Professional Documents
Culture Documents
Blood-Borne Infections Guide
Uploaded by
Rhod Bernaldez EstaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Blood-Borne Infections Guide
Uploaded by
Rhod Bernaldez EstaCopyright:
Available Formats
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
I. SEPSIS IN CHILDREN
Systemic Inflammatory Response Syndrome (SIRS)
The presence of two or more of the following four criteria, one of which must be
abnormal temperature or white blood cell count:
1. Core temperature (rectal, bladder, oral, or central catheter probe) >38.5°C
(101.3°F) or <36°C (96.8°F)
2. Tachycardia or bradycardia
3. Mean RR >2 standard deviations for age or mechanical ventilation for an
acute process not related to an underlying neuromuscular disease or to
general anesthesia
4. Abnormal WBC count or >10% immature neutrophils
Sepsis: SIRS in the presence of or caused by suspected or proven infection
A. Neonate
POTENTIALLY SEPTIC NEONATE
Etiology: Asymptomatic neonates with documented maternal risk factors like
history of UTI during the last trimester, membranes ruptured >18h before delivery,
fever >38°C before delivery or during labor and/or foul-smelling or purulent
amniotic fluid
Preferred Regimen:
Ampicillin PLUS Gentamicin or Amikacin
Weight, Age Ampicillin Gentamicin Amikacin
≤2 kg, ≤7d old: 50mg/kg q12h 5mg/kg q48h 15mg/kg q48h
≤2 kg, 8-28d old: 50mg/kg q8h 5mg/kg q36h 15mg/kg q24h
>2kg, ≤7d old: 50mg/kg q8h 4mg/kg q24h 15mg/kg q24h
>2kg, 8-28d old: 50mg/kg q6h 4-5mg/kg q24h 17.5mg/kg q24h
Comments:
For infants who remain asymptomatic and whose initial blood cultures are
negative after 48-72 hours of incubation, antimicrobial therapy can be
discontinued. If no pathogen has been isolated but bacterial sepsis cannot be
excluded, a negative CRP test at 72 hours can help support decision to discontinue
antibiotics.
NEONATAL SEPSIS
Etiology: Gram-negative bacilli, Group B streptococci, S. pneumoniae, S. aureus
National Antibiotic Guidelines 1
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Neonates with bacterial sepsis may present either with non-specific signs and
symptoms or focal signs of infection. The clinical criteria for the diagnosis of
bacterial sepsis by the Integrated Management of Childhood Illness (IMCI) and
WHO are as follows:
NEUROLOGIC: convulsions, drowsy or unconscious, decreased activity,
bulging fontanel
RESPIRATORY: respiratory rate >60 breaths/min, grunting, sever chest
indrawing, central cyanosis
CARDIAC: poor perfusion, rapid and weak pulse
GASTROINTESTINAL: jaundice, poor feeding, abdominal distention
DERMATOLOGIC: skin pustules, periumbilical erythema or purulence
MUSCULOSKELETAL: edema or erythema overlying bones or joints
OTHER: Temperature >37.7°C (99.9°F; or feels hot) or <35.5°C
(95.9°F; or feels cold)
Preferred Regimen:
1st line: 2nd line:
Cefotaxime Ceftazidime
≤2 kg, ≤7d old: 50mg/kg q12h ≤2 kg, ≤7d old: 50mg/kg q12h
≤2 kg, 8-28d old: 50mg/kg q8-12h ≤2 kg, 8-28d old: 50mg/kg q8-12h
>2kg, ≤7d old: 50mg/kg q12h >2kg, ≤7d old: 50mg/kg q12h
>2kg, 8-28d old: 50mg/kg q8h or >2kg, 8-28d old: 50mg/kg q8h
Ceftriaxone 50mg/kg q24h PLUS
PLUS Gentamicin
Gentamicin ≤2 kg, ≤7d old: 5mg/kg q48h
≤2 kg, ≤7d old: 5mg/kg q48h ≤2 kg, 8-28d old: 5mg/kg q36h
≤2 kg, 8-28d old: 5mg/kg q36h >2kg, ≤7d old: 4mg/kg q24h
>2kg, ≤7d old: 4mg/kg q24h >2kg, 8-28d old: 4-5mg/kg q24h or
>2kg, 8-28d old: 4-5mg/kg q24h or Amikacin
Amikacin ≤2 kg, ≤7d old: 15mg/kg q48h
≤2 kg, ≤7d old: 15 mg/kg q48h ≤2 kg, 8-28d old: 15mg/kg q24h
≤2 kg, 8-28d old: 15mg/kg q24h >2kg, ≤7d old: 15mg/kg q24h
>2kg, ≤7d old: 15mg/kg q24h >2kg, 8-28d old: 17.5mg/kg q24h
>2kg, 8-28d old: 17.5mg/kg q24h
WITH OR WITHOUT
Oxacillin
≤2 kg, ≤7d old: 25mg/kg q12h
≤2 kg, 8-28d old: 50mg/kg q8h
>2kg, ≤7d old: 50mg/kg q8h
>2kg, 8-28d old: 50mg/kg q6h or
Vancomycin (for MRSA)
Meningitis: 15mg/kg/dose
Bacteremia: 10mg/kg/dose
2 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Dosing Interval chart
Gestational Postnatal Interval
Age(weeks) (days) (hours)
≤29 0-14 18
>14 12
30 to 36 0-14 12
>14 8
37 to 44 0 to 7 12
>7 8
≥45 ALL 6
DOT: 7-10d or approximately 5-7d after clinical signs and symptoms of infection
have disappeared
Comments:
Precautions for ceftriaxone: Because of its extensive protein binding, ceftriaxone
can displace bilirubin from albumin-binding sites, with the potential risk of
inducing kernicterus. Thus, its use should be avoided in jaundiced neonates.
Likewise, neonates should not receive ceftriaxone intravenously if also receiving
intravenous calcium in any form, including parenteral nutrition, because of the risk
for precipitation of ceftriaxone-calcium salt.
Add Oxacillin or Vancomycin (MRSA) if with skin/soft tissue infections (refer to
the Skin and Soft Tissue Infections guidelines). Use Ceftazidime if Pseudomonas or
Burkholderia is suspected.
B. Child, Immunocompetent
CLINICAL SEPSIS WITHOUT FOCUS
Etiology: Preferred Regimen:
S. pneumoniae, Ceftriaxone 100mg/kg/d IV q12-24h (Max: 2-4 g/d) or
S. aureus (MSSA & Cefotaxime 200-225mg/kg/d q4-6h (Max: 8-12g/d)
MRSA), WITH OR WITHOUT
H. influenzae B, Oxacillin 150-200mg/kg/d q4-6h (Max: 4-12 g) or
Meningococci Vancomycin 40-60mg/kg/d q6h (for MRSA) (Max: 2-4g/d)
DOT: 10-14d or longer depending on established foci of infection
Comments:
Check on immunization status against Pneumococcus and H. influenzae B. Provide
coverage for S. aureus if with concomitant skin/soft tissue infections or previous
trauma. May use oxacillin only if culture-proven sensitive.
National Antibiotic Guidelines 3
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
URINARY SOURCE (SEE UTI, COMPLICATED)
Etiology: Preferred Regimen:
Enterobacteriaceae, Ceftriaxone 100mg/kg/d IV q12-24h (Max: 2-4g/d) or
P. aeruginosa, Cefotaxime 200-225 g/kg/d q4-6h (Max: 8-12g/d)
Enterococcus PLUS
Gentamicin 6-7.5mg/kg/d q8h or 5-7.5mg/kg/d qd or
Amikacin 15-22.5mg/kg/d q8-12h or 15-20mg/kg/d qd
DOT: 10-14d or longer depending on established foci of infection
INTRA-ABDOMINAL SOURCE
Etiology: Enterobacteriaceae, Bacteroides sp, Enterococci, P. aeruginosa
Preferred Regimen:
1st line: 2nd line:
Ampicillin 200-400mg/kg/d IV q8h Ampicillin-sulbactam 200 mg/kg/d
(Max: 6-12 g/d) q6h (ampicillin component) (Max: 8
PLUS g/d) or
Gentamicin 6-7.5mg/kg/d q8h or Piperacillin-tazobactam 300mg
5-7.5 mg/kg/d qd or (piperacillin component) (Max: 9-
Amikacin 15-22.5mg/kg/d q8-12h or 16g/d)
15-20 mg/kg/d qd WITH OR WITHOUT
PLUS Gentamicin 6-7.5mg/kg/d q8h or
Metronidazole 30-50mg/kg/d q6h 5-7.5mg/kg/d qd or
(Max: 1.5g/d) or Amikacin 15-22.5mg/kg/d q8-12h or
Clindamycin 20-40mg/kg/d IV q6-8h 15-20 mg/kg/d qd or
(Max: 1.8-2.7g/d) Ceftriaxone 100mg/kg/d IV q12-24h
(Max: 2-4 g/d) or
Cefotaxime 200-225mg/kg/d q4-6h
(Max: 8-12g/d)
PLUS
Metronidazole 30-50mg/kg/d q8h
(Max: 1.5g/d) or
Clindamycin 20-40 mg/kg/d IV q6-8h
(Max: 1.8-2.7 g/d)
DOT: 10-14d or longer depending on established foci of infection
POST-SPLENECTOMY/ FUNCTIONAL ASPLENIA
Etiology: Preferred Regimen:
S. pneumoniae, Ceftriaxone 100mg/kg/d IV q12-24h (Max: 2-4 g/d)
H. influenzae, OR
4 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
N. meningitides Cefotaxime 200-225mg/kg/d q4-6h (Max: 8-12g/d)
HEALTHCARE-ASSOCIATED SEPSIS
Etiology: Gram-negative bacilli, S. aureus
Preferred Regimen:
Ceftazidime 150-200mg/kg/d q8h (Max: 6 g/d) or
Cefepime 100-150mg/kg/d q8h (Max: 4-6g/d) or
Piperacillin-tazobactam 300mg/kg/d q8h (piperacillin component) (Max: 9-16
g/d) or Meropenem 60-120mg/kg/d q8h (Max: 1.5-6g/d)
WITH OR WITHOUT
Amikacin 15-22.5mg/kg/d q8-12h or 15-20mg/kg/d qd
WITH OR WITHOUT
Vancomycin 40-60mg/kg/d q6h (Max: 2-4 g/d)
Comments:
Choice of empiric antibiotic therapy should be based on current antimicrobial
susceptibility pattern within an institution. For severe infections with
Pseudomonas and/or if antimicrobial resistance is suspected add aminoglycosides.
If with previous surgery, IV therapy or other instrumentation and staphylococcal
infection is suspected.
SEVERE SEPSIS AND SEPTIC SHOCK
Severe Sepsis: Sepsis plus one of the following: cardiovascular organ dysfunction,
acute respiratory distress syndrome or two or more other instances of organ
dysfunction as defined in the consensus statement
Septic Shock: Sepsis and cardiovascular organ dysfunction
Preferred Regimen:
Piperacillin-tazobactam 300mg/kg/d q8h (piperacillin component) (Max: 9-
16g/d) or Meropenem 60-120mg/kg/d q8h (Max: 1.5-6g/d) PLUS
Vancomycin
Neonates* Child
Meningitis: 15mg/kg/dose 40-60 mg/kg/d q6h
Bacteremia: 10mg/kg/dose (Max dose: 2-4 g/d)
*See previous Dosing Interval Chart in Neonatal Sepsis
DOT: 10-14d in the absence of a complication
Comments:
The initial assessment and treatment of the pediatric shock patient should include
stabilization of airway, breathing, and circulation (the ABC’s) plus early
National Antibiotic Guidelines 5
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
administration of broad spectrum antibiotics. The choice of antimicrobial agents
depends on the predisposing risk factors, clinical situation, and the antibiotic
resistance patterns in the community and/or hospital settings. Modify antibiotic
regimen based on culture and sensitivity.
STAPHYLOCOCCAL TOXIC SHOCK SYNDROME
Clinical Findings:
Fever: Temperature ≥38.9°C (102°F)
Rash: Diffuse macular erythroderma
Desquamation: 1-2 weeks after onset of illness, on palms, soles, fingers, and toes
Hypotension
Involvement of ≥3 of the following organ systems:
• GIT: Vomiting or diarrhea at onset of illness
• Muscular: Severe myalgia or creatinine phosphokinase > 2x twice the upper
limit of normal
• Mucous membrane: Vaginal, oropharyngeal, or conjunctival hyperemia
• Renal: BUN or serum creatinine > 2x upper limit of normal or ≥5 wbc/hpf in
the absence of UTI
• Hepatic: Total bilirubin, AST, or ALT > 2x upper limit of normal for the
laboratory
• Hematologic: platelets <100,000/mm3
• CNS: disorientation or alterations in consciousness without focal neurologic
signs when fever and hypotension are absent
Negative results on the following tests, if obtained: Blood, throat, or cerebrospinal
fluid cultures (blood culture may be positive for S. aureus, Serologic tests for Rocky
Mountain spotted fever, leptospirosis, or measles)
Case Classification
Probable: A case with 5 of the 6 clinical findings as above
Confirmed: A case with all 6 of the clinical findings as above, including
desquamation, unless the patient dies before desquamation could occur
Preferred Regimen:
Oxacillin 150-200mg/kg/d IV q4-6h (Max: 4-12g/d) or
Cefazolin 75-100mg/kg/d IV q8h (Max: 3-6g/d) or
Vancomycin (for MRSA): 40-60 mg/kg/d IV q6h drip x 1h (Max: 2-4 g/d)
PLUS Clindamycin 30-40mg/kg/d IV q6-8h (Max: 1.8-2.7 g/d)
PLUS IVIG 150-400mg/kg x 5d or 1 dose of 1-2 g/kg
DOT: 10-14d in the absence of a complication
Comments:
Immediate aggressive fluid management; surgical debridement; anticipatory
management of multisystem organ failure. Intravenous immunoglobulin (IVIG) can
6 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
be considered in severe staphylococcal TSS unresponsive to other therapeutic
measures.
STREPTOCOCCAL TOXIC SHOCK SYNDROME
Clinical Criteria: Hypotension plus 2 or more of the following: renal impairment,
coagulopathy, hepatic involvement, adult respiratory distress syndrome,
generalized erythematous macular rash, and soft-tissue necrosis
Definite Case: Clinical criteria plus Group A streptococcus from a normally sterile
site
Probable Case: Clinical criteria plus Group A streptococcus from a nonsterile site
Preferred Regimen:
Penicillin G Na 200,000-300,000 U/kg/d IV q4-6h (Max: 12-24 MU/d) OR
Ceftriaxone 100mg/kg/d q12-24h (Max: 2-4 g/d)
PLUS Clindamycin 30-40mg/kg/d IV q6-8h (Max: 1.8-2.7 g/d)
PLUS IVIG 1g/kg on d1, followed by 0.5 g/kg on d2-3
DOT: 10-14d or longer depending on established foci of infection
Comments:
Immediate aggressive fluid management. Surgical debridement. Anticipatory
management of multisystem organ failure. Intravenous immunoglobulin (IVIG)
may be considered if refractory to several hours of aggressive therapy or in the
presence of undrainable focus or persistent oliguria with pulmonary edema.
Febrile Neutropenia in Children
Neutropenia is defined as an ANC of < 500 cells/mm3 or an ANC that is expected
to decrease to <500 cells/mm3 during the next 48h.
Etiology: Staph including MRSA, Streptococcus, Enterococci, P. aeruginosa and
other gram-negative bacilli, Fungi
Preferred Regimen:
Cefepime 150mg/kg/d div q8h or Piperacillin-tazobactam 300mg/kg/d div q6h or
Meropenem 60-120mg/kg/d div q8h (Max: 2-4g)
If antimicrobial resistant pathogens are suspected consider adding Amikacin 15-
20mg/kg/d qd. In cases of suspected catheter-related infection, or skin or soft-
tissue infection, pneumonia, or hemodynamic instability consider adding
Vancomycin 40-60mg/kg/d q6h (Max: 2-4g/day)
If with abdominal symptoms (pain or blood per rectum) or suspected C. difficile
infection consider adding Metronidazole IV: 22.5-40mg/kg/d q8h (Max: 1.5 g/d);
PO: 30-50mg/kg/d q8h (Max: 2.25 g/d).
National Antibiotic Guidelines 7
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Empirical antifungal coverage should be considered in high-risk patients who have
persistent fever after 4–7 days of a broad-spectrum antibacterial regimen and no
identified fever source. Treatment is continued until patient is afebrile and ANC
>500 cells/μl.
Comments:
Start empiric antibiotics as soon as possible after taking blood cultures and refer
to an ID specialist. Baseline laboratory tests to request for are:
• (CBC) count with differential leukocyte count and platelet count
• creatinine and BUN
• electrolytes
• hepatic transaminase enzymes
• bilirubin
• blood cultures, at least 2 sets of which are recommended, with a set
collected simultaneously from each lumen of an existing central venous
catheter (CVC), if present, and from a peripheral vein site; 2 blood culture
sets from separate venipunctures should be sent if no central catheter is
present.
• Culture of specimens from other sites of suspected infection should be
obtained as clinically indicated
• CXR for patients with respiratory signs and symptoms
GCSFs are not routinely recommended
II. SEPSIS IN ADULTS
Sepsis is defined as presence of suspected or documented infection associated
with life threatening organ dysfunction represented by a quick SOFA (Sequential
Organ Failure Assessment) score of 2 or more of the following: 1) respiratory rate
of 22/min or more; 2) altered mentation; 3) systolic BP of 100 mmHg or less.
Septic Shock is defined as sepsis plus need for vasopressor to increase MAP to >
65 mmHg and lactate >2mmol (18 mg/dL)
A. Sepsis, Non-Neutropenic
SOURCE IS UNCLEAR
Preferred Regimen:
1st line: 2nd line:
Piperacillin-tazobactam 4.5g IV q6-8h Meropenem 1g IV q8h PLUS
PLUS Vancomycin 25-30mg/kg loading Vancomycin 25-30mg/kg loading
dose then 1g IV q8h dose then 1g IV q8h
8 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Comments:
Do source control, if possible. Intravenous antibiotics should be given as soon as
sepsis or septic shock is recognized and within the 1st hour. Initial fluid
resuscitation of crystalloid at 30ml/kg should be given in first 3 hours. Target MAP
to >65 mmHg in patients receiving vasopressors. Appropriate routine
microbiologic cultures (including blood) be obtained before starting antimicrobial
therapy in patients with suspected sepsis or septic shock if doing so results in no
substantial delay in the start of antimicrobials
SUSPECT INTRA-ABDOMINAL SOURCE
Etiology: Aerobic and anaerobic gram-negative bacilli
Preferred Regimen:
1st line: Piperacillin-tazobactam 4.5 g IV q8-6h
2nd line: Ceftriaxone 2g IV q12h PLUS Metronidazole 1g loading dose then 500mg
IV q6h or 1g IV q12h OR
Ciprofloxacin 400mg IV q12h or Levofloxacin 750mg IV q24h PLUS
Metronidazole 1g loading dose then 500mg IV q6h or 1g IV q12h
SUSPECT, URINARY TRACT INFECTION
Etiology: Aerobic Gram-negative bacilli (E. coli), Enterococcus species
Preferred Regimen:
1st line: 2nd line:
Piperacillin-tazobactam 4.5g IV q8-6h Ceftriaxone 1g IV q24h OR
Ertapenem 1g IV q24h
Comments:
Base recommendation on local/ hospital antibiogram results. Always assess for
risk factors for antibiotic resistance (e.g. ESBL production because of prior
fluoroquinolone use). Use Ertapenem if with risk for antibiotic resistance.
SUSPECT COMMUNITY-ACQUIRED PNEUMONIA (See treatment of high risk
pneumonia)
SUSPECT ILLICIT IV DRUG USE SOURCE
Etiology: Preferred Regimen:
S. aureus Vancomycin 25-30mg/kg loading dose then 1g IV
q8h PLUS Piperacillin-tazobactam 4.5g IV q8-6h
National Antibiotic Guidelines 9
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
SUSPECT MENINGOCOCCEMIA
Etiology: Preferred Regimen:
N. meningitides Ceftriaxone 2g IV q12h
SEPTIC SHOCK, POST SPLENECTOMY
Preferred Regimen: Comments:
Ceftriaxone 2g IV q12h Increase dose if considering meningitis
STAPHYLOCOCCAL TOXIC SHOCK
Preferred Regimen: Comments:
Vancomycin 25-30mg/kg loading Note: Intravenous Immunoglobulin has
dose then 1g IV q8h PLUS the potential to neutralize super antigen
Clindamycin 900mg IV q8h PLUS and to mitigate subsequent tissue
IVIG 1g/kg d1 then 500mg/kg/d for damage
2-3d
STREPTOCOCCAL TOXIC SHOCK
Preferred Regimen:
1st line 2nd line
Penicillin G 24 MU/d IV in 4-6 div Ceftriaxone 2g IV q24h PLUS
doses PLUS Clindamycin 900mg IV q8h PLUS
Clindamycin 900mg IV q8h IVIG 1g/kg on d1 then 500mg/kg on d2-3
If with Penicillin allergy: Clindamycin 900mg IV q8h PLUS Vancomycin 25-
30mg/kg loading dose then 1g IV q8h. Also start IVIG 1g/kg on d1 then 500mg/kg
on d2-3 for patients unresponsive to vasopressor.
DOT is individualized; Min of 14d if with bacteremia.
B. Febrile Neutropenia in Adults
Defined as an oral temperature of >38.3°C or two consecutive readings of >38.0°C
for >1h and an absolute neutrophil count (ANC) of <500/μL, or <1000/μL and
expected to fall below 500/μL over the next 48h. Assess for risk (low or high risk)
of complication for severe disease at presentation of fever.
LOW RISK
Etiology: Gram positive organisms (predominantly coagulase negative
staphylococci and S. aureus), gram negative bacilli; fungal inf. uncommon
10 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Preferred Regimen:
Ciprofloxacin 750mg PO bid or Levofloxacin 750mg PO qd PLUS
Amoxicillin clavulanic acid 625mg tid
Penicillin Allergy: Ciprofloxacin 750mg PO bid or Levofloxacin 750mg PO qd PLUS
Clindamycin 300mg PO q6h
DOT: Until patient is afebrile and absolute neutrophil count >500cells/μl
Comments:
Those with anticipated <7 days of neutropenia, no medical co-morbidities, and no
significant liver or renal dysfunction, able to take oral medications. Empiric
antibiotic Rx should be started as soon as possible after taking blood cultures. A
fluoroquinolone (FQ) should not be used in patients given a FQ-based antibacterial
prophylaxis. Instead an IV regimen as recommended for high risk patients should
be administered. GCSFs are not routinely recommended as an adjunct to antibiotic
Rx.
HIGH RISK
Etiology: Gram positive (staph, strep, enterococci) and gram-negative bacteria w/
GNB (e.g. P. aeruginosa) causing the more serious infections; fungi (esp. Candida
and Aspergillus)
Preferred Regimen:
Initial therapy for fever Monotherapy with:
Cefepime 2g IV q8h or Meropenem 1-2g IV q8h or
Piperacillin-tazobactam 4.5g IV q6h
PLUS Aminoglycoside or Fluoroquinolone or Vancomycin if with suspected
central line infection, severe mucositis, skin and soft tissue infection, pneumonia,
hypotension
PLUS Antifungal treatment if fever continues beyond 4-7d and no source is
identified
DOT should be dictated by particular organism and site:
Staphylococcus bacteremia should be treated for at least 2 weeks after negative
blood culture; prolonged (4-6 weeks) if disseminated or deep infection. Other
infections may be treated for 14 days. In patients with unexplained fever, initial
regimen should be continued until marrow recovery
Comments:
Those with profound neutropenia of <100 cells/μl and anticipated fever >7days
and/or significant medical comorbidities, hemodynamic instability, hepatic or
renal insufficiency, uncontrolled or progressive cancer, pneumonia or other
complex infections, mucositis grade 3 or 4, new onset neurologic/mental changes,
National Antibiotic Guidelines 11
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
IV catheter infection, inpatient status at time of development of fever, and GI
symptoms. These patients should be admitted in the hospital.
Empiric antibiotic Rx should be started ASAP after blood cultures. Continue
treatment until patient is afebrile and absolute neutrophil count is >500 cells
(some >1000 cells). Modifications to the initial antibiotic regimen should be guided
by clinical and microbiologic data. Use of CSF is controversial; may be considered
in the presence of serious infectious complications such as progressive course,
pneumonia, and invasive fungal infection.
ANTIBACTERIAL PROPHYLAXIS
For high risk patients with expected duration of neutropenia of > 7 days and ANC
≤100 cells/mm3
Preferred Regimen:
1st line 2nd line
Levofloxacin 500-750mg PO/IV qd Ciprofloxacin 500-750mg PO or 400mg
IV q12h
Comments:
Not routinely recommended for low risk patients.
ANTICANDIDAL PROPHYLAXIS
Etiology: Preferred Regimen:
Allogeneic hematopoietic stem cell Fluconazole 400mg IV/PO q24h OR
transplant (HSCT) recipients, acute Micafungin 150mg/d IV OR
leukemia undergoing intensive Itraconazole 200mg PO bid
remission - induction or salvage DOT: until recovery of neutropenia
therapy. For high risk patients with
expected duration of neutropenia of
>7d and ANC≤ 100 cells/mm3
ANTI-ASPERGILLUS PROPHYLAXIS
Etiology: Preferred Regimen:
Patients undergoing chemotherapy Voriconazole 200mg PO/IV bid OR
for AML/MDS with neutropenia and Posaconazole 200mg PO tid for
allogeneic HSCT recipients patients ≥13 years of age
Comments:
Prophylaxis against aspergillus infection in pre-engraftment allogeneic or
autologous transplant recipients has not been shown to be efficacious
12 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
ANTIVIRAL PROPHYLAXIS
Etiology: Preferred Regimen:
HSV seropositive patients undergoing Aciclovir 800mg PO bid OR
allogeneic HSCT or induction for acute Aciclovir 400mg PO tid-qid
leukemia
III. TYPHOID FEVER
UNCOMPLICATED TYPHOID FEVER
Preferred Regimen:
1st line 2nd line
PEDIATRICS
Amoxicillin 75-100mg/kg/d q8h x 14d Cefixime 15-20mg/kg/d q12h x 7-
(Max: 500mg 2 caps q6h) OR 10d (Max: 200mg 1 tab q12h) OR
Ampicillin 100-200mg/kg/d IV q6h x 14d Azithromycin 20mg/kg/d q24h x 5-
(Max: 12g/24h) OR 7d (Max: 500mg 1-2 tabs q24h) OR
Chloramphenicol 50-75mg/kg/d q6h x Ciprofloxacin 30mg/kg/d q12h x 7-
14-21d (Max: 500mg 2 caps q6h) OR 10d (Max: 500mg 1 tab q12h)
TMP-SMX 8mg/kg/d (TMP component)
q12h x 14d (Max: 160/800mg 1 tab
q12h)
ADULTS
Amoxicillin 1g q6h x 14d OR Cefixime 200mg PO q12h x 7- 10d
TMP-SMX 800/180mg I tab q12h x 14d OR
OR Chloramphenicol 1g PO q6h x 14d Azithromycin 500mg-1g PO qd x 5-
OR Ciprofloxacin 500mg 1 tab q12h x 7d
7-10d
Comments:
Based on ARSP 2015, Salmonella typhi remained susceptible to the 1st line agents
like ampicillin, chloramphenicol & TMP-SMX. The use of second line antibiotics
should be reserved for suspected or proven Multi-drug resistant typhoid fever
(MDRTF). MDRTF is defined as typhoid fever caused by Salmonella typhi strains
which are resistant to the first-line recommended drugs for treatment namely
chloramphenicol, ampicillin and TMP-SMX.
MDRTF should be suspected in any of the following situations:
• Failure to respond after 5-7 days treatment with a first line antibiotic;
• Household contact with a documented case or during an epidemic of
MDRTF; and/or
National Antibiotic Guidelines 13
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
• Clinical deterioration or development of complications during conventional
antibiotic treatment
Serious and fatal blood dyscrasias (aplastic anemia, hypoplastic anemia,
thrombocytopenia and granulocytopenia) are known to occur after the
administration of chloramphenicol. An irreversible type of marrow depression
leading to aplastic anemia with a high rate of mortality may occur after short or
long-term use of chloramphenicol.
Ciprofloxacin is not recommended for pregnant women. It can be used among
children if the benefits outweigh the potential harms. High–dose parenteral
Ampicillin can be used if fluoroquinolone is not well tolerated.
Stepping down to an oral antibiotic may be done if patient is afebrile for 48hrs and
is able to tolerate oral medications. De-escalation to oral antibiotics should be
based on results of culture and sensitivity if available.
SEVERE/COMPLICATED TYPHOID FEVER
(Gastrointestinal bleeding, intestinal perforation, typhoid encephalopathy, etc.)
Preferred Regimen:
1st line Step down antibiotics
PEDIATRICS
Ceftriaxone 75mg/kg/d IV q24h x 10- Cefixime 15-20mg/kg q12h x 7-10d
14d (Max: 2-3g q24h) OR (Max: 200mg 1 tab q12h) OR
Ciprofloxacin 30mg/kg/d q12h x 7-10d Azithromycin 20mg/kg q24h x 5-7d
(Max: 500mg/dose q12h) OR (Max: 500mg 1-2 tabs q24h) OR
Azithromycin 20mg/kg/d IV q24h x 5- Ciprofloxacin 30mg/kg q12h x 7-
7d (Max: 1g q24h) 10d (Max: 500mg 1 tab q12h)
ADULTS
Ceftriaxone 1-2g IV x 10-14d OR Cefixime 200mg 1tab q12h x 7-10d
Ciprofloxacin 400mg IV q12h x 7-10d OR Azithromycin 500mg 1-2tabs
q24h x 5-7d OR
Ciprofloxacin 500mg 1tab q12h x
7-10d
CHRONIC CARRIER
Defined as asymptomatic shedding of typhoidal S. enterica for 1 year or more
14 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Preferred Regimen:
1st line 2nd line
PEDIATRICS
Ciprofloxacin 30mg/kg/d q12h x 4 Ampicillin 100-200mg/kg/d IV q6h x
weeks (Max: 1-1.5g/d) 4 weeks (Max: 12g/d)
ADULTS
Ciprofloxacin 500-750mg q12h PO x
28d
NONTYPHOIDAL SALMONELLOSIS (Salmonella gastroenteritis)
Preferred Regimen:
1st line 2nd line
Cefotaxime 100-200 mg/kg/d IV q6h Ciprofloxacin 10-20 mg/kg/d q12h x
x 5-14d (Max: 8-12 g/d) OR 7-10d (Max:1-1.5g/d) OR
Ceftriaxone 75 mg/kg/d IV q24h x7d Chloramphenicol 50-75 mg/kg/d
(Max: 2-4 g/d) OR q6h x 7d (Max: 2-4 g/d)
Cefixime 15 mg/kg/d PO q12h x 7-10d
(Max: 400mg/d)
EXTRA-INTESTINAL INFECTIONS (bacteremia, meningitis, osteomyelitis)
Etiology: Preferred Regimen:
N. meningitides Ceftriaxone 100 mg/kg/d IV q12-24h (Max: 2-
4g/d)
DOT: Bacteremia: 10-14d; Meningitis: 4 weeks; Osteomyelitis: 4-6 weeks
Comments:
Antibiotics are not generally recommended for the treatment of uncomplicated
Salmonella gastroenteritis because they may suppress normal intestinal flora and
prolong both the excretion of Salmonella and the remote risk for creating the
chronic carrier state. Indications for antibiotic treatment include any of the
following:
• Neonates and young infants (≤3 • Hemolytic anemia, including sickle
months old) cell disease, malaria, and
• HIV/AIDS bartonellosis
• Other immunodeficiencies and • Collagen vascular disease
chronic granulomatous disease • Inflammatory bowel disease
• Immunosuppressive and • Achlorhydria or use of antacid
corticosteroid therapies medications
• Malignancies, especially leukemia • Impaired intestinal motility
and lymphoma • Schistosomiasis, malaria
• Malnutrition
National Antibiotic Guidelines 15
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Based on ARSP 2015, nontyphoidal Salmonella is also susceptible to
chloramphenicol & ciprofloxacin. Antibiotics should be revised depending on the
susceptibility pattern.
IV. LEPTOSPIROSIS
Suspected leptospirosis case:
• Fever of at least 2d; AND
• Either residing in a flooded area or has high-risk exposure (wading in floods and
contaminated water, contact with animal fluids, swimming in flood water or
ingestion of contaminated water with or without cuts or wounds); AND,
• At least two of the following: myalgia, calf tenderness, conjunctival suffusion,
chills, abdominal pain, headache, jaundice or oliguria
MILD LEPTOSPIROSIS:
A suspected case of leptospirosis with:
• Stable vital signs • NO evidence of meningismus/ meningeal
• Anicteric sclerae irritation, sepsis/ septic shock, difficulty of
• Good urine output breathing, jaundice
• Can take oral medications
Preferred Regimen:
1st line 2nd line
<8 yo: Amoxicillin 50mg/kg q8h x 7d Azithromycin 1g loading dose then 10
(Max: 500mg q8h) mg/kg qd x 2d (Max: 500 mg/d)
≥8 yo: Doxycycline 2-4mg/kg/d bid x
7d (Max: 200mg/d)
Comments:
Precautions for doxycycline: children <8 years, pregnancy, interaction with birth
control pills, photosensitivity, diarrhea, GI upset and interaction if co-administered
with iron, supplements, statins, other antibiotics and laxatives. Take doxycycline
with food or after a meal.
MODERATE TO SEVERE LEPTOSPIROSIS:
A suspected case of leptospirosis with:
• Unstable vital signs • Meningismus/ meningeal irritation
• Jaundice/ icteric sclerae • Sepsis/ septic shock
• Abdominal pain • Altered mental states or difficulty of
• Nausea, vomiting and diarrhea breathing
• Oliguria/anuria • Hemoptysis
16 National Antibiotic Guidelines
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
Preferred Regimen:
1st line 2nd line
Penicillin 250,000-400,000 U q4-6h Ampicillin 100 mg/kg q6h x 7d
x 7d (Max: 1.5 MU q6-8h) (Max: 0.5-1.0 g q6h) OR
Cefotaxime 100-150 mg/kg q6-8h x 7d
(Max: 1g q6h) OR
Ceftriaxone 80-100 mg/kg q24h x 7d
(Max: 2g q24h) OR
Azithromycin 500mg qd x 5d
Comments:
Step-down therapy can be instituted once patient is clinically stable and bale to
tolerate oral medication. Any oral antibiotic under mild leptospirosis can be
selected.
ANTIBIOTIC PROPHYLAXIS
Pre-exposure prophylaxis - not routinely recommended except for travelers,
soldiers, those engaged in water-related recreational and occupational activities
in highly endemic areas.
Post-exposure prophylaxis depends on type of risk.
Preferred Regimen:
1st line 2nd line
Doxycycline 4mg/kg x 1 dose Amoxicillin 50mg/kg/d q8h x 3-5d
(Max: 200mg regardless of age) (Max: 500mg q8h) OR
Azithromycin 10mg/kg x 1 dose
Take 100mg bid if 200 mg qd is not (Max: 500 mg)
tolerated. If children are exposed for more than
7d, the dose should be repeated after 1
week.
Comments:
The most effective preventive measure is avoidance of high-risk exposure. If
unavoidable, use protective measures such as boots, goggles, over-alls, and rubber
gloves. Antibiotic prophylaxis not 100% effective; protective measures should still
be used. Post-exposure doses may be repeated once weekly if with continued
exposure to risk factors (e.g. staying in a constantly flooded area)
National Antibiotic Guidelines 17
BLOOD-BORNE INFECTIONS AND OTHER SYSTEMIC
SYNDROMES
REFERENCES:
• Ahmed NM, et al. Fever in children with chemotherapy –induced neutropenia. Available
at: http://www.uptodate.com/contents/fever-in-children-with-chemotherapy-induced-
neutropenia.
• American Academy of Pediatrics, In: Kimberlin DW, Brady MT, et al.eds. Red Book 2015
Report of the Committee on Infectious Diseases,30th ed. Elk Grove Village.2015
• Antimicrobial Resistance Surveillance Program. Manila: Department of Health; 2015
• Bradley JS, et al. Intravenous ceftriaxone and calcium in the neonate: assessing the risk for
cardiopulmonary adverse events. Pediatrics.2009;123 (4): e609-e613.
• Cherry JD, Harrison GJ, Kaplan SL, Steinbach WJ, Hotez PJ. Feigin and Cherry’s Textbook of
Pediatric Infectious Diseases. Philadelphia: Elsevier Inc., 2014.
• Dellinger RP, et al. Surviving Sepsis Campaign: International Guidelines for Management of
Severe Sepsis and Septic Shock: 2012. Available at: www.ccmjournal.org.
• Emma Lappin et al. Gram positive toxic shock syndrome. The Lancet Infectious Dis. 9 (5):
May 2009.
• Freifeld A, et al. Clinical Practice Guideline for the Use of Antimicrobial Agents in
Neutropenic Patients with Cancer: 2010 Update by the Infectious Diseases Society of
America. Clin Infect Dis. 2011 Feb 15;52(4): e56-93.
• Integrated Management of Childhood Illness Chart Booklet. Geneva: World Health
Organization; March 2014
• Kliegman RM, et al., eds. Nelson Textbook of Pediatrics. 20th ed. Philadelphia, PA: Elsevier,
2016.
• Pediatric Infectious Diseases Society of the Philippines. PIDSP Core Group
Recommendation: Clinical Practice Guidelines on Childhood Leptospirosis 2015. Quezon
City: PIDSPI; 2015.
• Pediatric Infectious Diseases Society of the Philippines. Post-Disaster Interim Advice on the
Prevention of Leptospirosis in Children 2012. Quezon City: PIDSPI; 2012.
18 National Antibiotic Guidelines
You might also like
- Pediatric Antibiotic Dosing Card 2012Document2 pagesPediatric Antibiotic Dosing Card 2012yoshilimsiacoshigyoNo ratings yet
- E A G - SCH: Mpiric Ntibiotic UidelinesDocument6 pagesE A G - SCH: Mpiric Ntibiotic UidelinesPulseWangminNo ratings yet
- NAG Central Nervous System Infections As of Nov 2017Document9 pagesNAG Central Nervous System Infections As of Nov 2017Rhod Bernaldez EstaNo ratings yet
- NAG Urinary Tract InfectionsDocument14 pagesNAG Urinary Tract InfectionsJun JimenezNo ratings yet
- Empiric Antibiotic Guidelines For Paediatric Intensive Care Unit (PICU)Document7 pagesEmpiric Antibiotic Guidelines For Paediatric Intensive Care Unit (PICU)Benny Chris TantoNo ratings yet
- Champ Empiric Antimicrobial Guidelines: Consider Investigation and Treatment For Pertussis And/Or Chlamydia TrachomatisDocument2 pagesChamp Empiric Antimicrobial Guidelines: Consider Investigation and Treatment For Pertussis And/Or Chlamydia TrachomatistynNo ratings yet
- Icu Antibiotic GuidelinesDocument4 pagesIcu Antibiotic GuidelinesTia MonitaNo ratings yet
- NAG Upper Respiratory Tract InfectionsDocument20 pagesNAG Upper Respiratory Tract InfectionsJun JimenezNo ratings yet
- DRUG DOSAGES For ChildrensDocument8 pagesDRUG DOSAGES For ChildrensAsadullah RawabNo ratings yet
- Cefotaxime 1Document3 pagesCefotaxime 1DidikNo ratings yet
- DOSES FOR SMALL ANIMALS: KEY MEDICATIONS FOR RABBITS, RODENTS, REPTILES AND BIRDSDocument14 pagesDOSES FOR SMALL ANIMALS: KEY MEDICATIONS FOR RABBITS, RODENTS, REPTILES AND BIRDSBruna MoreiraNo ratings yet
- Stanford Hospital & Clinics Antimicrobial Dosing Reference Guide 2013Document3 pagesStanford Hospital & Clinics Antimicrobial Dosing Reference Guide 2013SANCHOSKYNo ratings yet
- Guidelines For First-Line Empirical Antibiotic Therapy in AdultsDocument1 pageGuidelines For First-Line Empirical Antibiotic Therapy in AdultsAnonymous s4yarxNo ratings yet
- ConnectorDocument4 pagesConnectoryetaung8No ratings yet
- Final Anti TB in SP - SituationDocument50 pagesFinal Anti TB in SP - SituationAbdul JalilNo ratings yet
- GentamiciniDocument11 pagesGentamiciniBenjie SisonNo ratings yet
- Antibiotic DosingDocument2 pagesAntibiotic Dosingscohen1No ratings yet
- Meningitis in ChildrenDocument30 pagesMeningitis in ChildrenPNVRSNo ratings yet
- Quick NOteDocument7 pagesQuick NOteAuni Akif Aleesa100% (1)
- Dosi S Anti Mi Kroba: Nama Obat Dosis Dewasa Dosis Anak KETDocument7 pagesDosi S Anti Mi Kroba: Nama Obat Dosis Dewasa Dosis Anak KETBaja Putra HasibuanNo ratings yet
- Vancomycin & Vancomycin Resistant Enterococci: Abdullah M. Kharbosh, B.SC., PharmDocument78 pagesVancomycin & Vancomycin Resistant Enterococci: Abdullah M. Kharbosh, B.SC., Pharmkharbosham100% (1)
- Prevention SepsisDocument25 pagesPrevention SepsisckNo ratings yet
- Drug Doses12Document45 pagesDrug Doses12Asghar Shah100% (1)
- Idiot NotesDocument53 pagesIdiot NotesRay PerezNo ratings yet
- Medicine RotatationbookletDocument20 pagesMedicine RotatationbookletJanelle JosephsNo ratings yet
- Lecture 11. Acute and Chronic Glomerulonephritis, Pediatric HypertensionDocument30 pagesLecture 11. Acute and Chronic Glomerulonephritis, Pediatric HypertensionkrisnadewirahadiNo ratings yet
- Treatment of Malaria RenjithDocument10 pagesTreatment of Malaria RenjithRenjith IndrajithNo ratings yet
- Case Presentation On:: Rheumatoid Arthritis With Newly Diagnoised Steroid Related DM With Systemic HypertensionDocument12 pagesCase Presentation On:: Rheumatoid Arthritis With Newly Diagnoised Steroid Related DM With Systemic HypertensionSamyuktaNo ratings yet
- CURB-65 A 7mmol (19mg/dl) BP 65: CURB-65, PSI, CPIS & AntibioticDocument3 pagesCURB-65 A 7mmol (19mg/dl) BP 65: CURB-65, PSI, CPIS & AntibioticfaberNo ratings yet
- Pedia HandoutsDocument5 pagesPedia HandoutskevincouslandNo ratings yet
- Common Tropical Disease in ThailandDocument84 pagesCommon Tropical Disease in ThailandDr.Sathaporn KunnathumNo ratings yet
- COVID-19 Protocol KGMU Version 6.0 17-4-21Document34 pagesCOVID-19 Protocol KGMU Version 6.0 17-4-21Kirtivaan MishraNo ratings yet
- AntibioticsDocument13 pagesAntibioticsJOrgeNo ratings yet
- PEDIATRIC GROWTH CHART AND DRUG DOSING REFERENCEDocument9 pagesPEDIATRIC GROWTH CHART AND DRUG DOSING REFERENCEjandale100% (1)
- Gestational Diabetes MellitusDocument22 pagesGestational Diabetes MellitusNadia AgagonNo ratings yet
- 05 Paeds Drug Doses-1Document4 pages05 Paeds Drug Doses-1JunaidahMubarakAliNo ratings yet
- The Drug Doses in The Following Pages Are ReproducDocument168 pagesThe Drug Doses in The Following Pages Are ReproducAsghar ShahNo ratings yet
- Empiric Treatment Guidelines Common InfectionsDocument9 pagesEmpiric Treatment Guidelines Common InfectionsShiza Batool100% (1)
- Antibiotic Dosing Guidelines For Renal ImpairmentDocument6 pagesAntibiotic Dosing Guidelines For Renal ImpairmentvitauxianaNo ratings yet
- Paediatricshouseofficerguidehospitalkulim 151026150042 Lva1 App6891Document14 pagesPaediatricshouseofficerguidehospitalkulim 151026150042 Lva1 App6891Nadia SalwaniNo ratings yet
- Profil Ampicillin SulbactamDocument12 pagesProfil Ampicillin SulbactamasriNo ratings yet
- Drug HandBookDocument10 pagesDrug HandBookAhmed FekryNo ratings yet
- Aminoglycoside & Vancomycin: Basic TDMDocument57 pagesAminoglycoside & Vancomycin: Basic TDMft84nzzc92No ratings yet
- Laboratory Tests for Diabetes Diagnosis and ManagementDocument48 pagesLaboratory Tests for Diabetes Diagnosis and ManagementBababo StopNo ratings yet
- Central Nervous System InfectionsDocument9 pagesCentral Nervous System InfectionsSaddamNo ratings yet
- Dr. Paulus Novian Harijanto, SPPD, K-PTI, FINASIM-Management Malaria in SepsisDocument30 pagesDr. Paulus Novian Harijanto, SPPD, K-PTI, FINASIM-Management Malaria in SepsisOlivia DwimaswastiNo ratings yet
- MPProtocols 380Document1 pageMPProtocols 380Indrawathan SamyNo ratings yet
- Terapi AnakDocument10 pagesTerapi AnakIka KrastanayaNo ratings yet
- Pediatric Drug Dosage - All in One PDFDocument15 pagesPediatric Drug Dosage - All in One PDFHuang Hasjim33% (9)
- NAG Sexually Transmitted InfectionsDocument24 pagesNAG Sexually Transmitted InfectionsJun JimenezNo ratings yet
- Role of DHA in Paediatric NutritionsDocument67 pagesRole of DHA in Paediatric NutritionsSIROY LIFE SCIENCESNo ratings yet
- Paediatric Anaesthesia GuideDocument1 pagePaediatric Anaesthesia GuideAndrewBeckNo ratings yet
- MALARIA DR - PAULDocument67 pagesMALARIA DR - PAULNodi Rahma DiniNo ratings yet
- PCCU Dosing Handbook 2009 PDFDocument53 pagesPCCU Dosing Handbook 2009 PDFTyrone PooleNo ratings yet
- AnestesiDocument61 pagesAnestesiJack Kings QueenNo ratings yet
- Renal Dosing2Document3 pagesRenal Dosing2Mohammed IbrahimNo ratings yet
- Metronidazole: Antibiotic Class: Antimicrobial SpectrumDocument4 pagesMetronidazole: Antibiotic Class: Antimicrobial SpectrumChinedu H. DuruNo ratings yet
- Physiology for General Surgical Sciences Examination (GSSE)From EverandPhysiology for General Surgical Sciences Examination (GSSE)S. Ali MirjaliliNo ratings yet
- HGVSJDocument2 pagesHGVSJRhod Bernaldez EstaNo ratings yet
- 2nd Patient Safety Congress RegistrationDocument1 page2nd Patient Safety Congress RegistrationRhod Bernaldez EstaNo ratings yet
- Statistics PDFDocument54 pagesStatistics PDFRhod Bernaldez EstaNo ratings yet
- Erastus Perceptions 2018 PDFDocument105 pagesErastus Perceptions 2018 PDFRhod Bernaldez EstaNo ratings yet
- Grenada History, Geography, Politics and EconomyDocument2 pagesGrenada History, Geography, Politics and EconomyRhod Bernaldez EstaNo ratings yet
- Official Receipt PDFDocument1 pageOfficial Receipt PDFRhod Bernaldez EstaNo ratings yet
- Carrebean SeaDocument7 pagesCarrebean SeaRhod Bernaldez Esta100% (1)
- Radically Redesigning: Patient SafetyDocument9 pagesRadically Redesigning: Patient SafetyRhod Bernaldez EstaNo ratings yet
- Patient Safety in Primary Healthcare A Review of The Literature August 2015Document160 pagesPatient Safety in Primary Healthcare A Review of The Literature August 2015Rhod Bernaldez EstaNo ratings yet
- NursingDocument1 pageNursingRhod Bernaldez EstaNo ratings yet
- Patient Safety Culture in Primary Care: Natasha VerbakelDocument176 pagesPatient Safety Culture in Primary Care: Natasha VerbakelRhod Bernaldez EstaNo ratings yet
- Patient Safety Incident Reporting - Canadian Health SystemDocument13 pagesPatient Safety Incident Reporting - Canadian Health SystemRhod Bernaldez EstaNo ratings yet
- Leadership DevelopmentDocument2 pagesLeadership DevelopmentRhod Bernaldez EstaNo ratings yet
- RHOD Seniority Complex Semi FinalDocument39 pagesRHOD Seniority Complex Semi FinalRhod Bernaldez EstaNo ratings yet
- Perceive/observe It. Please Answer All Items On This Sheet. If An Item Is Irrelevant, or IfDocument3 pagesPerceive/observe It. Please Answer All Items On This Sheet. If An Item Is Irrelevant, or IfRhod Bernaldez EstaNo ratings yet
- Gardner-Webb University Digital Commons at Gardner-Webb UniversityDocument132 pagesGardner-Webb University Digital Commons at Gardner-Webb UniversityRhod Bernaldez EstaNo ratings yet
- Sops Hospital Survey: Language: EnglishDocument6 pagesSops Hospital Survey: Language: EnglishNoviyanti LindaNo ratings yet
- AHRQ Patient Safety Culture Improvement PlanDocument4 pagesAHRQ Patient Safety Culture Improvement PlanRhod Bernaldez EstaNo ratings yet
- Icrd Vawc-1Document1 pageIcrd Vawc-1Rhod Bernaldez EstaNo ratings yet
- Facil Scan FormDocument7 pagesFacil Scan FormJoe ThesecondmonthNo ratings yet
- Relationship Between Patient Safety Culture and Safety Outcome Measures Among NursesDocument80 pagesRelationship Between Patient Safety Culture and Safety Outcome Measures Among NursesRhod Bernaldez EstaNo ratings yet
- Implementing Rules and Regulations of The Lending Company Regulation Act of 2007 Ra9474Document19 pagesImplementing Rules and Regulations of The Lending Company Regulation Act of 2007 Ra9474Lance DionelaNo ratings yet
- Fallpxtool 1 BDocument2 pagesFallpxtool 1 BRhod Bernaldez EstaNo ratings yet
- MHD Mission VisionDocument1 pageMHD Mission VisionRhod Bernaldez EstaNo ratings yet
- Nurses' Perceptions of Patient Safety Culture in Oman: Fatma Al Dhabbari MSC, Pgd. BSC (Hons), R.G.NDocument3 pagesNurses' Perceptions of Patient Safety Culture in Oman: Fatma Al Dhabbari MSC, Pgd. BSC (Hons), R.G.NRhod Bernaldez EstaNo ratings yet
- Perceived Safety Culture of Healthcare Providers in Hospitals in The PhilippinesDocument14 pagesPerceived Safety Culture of Healthcare Providers in Hospitals in The PhilippinesRhod Bernaldez EstaNo ratings yet
- Objectives 2. Scope 3. Responsibilities 4. Records and References 5. Procedure Details Page No. Rev. No. Effectivity Nature of ChangeDocument8 pagesObjectives 2. Scope 3. Responsibilities 4. Records and References 5. Procedure Details Page No. Rev. No. Effectivity Nature of ChangeRhod Bernaldez EstaNo ratings yet
- Leadership DevelopmentDocument2 pagesLeadership DevelopmentRhod Bernaldez EstaNo ratings yet
- Control of Documented Information Procedure SampleDocument4 pagesControl of Documented Information Procedure Sampleingventor0% (1)
- NursingDocument1 pageNursingRhod Bernaldez EstaNo ratings yet
- WSO Global Stroke Fact SheetDocument15 pagesWSO Global Stroke Fact SheetPentolNo ratings yet
- Physiotherapy Treatment ScarsDocument3 pagesPhysiotherapy Treatment ScarsYuyun Aryuni MusrifNo ratings yet
- GBS IntroDocument2 pagesGBS IntroEula Angelica OcoNo ratings yet
- Pathophysiology of BurnDocument3 pagesPathophysiology of Burnuaeb100% (1)
- Airway ManagementDocument42 pagesAirway ManagementKugan KishurNo ratings yet
- Banner HealthcareDocument6 pagesBanner HealthcareValNo ratings yet
- Drugs That Cannot Be Crushed - Ms. HopeDocument4 pagesDrugs That Cannot Be Crushed - Ms. Hopemiggy13No ratings yet
- Skeletal Muscle Relaxants and Neuromuscular Blocking AgentsDocument7 pagesSkeletal Muscle Relaxants and Neuromuscular Blocking AgentsYanyan PanesNo ratings yet
- ACOG The RH Factor How It Can Affect Your Pregnancy PDFDocument3 pagesACOG The RH Factor How It Can Affect Your Pregnancy PDFdoc moNo ratings yet
- Lights and Siren May 2017 Maryn Final2 PDFDocument98 pagesLights and Siren May 2017 Maryn Final2 PDFepraetorian100% (2)
- Anabolic Peptide Beta EbookDocument226 pagesAnabolic Peptide Beta EbookMatei Cipri80% (5)
- UWorld Notes Step 2 CKDocument11 pagesUWorld Notes Step 2 CKSamah Khan50% (2)
- VBI Vaccines - ICAAC Presentation 2014Document12 pagesVBI Vaccines - ICAAC Presentation 2014DougNo ratings yet
- Uterine ProlapseDocument3 pagesUterine ProlapseKeshavprasad kurmi100% (1)
- Chapter 01 Introduction To Nursing PDFDocument7 pagesChapter 01 Introduction To Nursing PDFludwigs43100% (1)
- NCM 109 Reviewer Module 1Document6 pagesNCM 109 Reviewer Module 1tamsmadjad18No ratings yet
- San Jose, Batangas COVID-19 cases updateDocument79 pagesSan Jose, Batangas COVID-19 cases updatema. vidiaNo ratings yet
- Resume-Parimala DeepthiDocument2 pagesResume-Parimala DeepthideeptiNo ratings yet
- Application HFOV in NICU - Lily RundjanDocument43 pagesApplication HFOV in NICU - Lily Rundjandiah ayu pitalokaNo ratings yet
- MSC 1st Yr Unit PlanDocument10 pagesMSC 1st Yr Unit PlanSilja ManojNo ratings yet
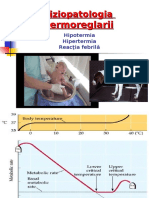
- Documents - MX Fiziopatologia Termoreglarii Fiziopatologia Termoreglarii Hipotermia Hipertermia Reactia Febrila 10-12-2006Document42 pagesDocuments - MX Fiziopatologia Termoreglarii Fiziopatologia Termoreglarii Hipotermia Hipertermia Reactia Febrila 10-12-2006AndreiNo ratings yet
- Discipline Relationship With Surgical Nurse PerformanceDocument16 pagesDiscipline Relationship With Surgical Nurse PerformanceDewi Nur Puspita SariNo ratings yet
- Diabetic Retinopathy Treatment in MumbaiDocument7 pagesDiabetic Retinopathy Treatment in MumbaiCharvi JainNo ratings yet
- Acute Flaccid Paralysis Case Investigation FormDocument2 pagesAcute Flaccid Paralysis Case Investigation FormMurari Rajendraprasad100% (1)
- AIIMS Rajkot Webinar on Sleep & Polysomnography Basics to UpdatesDocument4 pagesAIIMS Rajkot Webinar on Sleep & Polysomnography Basics to Updatesகார்த்திNo ratings yet
- DUOLIN RespulesDocument17 pagesDUOLIN RespulesNakul SharmaNo ratings yet
- CVA - Case ScenarioDocument3 pagesCVA - Case ScenarioHarvey T. Dato-onNo ratings yet
- Manual Resp Carat 2Document96 pagesManual Resp Carat 2jan gutiNo ratings yet
- ChinaDocument57 pagesChinaAsaf NaeemNo ratings yet
- Case Study Patient With CopdDocument54 pagesCase Study Patient With CopdKenneth NuñezNo ratings yet