth. Oedema and
venous congestion will cause the inflammatory response goes transmural, as
ischaemic condition starts to occur in the entire appendix. When the inflamed
serosa of appendix comes in contact with the parietal peritoneum, patient will
experience classic shift of pain from periumbilicus to the right lower abdominal
quadrant, which is continuous and more severe than early pain. This helps in
development of peritoneal irritation.
3. Gangrenous and perforated appendicitis- When the arterial blood flow
become fully compromised by the inflammation and oedema, this will lead to
tissue ischemia and gangrenous appendicitis. Persisting tissue ischaemia in
appendiceal infarction will cause full thickness necrosis of appendiceal wall,
resulting in perforation with release of faecal and suppurative content into
peritoneal cavity.
4. Abscess formation and peritonitis- The perforated appendix can be walled
off by adjacent greater omentum. A localised walled-off abscess occurs. If the
pathological condition rapidly advanced, perforation is free is peritoneal cavity
and generalised peritonitis can occur.
Pathophysiology of appendicitis
Nausea and vomiting is caused by intestinal obstruction and increased luminal
pressure. It is a protective mechanism to propel the obstructed material inside
intestine. Could be also caused by increased abdominal pressure due to swollen
appendix pressing the intestine. The condition worsen when the patient takes 5
hours journey to the hospital because the inflammation has developed to the
serious stage, and could be even worsened by motion sickness due to the road
condition.
Pain at periumbilical region is because of inflammation of appendix, which its
autonomic nerve is derived from the supply of T10. The pain is referred because
the periumbilical region is innervated by the same T10 level somatic sensory
nerve.
The second pain that shifted to the right iliac fossa is due to the inflammation of
the underlying parietal peritoneum beneath the skin. The peritoneum has its own
somatic innervation so the well localised pain is felt. The second pain is felt only
when the inflammation has gone transmural and eventually penetrates through
the serosal surface, causing inflammation on the overlying parietal peritoneum.
Tenderness (increased pain sensitivity) over right iliac fossa is due to swelling of
appendix pushes the parietal layer of peritoneum to abdominal wall, could be
also indicating the inflammation has been spread to peritoneum layer causing
peritonitis, thus increase its somatic pain sensitivity upon palpation.
Rebound tenderness is due to releasing of stretched parietal layer of peritoneum,
causing pain when the parietal peritoneum hit back on abdominal wall. It is an
indication of peritonitis.
Rigidity on abdomen upon arrival to hospital indicates that the peritonitis has
generalised over the lower part of abdomen. It is an involuntary response to
prevent pain caused by the pressure on abdomen.
*Initially after the appendix rupture, the greater omentum will adhere to the
perforated appendix to minimise the spread of inflammation to peritoneum,
causing tenderness and rebound tenderness at right iliac fossa at first. But after
some time, rigidity of abdomen is felt because the inflammation has diffusedly
spread around the lower abdomen (when inflammation, swelling of peritoneum
pushes it towards the abdomen wall causing pain), indicating generalised
peritonitis.
Lack of bowel sound is due to triggering of ileo-gastric reflex, impairing gastric
emptying process to reduce peristaltic activity of small bowel. This is to stop the
movement of chyme towards the small intestine to prevent further blockage.
Fibrinous material seen around the ileo-caecal region and right paracolic gutter is
due to inflammation triggering fibrosis.
Pharmacology of ampicillin, cloxacillin, metronidazole and cefuroxime
Ampicillin has activity against gram-positive, gram-negative and anaerobic
bacteria. It can interfere the bacterial cell wall synthesis during active replication.
Cloxacillin has similar target bacterial and similar function, but less susceptible to
beta-lactamase.
Cefuroxime is second generation cephalosporin, act against aerobic gram
positive and gram negative cocci and bacilli. Cefuroxime interfere bacterial cell
wall synthesis and is bactericidal.
Metronidazole is an antibiotic for anaerobes and antiprotozoal medication. It
inhibits nuclei acid synthesis by disrupting the DNA of microbial cells. This
function only happens when metronidazole is partially reduced and this reduction
can only happen in anaerobic cells.
Signs and symptoms of appendicitis
- Abdominal pain
- Nausea
- Vomiting
- Fever
- Migration of pain from abdominal wall to right lower quadrant of abdomen
- Sensitive to gentle touch on abdominal wall, pain felt upon application of
pressure
Rebound tenderness on abdominal wall, pain felt upon removal of pressure
Loss of appetite
Diarrhea or constipation
Some patients might have accessory signs such as
Rovsing sign (RLQ pain with palpation of the LLQ): Suggests peritoneal
irritation
Obturator sign (RLQ pain with internal and external rotation of the flexed
right hip): Suggests the inflamed appendix is located deep in the right
hemipelvis
Psoas sign (RLQ pain with extension of the right hip or with flexion of the
right hip against resistance): Suggests that an inflamed appendix is located
along the course of the right psoas muscle
Dunphy sign (sharp pain in the RLQ elicited by a voluntary cough): Suggests
localized peritonitis
RLQ pain in response to percussion of a remote quadrant of the abdomen or
to firm percussion of the patient's heel: Suggests peritoneal inflammation
Markle sign (pain elicited in a certain area of the abdomen when the
standing patient drops from standing on toes to the heels with a jarring
landing): Has a sensitivity of 74%
Causes
Caused by primary obstruction of lumen of appendix. When obstruction occurs,
appendix filled with mucous and swells. This creates a good environment for
bacterial growth. Colonisation of bacteria causes inflammation. Continued
production of mucous and inflammation leads to increased pressure within the
lumen and walls of appendix. Swelling and oedema of appendix will cause
thrombosis and occlusion of small vessels and stasis of lymphatic flow. When
there is occlusion of blood vessels, appendix will progress to ischaemic condition
and necrosis occurs. Bacteria will leak out from dying walls, forming pus around
and within the appendix. This will result in appendiceal rupture causing
peritonitis.
The causative agents of obstruction including bezoar (a mass trapped in GI tract
eg. Food bolus), foreign bodies, trauma, intestinal worms, lymphadenitis and
calcified faecal deposits (faecaliths).
Obstruction in appendix is thought to be contributed by faecal retention in colon
and prolonged transit time. Calcium salts and faecal debris will form layered
material around appendix, forming faecaliths.
Obstruction in GI tract particularly appendix can cause bacterial growth and
infection. These infections can further causing swelling and inflammation of
lymph vessels (lymphangitis) and lymph nodes (lymphadenitis). Swelling of
lymph node can further worsen the obstruction of appendix.
Diagnosis
- Complete blood count. Neutrophilia and leucocytosis is seen most patient of
appendicitis. But the blood test is not specific.
- C-reactive protein count. High CRP especially in patient progressing to
gangrene stage of appendicitis. But CRP count is not specific and does not
distinguish between infection and inflammation.
- Urinalysis. Some patients may have dysuria or right flank pain. Some patients
might have blood or pus in the urine. Can be used to differentiating appendicitis
from UTI.
- Urinary 5-HIAA. Its measurement could be an early marker of appendicitis.
- CT scan, MRI and ultrasound. Used for confirmation of appendicitis. CT scan not
recommended for children because of its radiation exposure.
- Kidneys-ureters-bladder radiographs. For visualisation of appendicoliths in
patient associated with appendicitis.
- Barium enema study. Absent or incomplete filling of appendix coupled with
pressure effect (due to obstruction) suggests appendicitis.
Treatment and management
- Appendectomy is the only curative treatment of appendicitis.
- Antibiotics prophylaxis should be administered before appendectomy to prevent
septicaemia. Patients with suspected appendicitis should not be given anything
by mouth, this could increase the obstruction.
- Preoperative antibiotics have efficacy in decreasing postoperative wound
infection rates.
- Broad-spectrum antibiotics for aerobic and anaerobic microorganism coverage.
Complications
- Wound infection or dehiscence after surgery
- Bowel obstruction
- Abdominal or pelvic abscess
- Sepsis
- Complicated peritonitis
Prognosis
Good prognosis. But delayed diagnosis and treatment can cause mortality and
morbidity associated with appendicitis. Overall mortality rate is around 0.2 to
0.8% attributable complications of disease rather than surgery. Perforation and
gangrenous appendicitis can cause higher morbidity rate.
Risk factors
Refer to cause
Preventions
It is not possible to prevent appendicitis.
Epidemiology
Many people sakit perut.
You might also like
- Acute Abdomen - SabistonDocument24 pagesAcute Abdomen - Sabiston2013SecB100% (1)
- Nursing InterventionsDocument3 pagesNursing InterventionsJemiah Lyn C. BragadoNo ratings yet
- Rif PainDocument26 pagesRif PainShashank SoodNo ratings yet
- Inflammatory Disorders AppendecitisDocument28 pagesInflammatory Disorders Appendecitisfrozen loombandsNo ratings yet
- Acute Appendicitis Signs, Causes, and TreatmentDocument4 pagesAcute Appendicitis Signs, Causes, and TreatmentSukainah syifahNo ratings yet
- Inflammatory Disorders AppendecitisDocument17 pagesInflammatory Disorders Appendecitisfrozen loombandsNo ratings yet
- AppendicitisDocument23 pagesAppendicitisGina LositoNo ratings yet
- Appendicitis DR WellDocument17 pagesAppendicitis DR Wellk.adeputriNo ratings yet
- Case Study AppendicitisDocument6 pagesCase Study AppendicitisPrincess Camille ArceoNo ratings yet
- Care of Clients WithDocument7 pagesCare of Clients Withyn8jg9fwx6No ratings yet
- AppendicitisDocument25 pagesAppendicitissjamilmdfauzie100% (1)
- Appendicitis (History & Examination)Document6 pagesAppendicitis (History & Examination)Doctor Saleem Rehman75% (4)
- Appendicitis Case StudyDocument30 pagesAppendicitis Case StudyAj GoNo ratings yet
- Grabe Ka FinalDocument57 pagesGrabe Ka FinalJoanne Bernadette AguilarNo ratings yet
- Nursing Care for Appendicitis PatientsDocument22 pagesNursing Care for Appendicitis PatientsIta Puspita Sari100% (1)
- Pathophysiology of AppendicitisDocument2 pagesPathophysiology of Appendicitis33342No ratings yet
- Ii. Appendicitis 1Document3 pagesIi. Appendicitis 1lalisa manobanNo ratings yet
- Appendectomy Appendicitis Case Study1Document18 pagesAppendectomy Appendicitis Case Study1Los Devio100% (1)
- Appendicitis Is A Condition Characterized by Inflammation of The Appendix. It Is Classified As A MedicalDocument5 pagesAppendicitis Is A Condition Characterized by Inflammation of The Appendix. It Is Classified As A Medicalbhe_jewelNo ratings yet
- Anatomy and Physiology of Git System (Gastroinstestinal Tract)Document37 pagesAnatomy and Physiology of Git System (Gastroinstestinal Tract)Nishi RuciNo ratings yet
- Pathophysiology AppendicitisDocument3 pagesPathophysiology AppendicitisIra Krystel ReyesNo ratings yet
- Answers For Oral FinalDocument139 pagesAnswers For Oral FinalIris BakerNo ratings yet
- Positioning of The Patient For Abdominal ExaminationDocument8 pagesPositioning of The Patient For Abdominal ExaminationDoctor Saleem RehmanNo ratings yet
- MS GI AppendicitisDocument2 pagesMS GI AppendicitisRachelle Ann CarilloNo ratings yet
- Pathophysiology: AppendicitisDocument3 pagesPathophysiology: AppendicitisEqah TajuddinNo ratings yet
- Gastrointestinal SystemDocument5 pagesGastrointestinal SystemTaylor NicholNo ratings yet
- Acute Appendicitis Signs, Symptoms, and TreatmentDocument39 pagesAcute Appendicitis Signs, Symptoms, and TreatmentVishva Lalitbhai HirparaNo ratings yet
- AppendicitisDocument4 pagesAppendicitisRonaldoNo ratings yet
- Acute Appendicitis Pathophysiology: MycobacteriaDocument10 pagesAcute Appendicitis Pathophysiology: MycobacteriaUzma KhanNo ratings yet
- Acute Abdominal Pain GuideDocument16 pagesAcute Abdominal Pain Guidereina200305No ratings yet
- Khim2 AppendicitisDocument2 pagesKhim2 AppendicitisMae Ann DiolataNo ratings yet
- Acute Appendicitis in Adults - Clinical Manifestations and Differential DiagnosisDocument17 pagesAcute Appendicitis in Adults - Clinical Manifestations and Differential Diagnosisnicholas Rojas SIlvaNo ratings yet
- AppendicitisDocument17 pagesAppendicitisAhmed Halaby100% (1)
- JJGR v1 1004Document5 pagesJJGR v1 1004laurencia aliminNo ratings yet
- لقطة شاشة 2022-04-21 في 11.10.40 صDocument55 pagesلقطة شاشة 2022-04-21 في 11.10.40 صEngi KazangyNo ratings yet
- Acute AppendicitisDocument9 pagesAcute AppendicitisSyarafina AzmanNo ratings yet
- APPENDICITISDocument37 pagesAPPENDICITISjohn paul richard mindanaoNo ratings yet
- Acute AppendicitisDocument15 pagesAcute AppendicitisSetyawan Aditya Pambudi SNo ratings yet
- Tanda dan Komplikasi Perforasi Usus pada Demam TifoidDocument5 pagesTanda dan Komplikasi Perforasi Usus pada Demam TifoidSisca Dwi Agustina0% (1)
- Pathophysiology of AppendicitisDocument2 pagesPathophysiology of AppendicitisAbbie Tantengco100% (3)
- Peritonitis: MselemaDocument64 pagesPeritonitis: MselemaAugustus CaesarNo ratings yet
- Acute Appendicitis: Causes, Symptoms and TreatmentDocument46 pagesAcute Appendicitis: Causes, Symptoms and TreatmentRAJAT DUGGALNo ratings yet
- Case Presentation On AppendecitisDocument68 pagesCase Presentation On AppendecitisJah GatanNo ratings yet
- Adult 1 Appendicitis and Peritonitis Guide for NursesDocument6 pagesAdult 1 Appendicitis and Peritonitis Guide for NursesSamah AdnanNo ratings yet
- Abdominal Pain: DR Budi Enoch SPPDDocument22 pagesAbdominal Pain: DR Budi Enoch SPPDRoby KieranNo ratings yet
- Differential Diagnosis Pain Right HypochondriumDocument35 pagesDifferential Diagnosis Pain Right HypochondriumDrArish Mahmood100% (1)
- Peptic Ulcer Symptoms, Causes and TreatmentsDocument14 pagesPeptic Ulcer Symptoms, Causes and Treatmentslagas_ralphNo ratings yet
- Acute AppendicitisDocument40 pagesAcute AppendicitisShegzy Michael SolankeNo ratings yet
- Chapter 2. Differential Diagnosis and Treatment of Gastric Dyspepsia SyndromeDocument9 pagesChapter 2. Differential Diagnosis and Treatment of Gastric Dyspepsia SyndromeShravan SharmaNo ratings yet
- Appendix Part 1Document8 pagesAppendix Part 1Abdullah EssaNo ratings yet
- Abdominal Pain Dept. of MedicineDocument37 pagesAbdominal Pain Dept. of Medicineiftekhar islamNo ratings yet
- Acute Appendicitis in Adults Clinical Ma PDFDocument27 pagesAcute Appendicitis in Adults Clinical Ma PDFAntonio Zumaque CarrascalNo ratings yet
- PERITONITSDocument3 pagesPERITONITSjyoti kundu100% (1)
- Appendicitis - PeritonitisDocument37 pagesAppendicitis - PeritonitisanisamayaNo ratings yet
- Acute Abdomen and Intestinal Obstruction CausesDocument116 pagesAcute Abdomen and Intestinal Obstruction CausesFan EliNo ratings yet
- Case Study AppendectomyDocument39 pagesCase Study AppendectomyHomework Ping100% (1)
- Causes and Types of Abdominal Pain ExplainedDocument14 pagesCauses and Types of Abdominal Pain ExplainedmdjohariNo ratings yet
- Chapter 14. Abdominal PainDocument10 pagesChapter 14. Abdominal PaindekergnpNo ratings yet
- Diverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesFrom EverandDiverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesRating: 1 out of 5 stars1/5 (1)
- Neonatal SepsisDocument3 pagesNeonatal SepsisHari SlzNo ratings yet
- Short Success StoryDocument1 pageShort Success StoryHari SlzNo ratings yet
- Lets Clear This Doubt For The Essay Question Once and For AllDocument1 pageLets Clear This Doubt For The Essay Question Once and For AllHari SlzNo ratings yet
- Tornadocluster To HeadDocument5 pagesTornadocluster To HeadHari SlzNo ratings yet
- Heron Kerja Projek AM SPM 2013Document38 pagesHeron Kerja Projek AM SPM 2013Hari SlzNo ratings yet
- Higher Order Thinking SkilsDocument2 pagesHigher Order Thinking SkilsHari SlzNo ratings yet
- The Novel That I Have Learnt in Form Five IsDocument1 pageThe Novel That I Have Learnt in Form Five IsHari SlzNo ratings yet
- Mind Map Eng 1Document1 pageMind Map Eng 1Hari SlzNo ratings yet
- Mind Map Eng 1Document1 pageMind Map Eng 1Hari SlzNo ratings yet
- One Student One Sport - Sheikh Kamaruddin 01Document10 pagesOne Student One Sport - Sheikh Kamaruddin 01Zd ZaidiNo ratings yet
- English Book Revie1Document10 pagesEnglish Book Revie1Hari SlzNo ratings yet
- Global WarmingDocument2 pagesGlobal WarmingHari SlzNo ratings yet
- ArticlesDocument4 pagesArticlesHari SlzNo ratings yet
- Medical CertificateDocument126 pagesMedical CertificateAnonymous mummYD0% (1)
- Medical Reabursement GONo.74Document19 pagesMedical Reabursement GONo.74gsreddy100% (1)
- Understanding Anemia: Causes, Symptoms, Diagnosis and TreatmentDocument27 pagesUnderstanding Anemia: Causes, Symptoms, Diagnosis and Treatment1108010091No ratings yet
- Emerging and Re Emerging DiseasesDocument63 pagesEmerging and Re Emerging DiseasesAljun MansalapusNo ratings yet
- Diploma in DiabetologyDocument8 pagesDiploma in Diabetologydawood260No ratings yet
- Colorectal Cancer Case StudyDocument1 pageColorectal Cancer Case StudyNur'aini Elita PutriNo ratings yet
- Anemia in Pregnancy by MahreeDocument53 pagesAnemia in Pregnancy by MahreesherzadmahreeNo ratings yet
- Hypertension - Management in Pregnancy Guideline (GL952) : ApprovalDocument55 pagesHypertension - Management in Pregnancy Guideline (GL952) : ApprovalhestiNo ratings yet
- Scripta Medica 46 2 English PDFDocument62 pagesScripta Medica 46 2 English PDFSinisa RisticNo ratings yet
- Alcoholic Gastritis Case PresentationDocument18 pagesAlcoholic Gastritis Case Presentationstancy thomas100% (1)
- Product Name:: Alaris™ GS, GH, CC, TIVA, PK, Enteral Syringe PumpDocument14 pagesProduct Name:: Alaris™ GS, GH, CC, TIVA, PK, Enteral Syringe PumpSalim AloneNo ratings yet
- Pregnancy Complications in Woman with Sickle Cell AnemiaDocument3 pagesPregnancy Complications in Woman with Sickle Cell AnemiaJam AliNo ratings yet
- Certificate of DeathDocument2 pagesCertificate of DeathAlfie Omega100% (2)
- Arterial Blood GasDocument55 pagesArterial Blood GasRathis Dasan100% (1)
- Panic DisorderDocument14 pagesPanic DisorderMatthew MckenzieNo ratings yet
- Board Exam Compilation Book 1Document141 pagesBoard Exam Compilation Book 1Aaron Cy Untalan75% (8)
- Medical Surgical Nursing Practice Test Part 1Document15 pagesMedical Surgical Nursing Practice Test Part 1cleznielNo ratings yet
- A Comparative Study of Hyfrecator Ablation To That of Cryosurgery in The Management of Benign Skin GrowthsDocument5 pagesA Comparative Study of Hyfrecator Ablation To That of Cryosurgery in The Management of Benign Skin GrowthsinventionjournalsNo ratings yet
- FAQs - NBME Comprehensive Clinical Science Self-Assessments - Updated July 28, 2021Document3 pagesFAQs - NBME Comprehensive Clinical Science Self-Assessments - Updated July 28, 2021羅瑞恩No ratings yet
- Stok 9 Jun 22Document90 pagesStok 9 Jun 22Sutama ArimbawaNo ratings yet
- КРАТКИЙ КУРС ПАТОМОРФОЛОГИИ ЧАСТЬ 1 ENGDocument214 pagesКРАТКИЙ КУРС ПАТОМОРФОЛОГИИ ЧАСТЬ 1 ENGRishik RanaNo ratings yet
- Biostatistics For CK Step 2 6.16.2019Document37 pagesBiostatistics For CK Step 2 6.16.2019karan kauraNo ratings yet
- Dermatitis HerpetiformisDocument4 pagesDermatitis HerpetiformisRizky ArfinaNo ratings yet
- Our Lady of Fatima University College of Nursing - Cabanatuan CityDocument3 pagesOur Lady of Fatima University College of Nursing - Cabanatuan CityDanica FrancoNo ratings yet
- Bag-Mask Ventillation PDFDocument6 pagesBag-Mask Ventillation PDFHaris PapadopoulosNo ratings yet
- Efektifitas Latihan Progressive Muscle Relaxation (PMR) Terhadap Mual Muntah Kemoterapi Pasien Kanker OvariumDocument8 pagesEfektifitas Latihan Progressive Muscle Relaxation (PMR) Terhadap Mual Muntah Kemoterapi Pasien Kanker OvariumMutmin AnsariNo ratings yet
- Drug Name Mechanism of Action Indication Contraindication Side Effects Nursing Responsibility Generic NameDocument4 pagesDrug Name Mechanism of Action Indication Contraindication Side Effects Nursing Responsibility Generic NameDan HizonNo ratings yet
- References: Bibliography Text BooksDocument14 pagesReferences: Bibliography Text Bookskalla sharonNo ratings yet
- Grade 6 WHLP 5Document14 pagesGrade 6 WHLP 5Benj AlejoNo ratings yet
- Laser Courses, Laser ClassesDocument15 pagesLaser Courses, Laser Classessiya rajNo ratings yet